|
Originally published on the front page of my “NormalBirth.org” website
 I am reposting this essay from 2007 as an example of how the story never really changes — we still have an obstetrical system that systematically imposes harmful and unnecessary interventions and surgical procedures on healthy women with normal pregnancies. I am reposting this essay from 2007 as an example of how the story never really changes — we still have an obstetrical system that systematically imposes harmful and unnecessary interventions and surgical procedures on healthy women with normal pregnancies.This unproductively expensive, totally unrepentant and wrong-headed use of obstetrics is why maternal mortality in the US ranks in 128th place worldwide.
Mothers are safer having their babies in 127 other countries than in the United States. Shame on us!
Faith Gibson ~ December 31, 2007
The New York Times’ op-ed piece on “The high Cost of Healthcare” (11-26-
 07) was excellent. However, it failed to mention the most frequent, most expensive and most misunderstood healthcare issue in the US – the unnecessary medicalization of normal childbirth for 3 million healthy women every year. 07) was excellent. However, it failed to mention the most frequent, most expensive and most misunderstood healthcare issue in the US – the unnecessary medicalization of normal childbirth for 3 million healthy women every year. For the last hundred years, the US has had a policy of using interventionist obstetrics as the primary source of maternity care for healthy women. The core of this obstetrical system – normal birth as a surgical procedure — was developed in 1910 to prevent hospital epidemics of childbirth-related infections in a pre-antibiotics era.
Since one-fifth of our annual healthcare budget is now being spent on maternity care, no effort to reform our national healthcare system can afford to ignore our expensive habit of medicalizing normal childbirth.
This issue has nothing to do with the appropriate use of obstetrical intervention to treat the 30% of women who develop complications. It’s obvious that modern obstetrical medicine is indispensable to modern life. As a mother, I have personally benefited from these medical miracles; as a maternity care provider, I greatly respect the life-saving skills of the obstetrical profession. The question is the wisdom, safety, and economic impact of routinely using invasive obstetrical interventions on a healthy population.
Ninety percent of women who become pregnant every year in the US are healthy; 70 to 80% are still enjoying a normal pregnancy nine months later. While the ratio of ill health and pregnancy complications in 2007 is many times less than it was in the early 1900s, the number and frequency of obstetrical interventions has sky-rocketed all out of proportion over the last century.
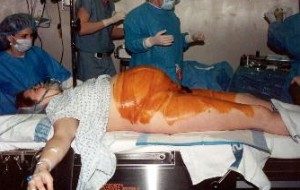 As American women have become progressively healthier, the operative delivery rate in the in the US has inexplicably risen with every decade. We seem to have lost sight of the basic purpose of maternity care, which is to preserve the health of already healthy women. Mastery in this field means bringing about a good outcome without introducing unnecessary harm or unproductive expense. As American women have become progressively healthier, the operative delivery rate in the in the US has inexplicably risen with every decade. We seem to have lost sight of the basic purpose of maternity care, which is to preserve the health of already healthy women. Mastery in this field means bringing about a good outcome without introducing unnecessary harm or unproductive expense. Out of the approximately four million babies born each year, nearly three-quarters of all obstetrical care goes to pregnant women who are healthy and have normal pregnancies. The medical intervention rate for this healthy population is 99%, with an average of seven significant medical procedures performed during labor on millions of healthy childbearing women every year. More than 70% of these new mothers will have one or more surgical procedures during birth – episiotomy, forceps, vacuum or Cesarean section. Over 2 million operative deliveries are performed each year in the US on this healthy population of women [a].
For the last two decade, Cesarean section has been the most commonly performed hospital procedure in the US [b]. In 2006, it was 31% of all births or 1.3 million Cesarean surgeries, equal to the total number of college students that graduate each year, with a price tag of approximately15 billion dollars.
One reason for the ever-increasing Cesarean rate is three decades of ever increasing obstetrical intervention in so-called “normal” vaginal births, a situation heavily influenced by the malpractice litigation issue. Since 1970, at least one major intervention has been added to the standard of care every couple of years. One by one, old and new medical procedures and restrictive protocols have been added to the labor woman’s experience.
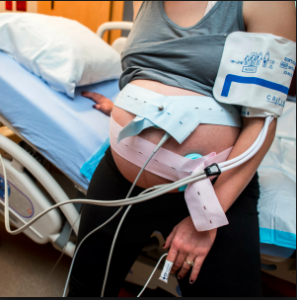
You can’t put a laboring woman in bed and hook her up to seven (or more) IV lines, electrical leads, tubes, automatic blood pressure cuff, pulse oximetry, catheters, and other equipment without profoundly disturbing the normally spontaneous biology of labor.
Each new intervention or drug introduces an independent risk, which is then multiplied by the aggregate of unpredictable interactions with one another. Every single invasive procedure increases the likelihood that a new mother will become infected with a drug-resistant bacteria such as MRSA (the Methicillin-Resistant Staphylococcus Aureus), a problem that already results in 90,000 nosocomial (hospital-acquired) infections every year.
Despite meticulous professional attention, ever higher intervention rates, and the huge amount of money spent on the American way of birth, we are still unable to match the better outcomes enjoyed by industrialized countries that use low-intervention maternity care systems. They achieve this laudable accomplishment by training physicians and professional midwives to manage childbirth physiologically, while reserving obstetrical interventions for women with complications and those who request medical interventions.
Cost-effective maternity care systems spend only a half to a third of what we do, while they enjoy a vastly superior outcome. At last count, the US was an embarrassing 32nd in perinatal mortality and ignoble 30th in maternal mortality.
During the 20th century there has been a steady improvement in maternal-infant outcomes around the world. Many assume this was the result of medicalizing normal childbirth in the richest countries, particularly the US. However, it turns out to be the result of an improved standard of living, general access to medical care and preventive use of people-intensive, low-tech maternity care.
This describes the prophylactic use of the eyes and ears and knowledge base of maternity care professionals who are able to screen for risk and refer for medical service as needed. This is the best ‘medicine’ for normalizing childbirth in a healthy population. As the medicalized model is currently configured in the US, it’s virtually impossible for any obstetrician or nurse midwife to provide physiologically-based care or for any mother have a truly physiological birth.
If we are to successfully compete in the global economy of the 21st century, we must develop a cost-effective maternity care system that relies on physiological practices for healthy women.
Unfortunately obstetrics in the US has turned its back on physiological childbirth for a hundred years. When combined with the unwarranted use of interventionist obstetrics, this disturbs the biological functions that make a normal childbirth possible. Millions of pregnant women are spending the many hours of their labor lying in bed while an extensive array of counterproductive and medically-unnecessary procedures are done to them.
The word for this is iatrogenesis. The obstetrical response to the increased morbidity that accompanies excessive intervention in vaginal birth is to propose the ultimate iatrogenic intervention – electively performed Cesarean surgery. There is a move within the obstetrical profession to promote electively scheduled Cesarean for healthy women as the preferred standard of care for the 21st century.
Replacing normal, low-risk biology with scheduled abdominal surgery is being promoted as better, safer and more economical, a two-for-one special that is suppose to be buying us better babies while saving the mother’s pelvic organs from the horrors of normal birth. It’s also being described as a gender rights issue and part of a woman’s “right to choose”. Renamed as the ‘maternal-choice’ Cesarean, medically unnecessary C-section is identified as the ultimate expression of control by women over their reproductive biology. Unfortunately, claims of improved safety or lowered cost do not square with the facts.
What we are not being told is that the scientific literature identifies many of the complications of Cesarean to be the same complications that Cesarean surgery was suppose to save us from. One recent study from France identified a 3½ times greater maternal mortality rate in electively scheduled Cesareans in healthy women with no history of health problems or complications during pregnancy. Another study on the elective or non-medical use of Cesarean surgery documented an increased mortality and morbidity for newborns.
The Medical Leadership Council (an association of more than 2,000 US hospitals), in its 1996 report on cesarean deliveries, concluded that the US cesarean rate was:
That’s pretty grim — a disjointed, economically-strapped and liability-burdened obstetrical system unable to help itself. I guess it’s up to consumers and (one hopes) investigative journalists to take on the problem. If the US is to successfully compete in the global economy of the 21st century, we will have to develop a cost-effective maternity care system that relies on physiological practices and is suitably “green”, that is, has a much smaller carbon footprint than our current system.
Obviously, we can’t eliminate the excessive use of Cesareans without providing an effective alternative — a plan that safely reduces the inappropriate reliance on technology, medical intervention and surgical delivery while meeting the physical, emotional and psycho-social needs of childbearing women. To bring about the necessary changes, we must initiate a robust public dialogue and reassess the unproductive methods that have captivated everyone’s imagination for the last hundred years.
Science-based Maternity Care for 21st Century
A consensus of the scientific literature identifies the physiological management of normal birth as the safest and most economical type of maternity care for healthy women. It’s the one used by countries with the best maternal-infant outcomes. Stedman’s Medical Dictionary defines physiological as: “…in accord with or characteristic of the normal functioning of a living organism”. When providing care to a healthy childbearing population, physiological care should be the foremost standard used by all birth attendants and in all birth settings.
Physiological care is a not passive or neglectful, it’s not just abstaining from the unnecessary use of medical interventions. It’s an active process for preserving maternal-fetal wellbeing that requires a technical body of knowledge and specific skills for addressing the physical, biological, and emotional needs that women face during labor. This model is always articulated with the healthcare system and includes the appropriate use of obstetrical interventions for complications or at the mother’s request.
Physiological management during labor and birth is associated with the lowest rate of maternal and perinatal mortality. It is protective of the mother’s pelvic floor and has the fewest number of medical interventions, the lowest rate of anesthetic use, obstetrical complications, episiotomy, and operative deliveries.
For women who choose physiologically managed care, the C-section rate ranges from 4 to 10 percent, which is three to seven times less than medicalized childbirth [British Medical Journal June 2005]. Millions of health care dollars can be saved every year on the direct cost of maternity care and a reduction in post-operative, delayed and downstream complications associated with Cesarean surgery. [ChildbirthConnection.org].
This is a hugely important savings to employers who pay for employee health insurance, for taxpayers who underwrite government-financed programs for the indigent and for the uninsured who must pay out of pocket.
A non-interventive approach to normal childbirth is careful not to disturb the natural process and to provide for appropriate physical and psychological privacy for the laboring woman. Its principles include patience with nature and continuity of care as provided by the primary caregiver throughout active labor. It acknowledges the mother’s right to control her environment and to direct her own activities, positions & postures during labor and birth. This may require changing institutional policies that interfere with the physiological process.
To help achieve these goals, evidence-based maternity care employs one-on-one social and emotional support and an absence of arbitrary time limits. Women are encouraged to move around during labor, to walk, change positions, be in the shower, etc. Being upright and mobile during contractions also diminishes the mother’s perception of pain, perhaps by stimulating endorphins. It takes into account the positive influence of gravity on the stimulation of labor. Right use of gravity helps dilate the cervix and assists the baby to descend down through the bony pelvis.
Physiologically-based maternity care for normal childbirth serves the needs of healthy families far better than our expensive and inflexible high-tech model, which is two to ten times more expensive than it should be. For example, a medically managed but otherwise totally normal vaginal birth in the San Francisco Bay area is about $32,000. In addition to the large initial cost, many common obstetrical interventions result in costly downstream complications, such as damage to the mother’s pelvic floor following episiotomy or instrumental delivery. Having had a Cesarean means a future risk of placental abnormalities, stillbirth, and emergency hysterectomy in a subsequent pregnancy.
Physiological management is misunderstood by the American medical profession, who tend to think of it as incompetent, negligent or substandard care and a horrible waste of their extensive and expensive medical education. We have a dysfunctional system because the default setting for childbirth in the US for the last hundred years has been obstetrical intervention. As a result, obstetricians see a disproportion number of complications and readily assume that the biology of birth is itself defective.
The assumption that childbirth is pathological creates a negative feed back loop that appears to justify an ever-increase level of medicalization. The obstetrical profession rarely acknowledges any causal relation between increasing rates of intervention and a rising levels of problems. Unfortunately, the 20th century legal standard for obstetrical care locks every obstetrical care provider into the same system and forces them to use the same invasive protocols, even when they personally know that physiological management is more appropriate to the situation.
Our 1910 system of medicalized maternity care has never been reexamined by modern scientific standards, or asked to account for its economic impact. To date, the most important untold story of the 20th century is how and why normal childbirth in a healthy population became the property of a surgical specialty and what the current costs and consequences of that are.
Judging a System by its Results
Ultimately, a maternity care system is judged by its results — the number of mothers and babies who graduate from its ministration as healthy, or healthier, than when they started. Medicalizing healthy women makes normal childbirth unnecessarily and artificially dangerous and is unproductively expensive. But unlike many of the problems facing us today that have so far defied our best efforts– cancer, terrorism, affordable healthcare for aging baby-boomers, etc— we know how to make a maternity care system for healthy women be safe and cost-effective. As a national maternity care policy, physiological principles should be integrated with the best advances in obstetrical medicine to create a single, evidence-based standard for all healthy women.
The question is simply this: How much longer will we be content to use an expensive, pathologically-based 19th century system for our healthy 21st century population?
Reference numbers refer to information on the Addendum {PDF version}.Topics either include the citation directly or a numbered bibliography
https://normalbirth.org/normalbirth.org/NYTimes_guest_opinion_Dec07.htm
|
||
The Politics of Normal Childbirth ~ Helping to End the Hundred Years War btw Midwifery & Medicine
