
Typical labor patient tethered to her bed by EFM cables and intravenous lines, while surrounded by IV poles with various electronic dispensing devices.
Still needs photos
The “Jekyll and Hyde” nature of the obstetrical dilemma
I haven’t worked in a hospital L&D for many years but the nature of the beast, which is based in “controlling the process”, is not all that different today.
It’s still a system in which the use of interventions during labor is the “norm”, only now Twilight Sleep drugs have been replaced by epidural anesthesia and the entire labor now revolves around the “machine that goes “ping” — electronic fetal monitor (EFM) — and giving intravenous Pitocin to speed up the labor, or as the L&D staff often remark: “moving things along”.
I long ago forgave myself for not speaking up when doctors ordered me to do things I knew would be harmful to mothers and babies, such as giving a large and frequently repeated dose of narcotics to a 90-pounds pregnant woman who was just minutes away from giving birth. The likelihood of her baby being respiratory depressed at birth due to drugs I’d just given to its mother was about 90%, and yet I did what the doctor ordered because that is what nurses are supposed to do.
On more than one occasion a particularly unhappy OB who was mad at me for speaking up, which was seen as “questioning his authority” said:
“I make the decisions, I give the orders; it’s not your job to question me, but simply do what I tell you, when I tell you! Is that clear?“
I didn’t let this Faustian bargain make me brain-dead, but found these obstetrical practices so baffling that I started to research them in old obstetrical textbooks donated by retiring obstetricians to our L&D’s small library.
 I’ve always been a curious person and for me that also meant being a “reader”, eager to know what, why and how things come about. I began eagerly studying the history and practice of American obstetrics as it burst on the scene early in the 20th century (1900 to 1910) as a brand-new surgical specialty. This was very different than the historic practice of obstetrics in Western Europe, which was not seen as a surgical discipline.
I’ve always been a curious person and for me that also meant being a “reader”, eager to know what, why and how things come about. I began eagerly studying the history and practice of American obstetrics as it burst on the scene early in the 20th century (1900 to 1910) as a brand-new surgical specialty. This was very different than the historic practice of obstetrics in Western Europe, which was not seen as a surgical discipline.
The stories revealing on historical documents and old OB textbooks was so remarkable that I’ve been reading and studying the issues they presented for the last half century and shamelessly describe myself as the “idiot savant” of the politics and practice of obstetrical medicine in the United States.
Jekyll and Hyde” nature of obstetrics
For the entire 20th century, and now the first two decades of the 21st, maternity care for healthy women has been defined by the individual preferences of obstetricians as a group of doctors trained in Ob-Gyn surgery. While childbirth itself is a personal experience for each individual family, the economics and basic functionality of our maternity care system does not exist in a vacuum.
Unfortunately, the big picture as defined by the number of new healthy women who die before, during or after giving birth in the US is shocking and will convince even the most reluctant reader that this important topic should be part of public discourse and call for our national maternity policies and practices to be reevaluated.
What has baffled me most was the inherent “Jekyll and Hyde” nature of obstetrics.
Obstetricians that attended births in our hospital could be really good doctors one minute, and then a few minutes later do things that were unnecessary and occasioned great harm to either mother or baby or both.
Every obstetrician I knew was willing to jump in to save the life of a laboring woman or her baby from some potentially-deadly obstetrical emergency, then five minutes later that same obstetrician would take a heavily-drugged but normal healthy laboring woman to the delivery room and “perform” a series of unnecessary surgical procedures that included a “generous” episiotomy (!) and forceps to drag a limp, unbreathing baby out of its mother’s inert body. Its poor Apgars and possible death were the result of the high level of drugs and anesthesia given to its mother over the many hours, sometimes days, of labor.
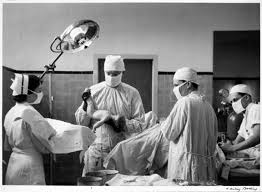
Severely depressed baby (note the floppy head and dangling arms) born to a mother who’d been heavily medicated and then given general anesthesia and was delivered by forceps
Many of these babies were never able to breathe on their own and despite our resuscitative efforts, they were considered “stillborn. This is a grievous experience not only for the parents and extended family, but also for L&D nurses and other hospital staff.
Unfortunately, the nursing staff knew that most of these newborn baby deaths were the result of iatrogenic intervention and virtually 100% preventable.
Obstetrics in America fails to distinguish between healthy childbearing women and those with complications so every patient is treated as potentially high-risk
But the obstetrical system, did not and still does not, distinguish between the two categories of “healthy” (70% to 85%) “high-risk” (15% to 25%). Historically, childbearing women were harmed in many ways by a system that routinely intervened in the labors and birth of all labor patients based on misguided efforts to prevent obstetrical complications by preemptively drugging them and turning normal birth in healthy low-risk women into a series of unnecessary surgical procedures.
During the 20th century — as late as 1980 in our hospital — this meant rendering healthy women unconscious during the ‘delivery’, so it’s mother was one person who was never able to “present” at her baby’s birth!
For reasons I still can’t explain, it never dawned on our OBs that giving birth was very special occasion for the mother, and that women wanted to be awake and fully present when their babies were born.
When my mother-in-law was 93 years old, she was still talking about her extreme disappointment at being been “put to sleep” without her consent when she gave birth to her one and only baby (my husband). She labored at home all day without any particular difficulty and went to the hospital when she started to feel “pushy”. She described how very excited she was when they had her move to a stretcher and wheel her into the delivery room, as she continued to anticipate seeing her baby born, then suddenly and without any prior explanation, everything went black. Several hours later she woke up in her hospital room, feeling empty and being told by the nurse that she had a boy.
Our interventive OB system, the link between EFM, Cesareans and preventable maternal mortality
Obstetrical interventions are nothing short of miracle for childbearing women suffering from a pregnancy or childbirth-related emergency. We are all grateful for ability of obstetrical medicine to successfully treat these complications without loss of life.
But in the United States, many of these same “life-saving” obstetrical interventions — in particular, continuous EFM, induction and Pitocin augmentation of labor and Cesarean surgery — have routinely been used on healthy women with normal pregnancies based on the idea that it made childbirth safer, thus reducing the risk of a malpractice suits for hospitals and doctors. But unfortunately, these risky practices were, and continue to be, responsible for an increasing number of preventable maternal deaths.
Expensive electronic monitoring of unborn babies dramatically increases the rate of emergency C-sections w/o benefitting the baby and it greatly increases the risk to its mother
The single biggest problem in American obstetrics, which is that the United States has the highest maternal mortality rate (MMR) in the developed world — can be traced back to two issues.
- For low-income minority groups the immediate problem is lack of access to high quality maternity care.
- For middle and upper class women the biggest problem is the universal use of continuous electronic fetal monitoring and the role it plays in dramatically increasing the rate of emergency C-sections and the cascade of immediate, delayed and downstream complications associated the repeated use of major abdominal surgery to deliver babies .
It’s not a surprise that the obstetrical profession claims continuous electronic monitoring during labor protects the unborn baby while having no negative effects on the labor or the childbearing woman.
However, the “science” says that isn’t factual. Here is a recently published study that is in direct contradiction:
“An observational study published in the peer-reviewed journal CMAJ in 2019 found women who had C-sections were 80% more likely to have complications than those who delivered vaginally.
Women over the age of 35 who had C-sections were almost three times more likely to have severe complications.”
In a strictly theoretical way, this argument over the role of continuous EFM as the universal ‘standard of care’ in the United States, and the disproportionately high rate of Cesarean surgeries reminds me of the current public discourse about the role of guns in mass shooting and mass casualty events. A majority of American (approx 85%) see a direct association between guns and subsequent gunshot deaths.
However, large minority of American defend the right walk around carrying guns. This second group thinks it’s unfair to blame the gun, and instead blame these deaths on everything other than the actual gun, usually seeing these preventable tragedies to be a consequence of untreated mental illness. But for most of us, we see a direct correlation between taking one or more guns out of your home and using them to randomly shoot at men, women and children!
Quote obviously electronic fetal monitoring has nothing to do with guns, but refusal to “connect up the dots” between the direct effects of a specific action — in this case, performing emergency Cesarean surgery based on a fetal heart rate pattern defined as “non-reassuring” — and all the immediate and downstream complications for the mother is disingenuous on the part of the obstetrical profession as a political entity represented by American College of Obstetricians and gynecologists (ACOG).
Since EFM was first marketed in the 1970s, it’s use is directly associated a dramatic increase in the Cesarean section rate and yet there is no improvement in outcomes for these babies. The very first study of continuous EFM in 1976 compared to regularly listening to the baby’s heart rate with an acoustic fetoscope or hand-held doppler (known as “aus-cul-ta-tion” was a prospective trial published by Dr. Haverkamp et al in 1976.
The study concluded that there were no differences in the infant outcomes in any measured category between the electronically monitored group and the auscultated group (listening with Doppler) except for a dramatic rise in the C-section rate in EFM cohort — from 6% to 16%!
More than a hundred such studies comparing EFM with auscultation (regularly listening to the fetal heart rate and rhythm with a hand-held Doppler) have continue to find the sayhas been
A diagnosis of a “non-reassuring fetal monitor tracing“is the second most frequently cited “reason” for doing a C-section during the labor of a woman having her first baby. Note that a less-than perfectly reassuring tracing is not the same thing as actually identifying profound fetal distress. “Non-reassuring” is nowhere close to “ominous“.
Give such a high rate of maternal complications, some of what are fatal, should make us re-examine the acceptance of the current obstetrical position in regard to Cesarean surgery with its “When in doubt, cut it out” motto. Obstetricians choosing the “intervention” of C-section are playing it ‘safe’, but the object of that supposedly greater safety are obstetrician and hospital administrators, while the burden and complications all fall on these childbearing women. Repeat C-sections are far more risky than the “primary” CS, as a result of the abdominal adhesions that make post-Cesarean surgery much more difficult.
Women who have had a previous CS are are left to bear a lifetime of post-Cesarean complications and their dangers. These mothers are 80% more likely to develop serious intraoperative, post-op, delayed or down stream complications that can include maternal death in a future pregnancy.
The evaluation of continuous fetal heart rate monitoring in high-risk pregnancy☆,☆☆
Abstract
“Intrapartum electronic fetal heart rate monitoring of the high-risk obstetric patient is thought to improve the perinatal outcome.
A prospective randomized study of 483 high-risk obstetric patients in labor was carried out comparing the effectiveness of electronic fetal monitoring with auscultation of fetal heart tones.
The infant outcome was measured by neonatal death, Apgar scores, cord blood gases, and neonatal morbidity (serious medical conditions).
There were no differences in the infant outcomes in any measured category between the electronically monitored group and the auscultated group.
The cesarean section rate was markedly increased in the {electronically} monitored group (16.5 vs. 6.8 per cent in the auscultated patients).
The presumptive benefits of electronic fetal monitoring for improving fetal outcome were not found in this study.”
Transactions of the Forty-third Annual Meeting of
the Central Association of Obstetricians and Gynecologists
Unnecessary obstetrical intervention for too many, too little for others, and the high rate of preventable maternal deaths in the US
At the same time the pregnancies and labors of predominantly white middle and upper class mothers suffer from too many obstetrical interventions. However, it turns out that obstetrical departments are the cash cow for most general hospitals. According to a study published some years back, as the profit margin for hospital maternity department is 38 cents per dollar of revenue received, while the profit for the cardiac department was only 5 cents per dollar.
One of the reasons that the maternity departments are able to subsidize the less profitable aspects of hospitals is the high rate of Cesareans which pay about twice as much and take a lot less of the L&D resources.
Ref” ~ “Value-based care in obstetrics: comparison between vaginal birth and caesarean section” ~ BMJ April 2021
“The C-section group had significantly … higher rate of intensive unit care (ICU) admissions both for the mother and the newborn … and a higher average cost of hospitalization …”
<https://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/s12884-021-03798-2>
Lack of access to obstetrical services for all too many childbearing women of color, immigrants, the working poor and the uninsured
Unfortunately, many among the working poor, black and immigrant communities and the uninsured are not getting the obstetrical care they desperately need. This is actually very expensive for society, as it dramatically increases the number of premature births, which means tiny fragiles babies that need to spend months in the NICU and often have many downstream health and educational problems later in life.
But the big ugly mark on our obstetrical system is that for the entire 20th century and the first two decades of the 21st, America has had the ignoble distinction of having had one of the very highest maternal mortality rates in the entire developed world for over 120 years.
As of 2021, the United States has the ignoble distinction of having the very highest MMR of any wealth, first-world country. {Link >> ref: Commonwealth Club publication}
The Right and Wrong Use of Obstetrics
I continue trying to figure out how to eliminate the corrupted aspects of obstetrical practices – what I call the “wrong use of obstetrics” – while acknowledging its noble origins as a life-saving discipline. I am always supportive and grateful for this “right use” of obstetrics.
My goal, and that of many other childbirth “activists” , is an obstetrical profession that actually does what it claims to do – make childbirth safer for both healthy women while also keeping it as safe as possible for those with complications. For high-risk women, these obstetrical interventions and surgical deliveries are exactly what they need. But for healthy women and babies, that same interventive process works against them.
The Right Use of Obstetrics includes physiologic support for normal childbirth, also known as “midwifery” — the art of not interfering in the normal biology of childbirth
The ‘right use of obstetrics’ starts by acknowledging that childbirth in healthy women is made safer by supporting the normal biology of labor and birth. Therefore, the bedrock of obstetrics as a process of support for the normal biology of childbirth should be non-interventive care and a laboring woman who is not assigned to a hospital bed, but is both allowed and encouraged to be up and moving around while she is in labor.
This cannot be done when the mother-to-be is immobilized and tethered to her bed by the two cables from the electronic fetal monitor that are attached to her abdomen and lead back to CPU sitting next to her bed, and in the majority of labors, an Pitocin IV line in her arm running up to an IV pole next to her bed.
This normal support for normal labor and birth is neither a medical or a surgical process, but one that historically was known as “midwifery”. Egyptian hieroglyphics more than 5,000 years old and the biblical book of Exodus both record the origins midwifery as the very first form of ‘preventative health care’ as women who had given birth themselves helped other women to give birth. That assistance was (and continues to be) non-interventive physiological support and childbirth is generally safer when another experience adult is present to help .
It’s obviously true that the midwives of antiquity could do very little if either mother or baby developed a serious complication such as a hemorrhage or infection. During the many eons of human history before the discoveries that we now call “modern medical science”, there was nothing anybody — doctor or midwife — could do. This was true for all serious illness or injury. Having been both an L&D and ER nurse, and requiring fertility surgery before I was able to get pregnant, I am eternally grateful for my the three healthy children that i was able to give birth to, for modern medicine and in particularly for obstetrics and gynecology!
Unnecessary Fear of the “M” word by the obstetrical world
In the late 19th and early 2oth century, the word “midwifery” was used to describe the care provided by both midwives and doctors to women having a normal birth. As recently as the 1920s, American obstetricians were still publishing papers that described what they did as the practice of “midwifery”. (ref: “How Can We Best Solve the Midwifery Problem” by Dr.Charles Ziegler, Nov. 1921)
However, obstetrics was declared by American obstetricians to be a surgical speciality in the United States. Starting in 1910, American obstetricians defined childbirth to be a “patho-physiology”, that is, a form of biology that was frequently abnormal and undependable. In an attempt to make childbirth “safer”, obstetricians began to routinely conduct normal childbirth as a surgical procedure that included the use of general anesthesia, and a series surgical procedures.
Nonetheless, they defined the practice of midwifery by obstetricians to be dramatically different than what midwives did when they attended a birth. Believing as they did that episiotomy, forceps, manual extraction of the placenta was a necessary prerequisite to safe childbirth, the obstetrical profession insisted that that only ‘safe’ practice of midwifery was by someone who had graduated from medical school. This meant that midwives, who obviously were not MDs, had absolutely no business attending “cases of childbirth”.
The obstetrical profession, with the support of the AMA, embarked on a very successful legal and public relations campaign to abolish the practice of midwifery by midwives. As a result, they were able to get laws passed in a majority of states that made it a crime for anyone other than an MD to provide care during pregnancy and childbirth. The rate of midwife-attended birth fell from around 50% to just 13%, and those few remaining were mostly black midwives in the segregated South that provided care to women of color, poor whites, and inmigrantes.
The bottom-line to this historical account is the need to rehabilitate the word “midwifery” in the minds of obstetricians as well as the American public. “Midwifery” is first and foremost a verb, a process of providing childbirth services by trained professionals — obstetricians, family practice physicians and midwives. You don’t have to “be a midwife” in order to provide the supportive services described by the word “midwifery”. This is NOT a substandard form obstetrics, as its “right use” embraces the principle of physiological management, whether that is by an OB, an L&D nurse, a nurse-midwife employed by the hospital or independent midwives providing primary care in an out-of-hospital setting.
What makes “midwifery” in America different than it is in other countries is that in a majority of other places midwives and obstetricians have a complimentary role with one another. For the most part, they work together instead of eyeing one another as either “competitors” or the “enemy”.
It would be a great service to childbearing women and their midwives if the professional organization for obstetricians in the US — the American College of Obstetricians and Gynecologists (ACOG) — could make its peace with the positive role of “midwifery” care, whether provided by MDs or midwives — as the best way make normal childbirth in healthy women with normal pregnancies safer. Equally important, lowering the medical and surgical interventions rates would ultimately lower our scandalously high maternal mortality rate. We really are all on the same side — a national maternity care system that cared for mothers and babies, from which childbearing women emerge as healthy, or even healthier than before they had their baby.
Support for normal childbirth as the 21st century standard of care in America with in the context of the Right Use of Obstetrics
Support for normal childbirth is the only safe and sane standard for maternity care in the United States. This is a win-win solution that saves healthy women and their unborn babies from the iatrogenic complications that are the result of unwanted and unnecessary obstetrical interventions.
Equally important, this would allow the obstetrical profession to reclaimed its noble and heroic mission – preventing unnecessary pain and suffering, saving the lives of mothers and babies, preserving the reproductive health of childbearing women, and receiving the gratitude of the many families they helped and the well-earned respect by the general public.
And all this is very much less expensive than our current highly interventive system, with its 32% C-section rate and very high maternal mortality and morbidity rate.
Maternity Care as Judged by its Result
Ultimately, all maternity care is judged by its results — the number of mothers and babies who graduate from its ministration as healthy, or healthier, than when they started.
This form of care needs is determined by the health status of the childbearing woman and her unborn baby, in conjunction with the mother’s stated preferences, rather than by the occupational status of the care provider (physician, obstetrician, midwife). It calls for integrating physiological principles with the best advances in obstetrical medicine to create a single, evidence-based standard for all healthy women
The care that a laboring woman typically receives in hospital obstetrical departments is oxymoronic at best, as it’s based on the category of the care provider, rather than the health status of the childbearing woman. Healthy women, who don’t need and don’t benefit from obstetrically-managed labors and births, are being cared for by obstetricians who are trained in and accustomed to routinely using obstetrical interventions, and being charged a lot of money for interventions they didn’t need, didn’t want, and far too often, were harmed by.
The form of care recommended by W.H.O. for a healthy population integrates the principles of physiological management with the best advances in obstetrical medicine to create a single, evidence-based standard for all healthy women. This standard should apply to all categories of birth attendants and in all settings and include the use of standard obstetrical interventions to treat complications and when medicalized care is requested by the childbearing woman.
No healthy woman should ever have to choose between an obstetrician and a midwife or between hospital and home in order to received physiologically based, non-interventive childbirth services. No matter who provides their maternity care – OB, family practice physician, or professional midwife, women should be confident that they will receive appropriate, physiologically-based care for a normal labor and spontaneous birth, while continuing to have unfettered access to obstetrical services if or when they desire or require them.
We need to use our energies to transform our national maternity care policies and reconfigure the system at its most basic and practical level by promoting:
- Maximal results with minimal interventions
- Skillful use of physiological management
- Adroit use of medical interventions as necessary
- Fewest number of medical/surgical procedures
- Least expense
- Best outcome for mothers and babies
- Value to families – meeting their social, psychological and developmental needs as defined by the mother, father and other members of the family
Modern Maternity Care for Healthy Childbearing Women
The fundamental purpose of maternity care is to protect and preserve the health of already healthy women. Mastery in normal childbirth services means bringing about a good outcome without introducing any unnecessary harm or unproductive expense.
The ideal maternity care system seeks out the point of balance where the skillful use of physiological management, and adroit use of necessary medical interventions, provides the best outcome with the fewest number of medical and surgical procedures and least expense to the healthcare system.
For an essentially childbearing healthy population, the safest and most cost-effective form of maternity care is always the method that provides “maximal results with minimal interventions”. This is a beneficial ratio of interventions to outcomes for each childbearing woman.
Modern Maternity Care
 for Healthy Women
for Healthy Women
with Normal Pregnancies
by Faith Gibson, LM
I ~ The fundamental purpose of maternity care is to protect and preserve the health of already healthy women.
II ~ For an essentially healthy population, the safest and most cost-effective form of maternity care is always the method that provides “maximal results with minimal interventions”. This is a beneficial ratio of interventions to outcomes for each childbearing woman.
III ~ Mastery in normal childbirth services means bringing about a good outcome without introducing any unnecessary harm or unproductive expense.
IV ~ The ideal maternity care system seeks out the point of balance where the skillful use of physiological management and adroit use of necessary medical interventions provides the best outcome with the fewest number of medical and surgical procedures and least expense to the healthcare system.
V ~ Maternity care in a healthy population is ultimately judged by its results — the number of mothers and babies who graduate from its ministrations as healthy, or healthier, than when they started.
@@@@@@@@@@@@@@@@@@@@@@@@@@@
File name Part-1_xyz-t1_The “Jeckle and Hyde” nature of the obstetrical dilemma_Feb-21-2023 Art-&-science-Mfry_Nov-30-22_Not-used_pg-9-to-33_12-01-2022
@@@@@@@@@@@@@@@@@@@@@@@@@@@

