1D: The Dark Side of the Moon
-
 Serious and ongoing disagreement btw individual obstetricians on EFM data & whether an emergent C-section is needed
Serious and ongoing disagreement btw individual obstetricians on EFM data & whether an emergent C-section is needed -
How and why EFM is directly associated with increased rate of Cesareans
The other great big ‘elephant’ in the labor room when interpreting c-EFM data is the incredible lack of agreement between obstetricians over the data being streamed to fetal monitor screens and printed out on reams of graph paper.
All the professional insiders — OBs, L&D nurses, obstetrical department heads, hospital administrators and their attorneys and lobbying groups such as the American College of Obstetricians & Gynecologists ACOG — are each and everyone aware of the “slips twixt cup and lip” when it comes to the interpretations EFM data by different obstetricians.
Here is another excerpt from the “Female Patient” April 2011 quoted earlier that reports on studies of this issue that the public is never privy to:
“There is considerable inter- and intra-variability in the interpretation of EFM. Clinicians disagree with each other in their evaluation of FHR about 80% of the time.
Even when reviewing the same FHR pattern several months later, a clinician disagrees with his or her own initial interpretation about 20%of the time.1″
One study by Chauhan et al had 5 clinical obstetricians evaluate the FHR patterns of 100 parturients using the traditional intrapartum evaluation (reassuring vs. non-reassuring). Forty-six percent of these patients had an emergent cesarean delivery, and 2% had a fetal pH less than 7.0.
The study found that not only was their poor agreement among clinicians, but they could not even predict which labor patients had an emergent cesarean delivery or low fetal pH. [3]
Fetal metabolic acidosis and hypoxic-ischemic encephalopathy are also associated with significant increases in EFM abnormalities, but EFM predictive ability to identify these conditions is low.” [4]

Simply put, the scientific literature has never supported the routine use c-EFM and one of the reasons may well be that the obstetrical profession has never been able to agreed on how to interpret fetal monitor tracings.
If they did, the C-section rate would drop like a stone, but instead, neither the obstetrical profession and the American news media are talking about the big blue elephant that is smack in the middle of the room. And so, the operative motto for American obstetrics remains: “When in doubt, cut it out”.
This is confirmed by Cesarean operative reports that identify “non-reassuring” EFM tracing as the second most frequent reason for performing an intrapartum Cesarean on a first-time mother.
In 2003, 1.2 million Cesarean surgeries were performed in the US (27.5% cesarean rate) at a cost of $14.6 billion. The Cesarean rate for 2006 was over 31% and for the most recently available stats (2017) it’s a whopping 32.8 % (i.e. 33%) or one out of every three women who gave birth that year.
This is equivalent to the number of students that graduate from college every year.
However, C-section stats are wildly different, depending on what state the mother gives birth. For example, Cesarean statistics for first-time mothers in New Mexico, South Dakota and Iowa in 2017 were just 17%, but jumped to 31% of first-time moms in West Virginia. Obviously, the high Cesarean in the US is not the result of a universal failure of female reproductive biology, no can it be claimed that the pelvic capacity or uterine power of childbearing women in South Dakota was twice as good as women living in West VIrginia.
The use of Cesarean surgery as pre-emptive strike’ has not made the tiniest bit of difference in the incidence of CP and similar neurological conditions. And yet, the public and the press never seem to question how unlikely it is that normal childbirth in healthy women is somehow made safer and better by turning it into an expensive and risky operation.
Obstetricians talking out of both sides of their mouth by:
- Using scientific research on the ineffectiveness of c-EFM to defend themselves against lawsuits,
- Talking out of the other side of their mouth when they describe c-EFM as critical life-saving intervention and appropriate obstetrical standard of care to be used routinely on healthy women.
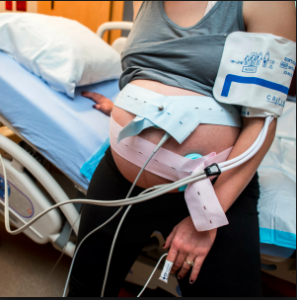 Even more oxymoronic is the obstetrical profession’s newly inverted relationship with c-EFM when it comes to malpractice cases claiming negligence for not using EFM every minute the mother was in the hospital. When OBs are on the other end of the legal stick, they happily acknowledge the large body of research (quoted in this and its companion posts) documenting the inability of EFM to prevent 92% of birth-related brain damage in newborns and use these facts to defend themselves in court.
Even more oxymoronic is the obstetrical profession’s newly inverted relationship with c-EFM when it comes to malpractice cases claiming negligence for not using EFM every minute the mother was in the hospital. When OBs are on the other end of the legal stick, they happily acknowledge the large body of research (quoted in this and its companion posts) documenting the inability of EFM to prevent 92% of birth-related brain damage in newborns and use these facts to defend themselves in court.
Since the publication of ACOG’s task force report in 2003, attorneys for obstetricians and hospitals who got sued because a baby developed CP trot out the studies that identify c-EFM as being unable to detect or prevent cerebral palsy, regardless of how much or little the mother was electronically monitored or how the EFM data was or wasn’t the interpretation by their OB or the L&D nurses.
Personally, I say ‘good for them’; obstetricians and hospitals shouldn’t be sued for bad outcomes they were NOT responsible for. But why is this recognition not used up-front, why not honestly tell low-risk women that the use of c-EFM makes no difference in outcomes for healthy women with normal pregnancies.
Why aren’t they giving their healthy patients copy of these studies or read their conclusions to them? For example, the April 2011 report Fetal Heart Rate Monitoring Update says:
“Despite the widespread use of EFM, there has been no decrease in cerebral palsy. … a meta-analysis of randomized control trials has shown that EFM has no effect in perinatal mortality or pediatric neurologic morbidity.2
However, EFM is associated with an increase in the rate of operative vaginal and cesarean deliveries.1”
Although intermittent fetal auscultation {IA} may be a theoretical option in low-risk patients, nursing staffing limitations makes this impractical … ”
 On the inability to agree on interpretation of EFM tracing:
On the inability to agree on interpretation of EFM tracing:
“Clinicians disagree with each other in their evaluation of FHR about 80% of the time. Even when reviewing the same FHR pattern several months later, a clinician disagrees with his or her own initial interpretation about 20% of the time.1
One study …. had 5 clinical obstetricians evaluate the FHR patterns of 100 parturients using the traditional intrapartum evaluation (reassuring vs. non-reassuring). Forty-six percent of these patients had an emergent cesarean delivery, and 2% had a fetal pH less than 7.0.
{BUT} The study found that not only was their poor agreement among clinicians, but they could not even predict which parturients had an emergent cesarean delivery or low fetal pH. [3]
AND this information on the increased risk of C-section and its many potentially-lethal complications:
Ob.Gyn.News in August 15, 2002, Dr. Hankins, professor and vice chair of Ob-Gyn at the University of Texas, Galveston, stated:
“Performing cesarean section for abnormal fetal heart rate pattern in an effort to prevent cerebral palsy is likely to cause as least as many bad outcomes as it prevents.
… A physician would have to perform 500 C-sections for multiple late decelerations or reduced beat-to-beat variability to prevent a single case of cerebral palsy.
But since Cesarean section carries a roughly 0.5% risk of future uterine rupture, those 500 C-sections would result on average in 2.5 uterine ruptures. This in turn would cause one case of neonatal death or cerebral palsy…. So I’ve prevented one case of cerebral palsy and I’ve caused one, concluded Dr. Hankins
Moreover, those 500 women who underwent C-section because of an abnormal fetal heart rate pattern face substantial morbidity related to their surgery, including a 5 to 10-fold increase in relative risk of infection, a 5-fold increase in [blood clots] as well as a 10- to 20-fold increase in future risk of placenta previa and accreta, he added.”
And this from Dr Peter Bernstein, MD, MPH; Associate Professor of Clinical Obstetrics & Gynecology and Women’s Health, Dept of Obstetrics and Gynecology, Albert Einstein College of Medicine; “Elective Cesarean Section: An Acceptable Alternative to Vaginal Delivery?” Medscape Ob/Gyn & Women’s Health; 9/16/02
“Although cesarean delivery has clearly become safer over the past 50 years with advances in antibiotics, anesthesia, and thromboprophylaxis, it is still not without risks. Woman undergoing cesarean delivery have greater blood loss and risk of damage to internal organs.
The mortality risk of undergoing an elective cesarean delivery with no emergency present has recently been reported almost 3 times the risk of vaginal delivery. [3]
Unfortunately, the well-documented evidence that c-EFM for healthy women makes absolutely no difference when it comes to the policies imposed by hospital obstetrical units. They continue to insist that low and moderate risk women must be hooked up to continuous fetal monitor for the entire length of their labors.”
Obstetrical Politics: same political strategies used for years by the tobacco and gun lobbies and “too big to fail” banks:
In the face of obvious and overwhelming evidence, the strategy is to “just say NO!”, dig in your heels, your the tables by aggressively attacking the opposition, and never, never, never admit defeat or give an inch!
If we, who are living in a democratic society let this ‘status quo’ prevail unchallenged in the face of a mountain of irrefutable scientific evidence of c-EFM’s ineffectiveness AND the fatal risk to childbearing women due to complications of Cesarean surgery, then we have to share the guilt with ACOG policymakers.
 In that case, it’s shame on us every time a healthy low-risk mother, who should have been monitored by the continuous presence of nurses or midwives using intermittent auscultation (IA), instead had a medically-unnecessary emergency CS due to the undependable information on an EFM tracing.
In that case, it’s shame on us every time a healthy low-risk mother, who should have been monitored by the continuous presence of nurses or midwives using intermittent auscultation (IA), instead had a medically-unnecessary emergency CS due to the undependable information on an EFM tracing.
And every time such a mother has intra-operative complications — hemorrhage, shock, drug reactions — requiring days or weeks in the ICU, and every time a post-Cesarean mother has to be treated for a post-op infection following her surgery and then loses her ability to breastfeed when she had to be re-admitted to the hospital with a drug-resistant infection that requires a week of IV antibiotics.
And every time a previous-Cesarean mother develops a placenta increta so extensive it requires a Cesarean-hysterectomy in a subsequent pregnancy, and every time previous-Cesarean mother finds herself to be one of the unlucky 7 to 10% of placenta percreta patients that, in spite of being care for in one of the best hospitals with the best doctors, blood banking and best of modern medical and technological equipment, dies from a massive and uncontrollable hemorrhage.
And every time a post-Cesarean mother dies 8 months later from a necrotic bowel caused by adhesions that develop due to her Cesarean surgery,
And every time a post-Cesarean woman finds that she is no longer able to get pregnant — secondary infertility — due thank to the post-op infection that scared her fallopian tubes.
And last, but certainly not least, every time a husband it told that his wife “didn’t make it” due to an intra-operative, post-operative, delayed or downstream complication of her most-often medically UNNECESSARY C-section, leaving him a widow and their children without a mother.
We all must own some part of the guilt of system that has institutionalized and systemized the abuse of their own power and economic advantage, a system that is characterized by a wanton disregard for the true wellbeing of healthy childbearing women and their families.
This is end of the original, five-part post republished as “Intro-Overview” and 1A, 1B, 1C, & 1D
Continue to next post in series Part 2A ~
The False Association btw routine use of c-EFM) to prevent pelvic floor damage in mothers
References
- ObGyn liability insurance: https://www.capson.com/medical-malpractice-insurance-by-specialty/
- C-section rate for first time mothers – 2017 https://www.statista.com/statistics/800589/us-hospital-c-section-rates-by-state/
Original link: http://collegeofmidwives.org/collegeofmidwives.org/Political_Action_2006/False_assoc_EFM-CS-prev-CP_08.htm