Chapter 14 ~ The Routine use of Continuous EFM – A Failed Experiment:
The Routine use of Continuous EFM –
A Failed Experiment:
Thirty years of continuous electronic fetal monitoring of all laboring women, combined with the liberal use of cesarean section in the event of even the slightest suspicion of fetal distress, failed to reduce the rate of cerebral palsy and other neurological disabilities.
This is a well-documented fact and widely acknowledged by the obstetrical profession itself. In July of 2003, a report by the American College of Obstetrician and Gynecologists (ACOG) Task Force on Neonatal Encephalopathy & Cerebral Palsy stated:
“Since the advent of fetal heart rate monitoring, there has been no change in the incidence of cerebral palsy.
… The majority of newborn brain injury does not occur during labor and delivery. …. most instances of neonatal encephalopathy and cerebral palsy are attributed to events that occur prior to the onset of labor.”
This report is widely regarded as the “most extensive peer-reviewed document on the subject published to date and has the endorsement of six major federal agencies and professional organizations, including the CDC, the March of Dimes, and the obstetrical profession in Australia, New Zealand, and Canada.
The September 15, 2003 edition of Ob.Gyn.News stated that:
“The increasing cesarean delivery rate that occurred in conjunction with fetal monitoring has not been shown to be associated with any reduction in the CP [cerebral palsy] rate… … Only 0.19% of all those in the study [these diagnosed with CP] had a non-reassuring fetal heart rate pattern….. If used for identifying CP risk, a non-reassuring heart rate pattern would have had a 99.8% false positive rate (N.Engl. J. Med 334[10:613-19, 1996). The idea that infection might play an important role in [CP] development evolved over the years as it became apparent that in most cases the condition cannot be linked with the birth process. ” [emphasis added]
An August 15, 2002 report in Ob.Gyn.News stated that:
“Performing cesarean section for abnormal fetal heart rate pattern in an effort to prevent cerebral palsy is likely to cause as least as many bad outcomes as it prevents. … A physician would have to perform 500 C-sections for multiple late decelerations or reduced beat-to-beat variability to prevent a single case of cerebral palsy.” [emphasis added]
Unfortunately, delayed and downstream complications for mothers and babies that are associated with EFM and the liberal use of Cesarean surgery make this policy counter-productive.
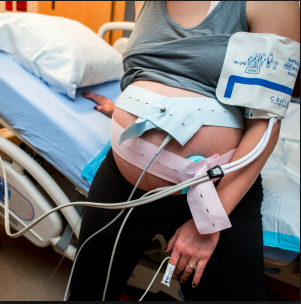
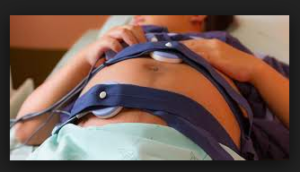
People wrongly assume that EFM is the equivalent of an electrocardiogram (EKG) for the unborn baby, but this is a serious misunderstanding of the technology. Electronic monitoring is simply an elaborate mechanism to count and graphically display the pulse rate of the unborn baby. The machine merely transposes the acoustic signal of heart rate into a printed paper graph and video display, which makes visible the four auditory markers of fetal well-being (baseline heart rate, variability, accelerations, and absence of pathological decelerations).
Listening to the baby with a fetoscope (a special non-electronic stethoscope for listening to fetal heart tones) or an electronic Doptone can provide the same ongoing data (same four markers of wellbeing) of the unborn baby without the interpretive errors by doctors and hospital staff, physical restrictions on the mother, which is to be tethered to her hospital bed, and unrealistic expectations of the public associated with the use of continuous EFM.
Despite a success rate of only 00.2%, most hospitals bill around $400 an hour for continuous EFM. Regularly listening to fetal heart tones with an electronic Doppler for one full minute immediately after a contraction, (called Intermittent auscultation or ‘IA’) permits the same data on the four auditory markers of fetal well-being to be obtained.
While intermittent auscultation is more time-intensive, IA for low and moderate-risk labor is equally as effective as continuous EFM, with the added benefit of a greatly reduced cesarean rate (4% vs. 26%). This is, in part, because it unhooks healthy mothers from machines and permits laboring women to move around freely. No longer tethered to the bed by electronic wires, the mother is able to change positions frequently, walk, use hot showers or deep water for pain relief and make “right use of gravity” These practices reduce fetal distress and the need for Pitocin-augmentation of labor, pain medication, anesthesia, and instrumental and operative delivery.
Increased in Cesarean delivery does NOT reduce urinary incontinence in the childbearing population of women
The other blue elephant in the room that no one is talking about – according to the scientific literature, elective Cesarean surgery isn’t a reliable method to prevent the pelvic floor problems sometimes associated with childbearing; “purple pushing” during 2nd stage labor identified as damaging to the soft tissue of the birth canal; study confirming that traditional upright positions provide the most room for baby to be born normally
Cesareans not safe or effective for preventing pelvic problems: Having debunked the ‘prophylactic’ use of Cesarean to prevent cerebral palsy in babies, elective C-section is now being promoted as a prophylactic procedure to eliminate pelvic floor problems later in the woman’s life. However, reputable research also does not support the use of elective Cesarean surgery as either a safe or a reliable method to achieve this goal.
In an article entitled “Elective Cesarean Section: An Acceptable Alternative to Vaginal Delivery?”, Dr Peter Bernstein, MD, MPH, Associate Professor of Clinical Obstetrics & Gynecology and Women’s Health at the Albert Einstein College of Medicine, reported on the failure of the obstetrical profession to practice evidence-based medicine as it applies to this topic. Addressing the popular notion that pelvic floor damage and incontinence were the inevitable result of normal birth (to which cesarean surgery was the proposed remedy), Dr Bernstein observed:
“…these adverse side effects may be more the result of how current obstetrics manages the second [pushing] stage of labor. Use of episiotomy and forceps has been demonstrated to be associated with incontinence in numerous studies. Perhaps also vaginal delivery in the dorsal lithotomy position [lying flat on the back] with encouragement from birth attendants to shorten the second stage with the Valsalva maneuver [prolonged breath-holding], as is commonly practiced in developed countries, contributes significantly to the problem.”
A guest editorial published in Ob.Gyn.News; August 1, 2002 by Dr. Elaine Waetjen debunked the idea that elective cesareans can reliably prevent the need for pelvic surgery later in life. She stated that a: “[physicians] would have to do 23 C-sections to prevent one such surgery.”
Non-physiological pushing styles and positions are risky for mother and baby:
Another report in published in Ob.Gyn.News, March 15 2003, councils against “purple pushing”, which is when the mother holds her breath and pushes so long that she temporarily uses up all her oxygen and gets purple in the face. Prolonged pushing of this type can cause tiny blood vessels [capillaries] in the face to break and sometimes blood vessels in the mother’s eyes will rupture, leaving a tell-tale bright red spot in the corner, similar to the damage that accompanies a black eye. The technique that causes this is the Valsalva maneuver, a combination of prolonged breath-holding and “closed-glottis” pushing.
The author, Lisa Miller, CNM, JD is a former labor and delivery nurse, a nurse-midwife and also an attorney. Her report identifies the general idea of ‘directed’ pushing as an undesirable practice that interferes with normal physiology. Directed pushing usually means the mother is being coached by the doctor or labor room nurse to hold her breath to a count of ten and push as long and hard as possible.
This is the familiar scene in which the mother lies in bed on her back, while her husband helps to hold her legs up in the air and with every uterine contraction, the hospital staff exhorts her to push “harder, harder, harder, hold it, hold it, now come on, give it all you’ve got, one more push, come on, just a little longer, we can see a little bit of the baby’s head, don’t waste your contraction, etc”, until the mother is out of breath and purple in the face. This style of “shout it out pushing” is biologically unnecessary and counterproductive for several reasons.
The hospital’s coaching policy assumes the mother’s natural biological urge to push is inadequate or that she wouldn’t know how to push, therefore labor attendants must instruct the mother to hold her breath to a count of ten for three times for each pushing contraction. Purple pushing is uncomfortable, undignified, and, when contrasted with the ‘right use of gravity’, usually counterproductive. It is not recommended by evidence-based studies because it disturbs the oxygen-carbon dioxide balance and causes a dangerous rise in the mother’s blood pressure.
Most regrettably, is an unspoken criticism that somehow the mother isn’t doing it quite “right” or that she isn’t trying quite hard enough. Even more disturbing is the anxiety it introduces into the labor room, which gives everybody in the room the idea that either childbirth is a race with a big prize for the fastest birth or the baby is in serious trouble and the staff is tying to get it out before it dies or they have do a crash C-section. Neither is true for 99.99% of healthy women.
The author states that:
“Long Valsalva’s maneuvers — or “purple pushing”— and standard supine [i.e. lying on one’s back] positioning should be reconsidered. …. Long Valsalva pushing can adversely affect maternal hemodynamics, which in turn adversely affects fetal oxygenation
Purple pushing–or closed-glottis pushing–during which the patient holds her breath for 10 seconds while pushing is safe in the approximately 80% of low-risk pregnancies. But that doesn’t mean it works best … in high-risk cases, the baby can’t tolerate that kind of pushing.
….near-infrared spectroscopy used to evaluate fetal effects revealed that closed glottis and coached pushing efforts led to decreased mean cerebral 02 saturation and increased mean cerebral blood volume. All Apgar scores were below 7 at one minute and below nine at five minutes. [i.e. both are sub-optimal Apgar scores indicating a transient stress on newborn]
Open-glottis pushing, on the other hand, allows the patient to exhale while bearing down and leads to minimal increase in maternal blood pressure and intrathoracic pressure, maintained blood flow, and decreased fetal hypoxia.”
Right and wrong use of gravity:
At a meeting of the Radiological Society of North America, two radiologists from the University Hospital, Zurich, Switzerland described a pelvimetry study using magnetic resonance imaging (MR) to determine which maternal positions provided the most room for the baby to be born.
The study contrasted the conventional supine position (mother lying flat on her back) to positions in which the mother was squatting or an all-fours ‘hands and knees’ position. A report on their presentation, aptly entitled “Upright Positions Offer Most Room for Delivery”, was published in Ob.Gyn.News [2002; Volume 37 • No 3]. They measured the space available for the baby to pass through at the three critical landmarks of the childbearing pelvis –intertuberous diameter, interspinous diameters, and the sagittal outlet. They discovered that upright positions provided an average of slightly more than a centimeter at each of these junctions.
“Upright birthing positions provide significantly more room for delivery in terms of pelvic dimensions, compared with lying supine, Dr. Thomas Keller said. He and his colleagues …who performed MR pelvimetry on 35 non-pregnant women to compare pelvic bony dimensions in the supine, hand-to-knee, and squatting positions.
These differences are statistically significant and confirm the advantages of birthing positions long practiced in other cultures, the study’s coauthor Dr. Rahel Kubik-Huch noted during an interview. [emphasis added]
… the theoretical ideal would thus be to adopt the hand-to-knee position to help the presenting part through the interspinous diameter, and to squat rather than remain supine as the [head] traverses the sagittal outlet, said Dr. Kubik-Huch.”
This silly little centimeter of extra space between lying down and standing up can easily be the difference between a spontaneous vaginal birth with a healthy baby and a difficult one that required unusually long and hard pushing, the use of forceps or vacuum to extract the baby or even a Cesarean section that may leave both mother and baby in need of prolonged or specialized care after the birth. It turns out that the ‘right use of gravity’ during the 1st and 2nd stage of labor is the best way facilitate a normal birth. By avoiding the use of obstetrical forceps or vacuum, the soft-tissue of the mother’s pelvis and the unborn baby’s brain are protected from the damage associated with either prolonged pushing or instrumental deliveries.
This is temporarily the end of this unpublished manuscript
However clicking this link will take you to
a list of links for published studies on EFM as compared to auscultation
EFM –>
associated with a high C-section rate and higher maternal mortality
and morbidity rateCompared to having a real person who listens with a fetascope or
electronic Doppler –>A much lower rate of all
types of interventions and
surgical deliveries!