Coalition for Improving Maternity Services (CIMS) Fact Sheet February 2010 ~ Permission granted to freely reproduce with attribution.
1500 Sunday Dr, Suite 102, Raleigh, NC 27607 | Tel: 919-863-9482 | www.motherfriendly.org
Coalition for Improving Maternity Services (CIMS) Fact Sheet February 2010
Link to printable informational and “Informed Consent” documents
that can be copied, personalized and printed out.
Editor’s Note:

Despite the passage of 13 years since this list was complied, the many serious risks of Cesarean surgery unfortunately are exactly the same in 2023 as they were in 2010, which is to say, every bit as deadly.
That means is the risks listed below — immediate intra-operative, hosptial-acquired drug-resistant infections, other post-op complications, delayed, and downstream — are all the same and can be cites as such.
In fact, the maternal mortality rate in the US is the very highest in the developed world, a statistics that for the most part reflects the high level of routine intervention in the US, most especially routine induction before the due date and the continuing high rate of both elective and intrapartum.
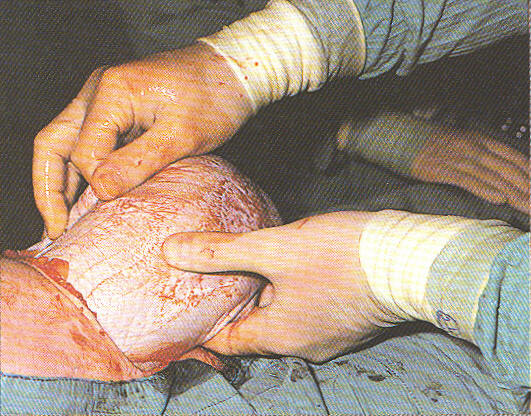
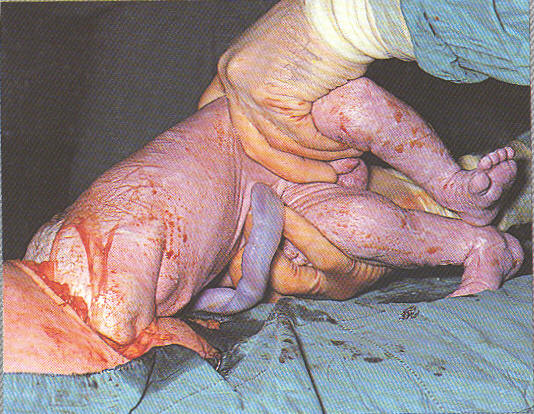
Risks of Cesarean Surgery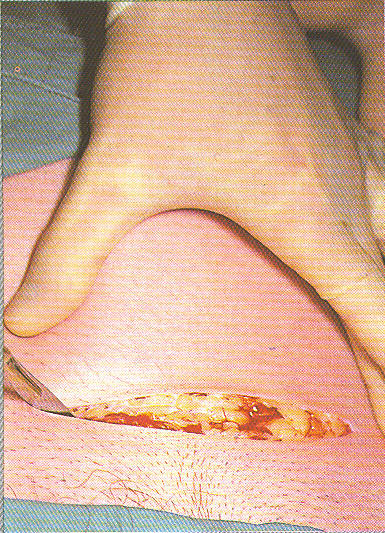
Cesarean section is the most common major surgical procedure performed in the United States. The Coalition for Improving Maternity Services (CIMS) is concerned about the dramatic increase and ongoing overuse of cesarean section.
The surgical procedure poses short- and long-term health risks to mothers and infants, and a scarred uterus poses risks to all future pregnancies and deliveries.
For these reasons, CIMS recommends that cesarean surgery be reserved for situations when potential benefits clearly outweigh potential harms.
The cesarean rate can safely be less than 15 percent {ref: 84} and 11 percent or less in low-risk women giving birth for the first time, {28} yet, in 2007 the U.S. cesarean rate was 32 percent.30 When cesarean surgery rates rise above 15 percent health outcomes for mothers and babies worsen,5 and increasing numbers of scheduled cesareans are contributing to the rising number of late- preterm births. {2,6}
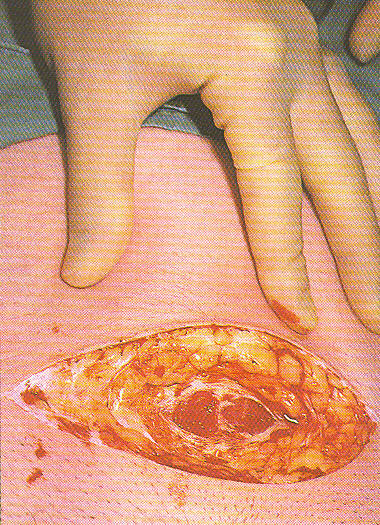 Cesarean rates have been rising for all women in the United States regardless of medical condition, age, race, or gestational age,52 and while the number of first cesareans performed without medical indication is increasing, no evidence supports the beliefs that these elective cesareans represent maternal request cesareans or that the rise in elective first cesareans has contributed significantly to the overall increase in cesarean rates. {52}
Cesarean rates have been rising for all women in the United States regardless of medical condition, age, race, or gestational age,52 and while the number of first cesareans performed without medical indication is increasing, no evidence supports the beliefs that these elective cesareans represent maternal request cesareans or that the rise in elective first cesareans has contributed significantly to the overall increase in cesarean rates. {52}
Elective first cesarean at physician request may, however, play a significant role, {39} and the rise in elective repeat surgeries, which has climbed by more than 40 percent in the last ten years, certainly does. {64} Although 70 percent of women or more who plan a vaginal birth after cesarean (VBAC) can birth vaginally and avoid the complications of repeat cesarean surgeries, {28} almost all women today have a repeat operation because most doctors and many hospitals refuse to allow VBAC. {20, 35, 54}
A cesarean can be a life-saving operation, and some babies would not be born vaginally under any circumstances; however, it is still major surgery. Women have a legal right to know the risks associated with their treatment and the right to accept or refuse it. {14} CIMS encourages childbearing women to take advantage of their rights and to find out more about the risks of cesarean section so they can make informed decisions about how they want to give birth.
What are the potential harms of cesarean surgery compared with vaginal birth?
Health outcomes after a cesarean may be worse because medical problems may lead to surgery. This fact sheet, however, is based on research that determined excess harms arising from the surgery itself. In other words, women with a healthy pregnancy who have a cesarean rather than a vaginal birth are at increased risk for the following complications as are their babies:
Potential Harms to the Mother
Compared with vaginal birth, women who have a cesarean are more likely to experience:
- Accidental surgical cuts to internal organs. {53,60,72}
- Major infection. {43,48}
- Emergency hysterectomy (because of uncontrollable bleeding). {38,48,83}
- Complications from anesthesia. {28}
- Deep venous clots that can travel to the lungs (pulmonary embolism) and brain (stroke). {28,48}
- Admission to intensive care. {58}
The Risks of Cesarean Section [editor note-2-self — insert { & } b4 & after ref below this point]
Page 2
- Readmission to the hospital for complications related to the surgery.18,28
- Pain that may last six months or longer after the delivery.19 More women report problems with pain from the cesarean incision than report pain in the genital area after vaginal birth.19
- Adhesions, thick internal scar tissue that may cause future chronic pain, in rare cases a twisted bowel, and can complicate future abdominal or pelvic surgeries.19
- Endometriosis (cells from the uterine lining that grow outside of the womb) causing pain, bleeding, or both severe enough to require major surgery to remove the abnormal cells.27
- Appendicitis, stroke, or gallstones in the ensuing year.18,46,47,50 Gall bladder problems and stroke may be because high-weight women and women with high blood pressure are more likely to have cesareans.
Negative psychological consequences with unplanned cesarean.
These include:
- Poor birth experience, overall impaired mental health, and/or self-esteem {12}.
- Feelings of being overwhelmed, frightened, or helpless during the birth.20
- A sense of loss, grief, personal failure , acute trauma symptoms, post-traumatic stress, and clinical depression. {37}
- Death {12,22}
Potential Harms to the Baby
 Compared with vaginal birth, babies born by cesarean section are more likely to experience:
Compared with vaginal birth, babies born by cesarean section are more likely to experience:
- Accidental surgical cuts, sometimes severe enough to require suturing.1,28
- Being born late-preterm (34 to 36 weeks of pregnancy) as a result of scheduled surgery.6
- Complications from prematurity, including difficulties with respiration, digestion, liver function, jaundice, dehydration, infection, feeding, and regulating blood sugar levels and body temperature.25,26 Late-preterm babies also have more immature brains,63 and they are more likely to have learning and behavior problems at school age.25,26
- Respiratory complications, sometimes severe enough to require admission to a special care nursery, even in infants born at early term (37 to 39 weeks of pregnancy).28 Scheduling surgery after 39 completed weeks minimizes, but does not eliminate, the risk.31,32
- Readmission to the hospital.25
- Childhood development of asthma,3,78 sensitivity to allergens,61 or Type 1 diabetes.11
- Death in the first 28 days after birth. {51
Potential Harms to Maternal Attachment and Breastfeeding
Failure to breastfeed has adverse health consequences for mothers and babies. Breastfeeding helps protect mothers against postpartum depression, Type 2 diabetes, high blood pressure, heart disease, ovarian and pre-menopausal breast cancer, and osteoporosis later in life.36,71 Breastfeeding helps protect babies against ear infections, stomach infections, severe respiratory infections, allergies, asthma, obesity, Type 1 and Type 2 diabetes, childhood leukemia, sudden infant death syndrome (SIDS), and necrotizing enterocolitis (a severe, life-threatening intestinal infection).15,36
- Women who have unplanned cesareans are more likely to have difficulties forming an attachment to their babies.23
- Women who have cesareans are less likely to have their infants with them skin-to-skin (cradled naked against their bare chest) after the delivery.20 Babies who have skin-to-skin contact interact more with their mothers, stay warmer, and cry less. When skin-to-skin, babies are more likely to be breastfed early and well, and to be breastfed for longer. They may also be more likely to have a good early relationship with their mothers, but the evidence for this is not as strong.16,57
- Women are less likely to breastfeed.21,44
The Risks of Cesarean Section
Page 3
Potential Harms to Future Pregnancies
With prior cesarean, women and their babies are more likely to experience serious complications during subsequent pregnancy and birth regardless of whether they plan repeat cesarean or vaginal birth. The likelihood of serious complications increases with each additional operation.28
Compared with prior vaginal birth, prior cesarean puts women at increased risk of:
- Uterine scar rupture. Planning repeat cesarean reduces the excess risk, but it is not completely protective.8,49,55,75
- Infertility, either voluntary (doesn’t want more children) or involuntary (can’t have more children).7,12,56,70,74,79,80
- Cesarean scar ectopic pregnancy (implantation within the cesarean scar), a condition that is life- threatening to the mother and always fatal for the embryo.67
- Placenta previa (placenta covers the cervix, the opening to the womb), placental abruption (placenta detaches partially or completely before the birth), and placenta accreta, (placenta grows into the uterine muscle and sometimes through the uterus, invading other organs), all of which increase the risk for severe hemorrhage and are potentially life-threatening complications for mother and baby.17,28,85
- Emergency hysterectomy.42,53
- Preterm birth and low birth weight.6,40,65,73,76
- A baby with congenital malformation or central nervous system injury12 due to a poorly functioning placenta.
- Stillbirth.28,29,40,65,76
Cesarean Surgery and Pelvic Floor Dysfunction
 Cesarean proponents claim that cesarean surgery will prevent pelvic floor dysfunction, but it offers little or no protection once healing is complete and no protection in later life.12 Moreover, risk-free measures such as engaging in exercises to strengthen the pelvic floor or losing weight can often improve or relieve stress urinary incontinence (loss of urine with pressure on the pelvic floor such as with exercise, laughing, sneezing, or coughing).9,12
Cesarean proponents claim that cesarean surgery will prevent pelvic floor dysfunction, but it offers little or no protection once healing is complete and no protection in later life.12 Moreover, risk-free measures such as engaging in exercises to strengthen the pelvic floor or losing weight can often improve or relieve stress urinary incontinence (loss of urine with pressure on the pelvic floor such as with exercise, laughing, sneezing, or coughing).9,12
Cesarean surgery does not protect against sexual problems,4,33,41 gas or stool incontinence,10,59 or urge urinary incontinence (loss of urine after sudden need to void).10,13,24,62,82
Cesarean surgery does not protect against severe stress urinary incontinence.62,82 As many as one more woman in six having vaginal birth may experience stress urinary incontinence of some degree, mostly minor, at six months or more after birth.10,13,24,62,82
Perhaps one more woman in twenty having vaginal birth will experience symptomatic pelvic floor prolapse (muscle weakness causes the internal organs to sag downwards).45,66,77,81 With three or more vaginal births, this number may be as high as one more woman in ten.66
 However, many other factors, including smoking, hysterectomy, hormone replacement therapy, constipation, irritable bowel syndrome, and urinary tract infections are also associated with pelvic floor prolapse.Cesarean Section, Care Providers and Place of BirthTo reduce the risk of cesarean surgery, CIMS encourages women to seek providers and hospitals with low cesarean rates (15% or less) and those that support VBAC. Women can access this data from their state health departments. They can also access hospital-specific cesarean rates and rates for other birth interventions for several states at www.thebirthsurvey.com and a listing of hospitals that do or do not support VBAC from the International Cesarean Network at http://ican-online.org/vac-ban-info.
However, many other factors, including smoking, hysterectomy, hormone replacement therapy, constipation, irritable bowel syndrome, and urinary tract infections are also associated with pelvic floor prolapse.Cesarean Section, Care Providers and Place of BirthTo reduce the risk of cesarean surgery, CIMS encourages women to seek providers and hospitals with low cesarean rates (15% or less) and those that support VBAC. Women can access this data from their state health departments. They can also access hospital-specific cesarean rates and rates for other birth interventions for several states at www.thebirthsurvey.com and a listing of hospitals that do or do not support VBAC from the International Cesarean Network at http://ican-online.org/vac-ban-info.
© 2010 Coalition for Improving Maternity Services. Coalition for Improving Maternity Services (CIMS) Fact Sheet February 2010Permission granted to freely reproduce with attribution.
The Risks of Cesarean Section Page 4
 Healthy women at low risk for complications should also know that choosing midwifery care or giving birth in a birth center or at home can lower their risk for cesarean section.68,69 Having a doula reduces the likelihood of a cesarean as well.34
Healthy women at low risk for complications should also know that choosing midwifery care or giving birth in a birth center or at home can lower their risk for cesarean section.68,69 Having a doula reduces the likelihood of a cesarean as well.34
This fact sheet was co-authored by Henci Goer, BA and Nicette Jukelevics, MA, ICCE.
© 2010 Coalition for Improving Maternity Services. Permission granted to freely reproduce with attribution.
This fact sheet is endorsed by the following organizations (as of Feb. 2010).
Academy of Certified Birth Educators
Birth Matters Virginia, BirthNet of Albany NY
BirthNetwork National
Birth Network of Santa Cruz
Birth Works International
Childbirth Connection
Choices in Childbirth
Citizens for Midwifery
DONA International
International Childbirth Education Association,
Lamaze International
The Lawton and Rhea Chiles Center for Healthy Mothers and Babies
Midwives Alliance of North America
National Association of Certified Professional Midwives
North American Registry of Midwives
Perinatal Education Associates
Reading Birth and Women’s Center
Tatia Oden-French Memorial Foundation
Labor: The Organization of Labor Assistants for Birth Options and Resources
 Editor’s Note: the original list of information and fully “Informed Consent“ for Cesarean surgery is included below and also can be accessed as a stand-along document from the link at the very top of this post.
Editor’s Note: the original list of information and fully “Informed Consent“ for Cesarean surgery is included below and also can be accessed as a stand-along document from the link at the very top of this post.
Click here to access a printable copy of a check list with both information and “informed consent” document for Cesarean and VBAC (vaginal birth after Cesarean)
A Checklist for Expectant Mothers to Read During Pregnancy
Birth is a normal, natural, process and the vast majority of women can have safe, normal, vaginal births. There are health conditions where a cesarean birth is necessary for the well being of the mother or her baby.
However, more and more mothers these days are giving birth by cesarean section for non-medical reasons. A cesarean poses risks as well as benefits for mother and baby, and should not be undertaken lightly.
This educational material is provided by the Coalition for Improving Maternity Services (CIMS) to help all expectant parents become better informed about the risks of cesarean section.
To give the expectant mother time to reflect on this information and consider the impact of cesarean surgery on her health and the health of her baby, care providers are encouraged to introduce and discuss this evidence- based information throughout pregnancy and no later than at 32-34 weeks. The expectant mother is encouraged to take the form home, read and initial the statements, discuss the information with her partner, and raise any questions or concerns she may have with her care provider.
The form may then be placed in her chart.
Link to stand-alone document that has printable informational and “Informed Consent” to be copied, personalized and printed out.
 For Reading
For Reading
Information on the risk of Cesarean Surgery
Compiled & published by the Coalition for Improving Maternity Services
(CIMS) 2010
Expectant Mother’s Name: _________________________________________________
Care Provider’s Name: ____________________________________________________
A cesarean section is an operation by which a baby is born by making a cut in the mother’s lower abdominal wall (abdominal incision) and a cut in her uterus (uterine incision). I understand that a cesarean operation may be more dangerous than a vaginal birth for my baby and me.
POSSIBLE PROBLEMS FOR ME WITH A CESAREAN
AS COMPARED TO A VAGINAL BIRTH:
1._____ I am more likely to have more blood loss and a longer recovery time.
2._____ I am more likely to have accidental surgical cuts to my bladder, bowel, or gastrointestinal tract.
3._____ I am more likely to have a serious infection in my incision, uterus, or bladder.
4._____ I am more likely to have thick scarring (adhesions) inside my abdomen that may cause chronic pain years after my cesarean. This scarring can make any future abdominal operation I may need more difficult.
5._____ I may have uncontrolled bleeding and need an emergency hysterectomy (removal of the uterus) if the bleeding cannot be stopped.
6._____ I am more likely to have complications from anesthesia.
7._____ I am more likely to develop serious and life-threatening blood clots that can travel to my lungs (pulmonary embolism) or my brain (stroke).
8._____ I am more likely to be admitted to intensive care.
9._____ I am more likely to need to return to the hospital for complications from the cesarean operation.
10._____ I am more likely to feel pain and/or numbness at the site of the operation for several months after my surgery.
11._____ I am less likely to breastfeed successfully. I may lose out on the health benefits of breastfeeding for myself, including: weight loss, reduced risks of cancers, heart disease, diabetes, and osteoporosis.
12._____ I am less likely to have a satisfactory birth experience. I am more likely to have emotional problems such as postpartum depression and post-traumatic stress. Many women experience a profound sense of happiness after a normal birth that flows naturally into bonding with the baby and breastfeeding.
13._____ I am more likely to die.
© 2010 Coalition for Improving Maternity Services. Permission granted to freely reproduce with attribution. 1500 Sunday Dr Ste 102, Raleigh, NC 27607 | Tel: 919-863-9482 | www.motherfriendly.org
Coalition for Improving Maternity Services (CIMS) Fact Sheet February 2010
About The Risks of Cesarean Section: A Checklist For Expectant Mothers To Read During Pregnancy
POSSIBLE PROBLEMS WITH A CESAREAN FOR ME
WITH A FUTURE PREGNANCY AS COMPARED TO A VAGINAL BIRTH:
14._____ I am more likely to have trouble becoming pregnant again.
15._____ I am more likely to have complications in a future pregnancy due to the scar in my uterus. If the new placenta attaches over my previous scar, it is more likely to cause serious problems, including: serious bleeding, placenta coming in front of the baby (placenta previa), placenta growing into or even through the wall of the womb (placenta accreta), miscarriage, or pre-term birth.
16._____ I am more likely to have a baby with a congenital malformation, central nervous system injury, or low birth weight due to problems with the placenta.
17._____ I am more likely to have a stillbirth.
18._____ I am more likely to require major surgery to remove cells from the lining of my uterus that may grow outside my womb (endometriosis).
19._____ Since it is difficult to find a physician or hospital supportive of a vaginal birth after a cesarean (VBAC), I am more likely to have a repeat cesarean for the birth of all my future children, although a vaginal birth after a cesarean birth is usually safe. Each additional operation I have increases the odds for complications.
20._____ Research shows that having a cesarean will not protect me from urine, gas, or stool incontinence in the future, or from future sexual problems.
21._____ I may not be able to get healthcare coverage since some insurance providers consider a cesarean to be a pre-existing condition.
POSSIBLE PROBLEMS FOR MY BABY:
1._____ My baby is more likely to be born prematurely if the cesarean surgery is performed anytime before labor begins. A premature baby is more likely to experience the following:
- admission to the intensive care nursery
- trouble breastfeeding, digesting food, and regulating body temperature
- developing jaundice
- brain development problems and difficulties in learning in school
2._____ My baby is more likely to face complications from anesthesia and postpartum pain medication.
3._____ My baby is more likely to be accidentally cut during surgery.
4._____ My baby is more likely to have breathing difficulties since labor contractions clear the lungs.
5._____ If I agree to a scheduled cesarean, it is normally best to wait for labor to begin before performing the operation.
6._____ My baby is more likely to have difficulty breastfeeding. My baby is less likely to benefit from skin-to- skin contact with me and is less likely to get the health benefits from breastfeeding including: reduced risk for asthma, allergies, respiratory infections, Type 1 diabetes, childhood leukemia, and SIDS (sudden infant death syndrome). If I do have a cesarean, I can request special care to help me and my baby breastfeed successfully before I am discharged from the hospital.I have read and discussed this information with my care provider.
Expectant Mother’s Signature: _______________________________ Date: ________________
Care Provider’s Signature: __________________________________ Date: ________________
This information is provided for expectant mothers and their care providers by the Coalition for Improving Maternity Services (CIMS). CIMS strongly recommends that cesarean surgery be reserved for situations when potential health benefits clearly outweigh the risks. Please see the The Risks of Cesarean Section, a CIMS Fact Sheet for the references that support this form, available as a free download from www.motherfriendly.org.
© 2010 Coalition for Improving Maternity Services. Permission granted to freely reproduce with attribution.
References:
- Alexander, J. M., Leveno, K. J., Hauth, J., Landon, M. B., Thom, E., Spong, C. Y., et al. (2006). Fetal injury associated with cesarean delivery. Obstet Gynecol, 108(4), 885-890.
- Analysis shows possible link between rise in c-sections and increase in late preterm birth. (12/16/08). Retrieved 11/12/09, from http://www.marchofdimes.com/aboutus/22684_48910.asp
- Bager, P., Wohlfahrt, J., & Westergaard, T. (2008). Caesarean delivery and risk of atopy and allergic disease: Meta-analyses. Clin Exp Allergy, 38(4), 634-642.
- Barrett, G., Peacock, J., Victor, C. R., & Manyonda, I. (2005). Cesarean section and postnatal sexual health. Birth, 32(4), 306-311.
- Betran, A. P., Merialdi, M., Lauer, J. A., Bing-Shun, W., Thomas, J., Van Look, P., et al. (2007). Rates of caesarean section:Analysis of global, regional and national estimates. Paediatr Perinat Epidemiol, 21(2), 98-113.
- Bettegowda, V. R., Dias, T., Davidoff, M. J., Damus, K., Callaghan, W. M., & Petrini, J. R. (2008). The relationship betweencesarean delivery and gestational age among us singleton births. Clin Perinatol, 35(2), 309-323, v-vi.
- Bhattacharya, S., Porter, M., Harrild, K., Naji, A., Mollison, J., van Teijlingen, E., et al. (2006). Absence of conception aftercaesarean section: Voluntary or involuntary? BJOG, 113(3), 268-275.
- Blanchette, H., Blanchette, M., McCabe, J., & Vincent, S. (2001). Is vaginal birth after cesarean safe? Experience at a communityhospital. Am J Obstet Gynecol, 184(7), 1478-1484; discussion 1484-1477.
- Bo, K. (2009). Does pelvic floor muscle training prevent and treat urinary and fecal incontinence in pregnancy? Nat Clin Pract Urol,6(3), 122-123.
- Borello-France, D., Burgio, K. L., Richter, H. E., Zyczynski, H., Fitzgerald, M. P., Whitehead, W., et al. (2006). Fecal and urinaryincontinence in primiparous women. Obstet Gynecol, 108(4), 863-872.
- Cardwell, C. R., Stene, L. C., Joner, G., Cinek, O., Svensson, J., Goldacre, M. J., et al. (2008). Caesarean section is associated withan increased risk of childhood-onset type 1 diabetes mellitus: A meta-analysis of observational studies. Diabetologia, 51(5), 726-735.
- Childbirth Connection. (2004). Harms of cesarean versus vaginal birth: A systematic review. Retrieved 4/17/2004, fromhttp://childbirthconnection.org/article.asp?ck=10271
- Chin, H. Y., Chen, M. C., Liu, Y. H., & Wang, K. H. (2006). Postpartum urinary incontinence: A comparison of vaginal delivery,elective, and emergent cesarean section. Int Urogynecol J Pelvic Floor Dysfunct.
- Coalition for Improving Maternity Services. (2007). Step 2: Provides accurate, descriptive, statistical information about birth carepractices. J Perinat Educ, 16(1), 20S-22S.
- Coalition for Improving Maternity Services. (2009). Breastfeeding is priceless: There is no substitute for human milk, a cims fact sheet. Retrieved 11/12/09, from http://www.motherfriendly.org/pdf/BreastfeedingisPricelessMarch2009.pdf
- Crenshaw, J. (2009). Healthy birth practices from lamaze international. #6: Keep mother and baby together-it’s best for mother,baby, and breastfeeding. Retrieved 2009, from http://www.lamaze.org/Portals/0/carepractices/CarePractice6.pdf
- Daltveit, A. K., Tollanes, M. C., Pihlstrom, H., & Irgens, L. M. (2008). Cesarean delivery and subsequent pregnancies. ObstetGynecol, 111(6), 1327-1334.
- Declercq, E., Barger, M., Cabral, H. J., Evans, S. R., Kotelchuck, M., Simon, C., et al. (2007). Maternal outcomes associated withplanned primary cesarean births compared with planned vaginal births. Obstet Gynecol, 109(3), 669-677.
- Declercq, E., Cunningham, D. K., Johnson, C., & Sakala, C. (2008). Mothers’ reports of postpartum pain associated with vaginal andcesarean deliveries: Results of a national survey. Birth, 35(1), 16-24.
- Declercq, E., Sakala, C., Corry, M. P., & Applebaum, S. (2006). Listening to mothers ii: Report of the second national u.S. Survey ofwomen’s childbearing experiences. New York: Childbirth Connection.
- Declercq, E., Sakala, C., Corry, M. P., & Applebaum, S. (2008). New mothers speak out:. National survey results highlight women’spostpartum experiences. . New York: Childbirth Connection.
© 2010 Coalition for Improving Maternity Services. Permission granted to freely reproduce with attribution.
Coalition for Improving Maternity Services (CIMS) Fact Sheet February 2010
The Risks of Cesarean Section Page 5
- Deneux-Tharaux, C., Carmona, E., Bouvier-Colle, M. H., & Breart, G. (2006). Postpartum maternal mortality and cesarean delivery. Obstet Gynecol, 108(3), 541-548.
- DiMatteo, M. R., Morton, S. C., Lepper, H. S., Damush, T. M., Carney, M. F., Pearson, M., et al. (1996). Cesarean childbirth and psychosocial outcomes: A meta-analysis. Health Psychol, 15(4), 303-314.
- Ekstrom, A., Altman, D., Wiklund, I., Larsson, C., & Andolf, E. (2008). Planned cesarean section versus planned vaginal delivery: Comparison of lower urinary tract symptoms. Int Urogynecol J Pelvic Floor Dysfunct, 19(4), 459-465.
- Engle, W. A., & Kominiarek, M. A. (2008). Late preterm infants, early term infants, and timing of elective deliveries. Clin Perinatol, 35(2), 325-341, vi.
- Engle, W. A., Tomashek, K. M., & Wallman, C. (2007). “Late-preterm” infants: A population at risk. Pediatrics, 120(6), 1390-1401.
- Goer, H. (May 11, 2009). Do cesareans cause endometriosis? Why case studies and case series are canaries in the mine. Science andSensibility, 11/12/2009, from http://www.scienceandsensibility.org/?p=147
- Goer, H., Sagady Leslie, M., & Romano, A. (2007). Step 6: Does not routinely employ practices, procedures unsupported byscientific evidence. J Perinat Educ, 16(1), 32S-64S.
- Gray, R., Quigley, M., Hockley, C., Kurinczuk, J., Goldacre, M., & Brocklehurst, P. (2007). Caesarean delivery and risk of stillbirthin subsequent pregnancy: A retrospective cohort study in an english population. BJOG, 114(3), 264-270.
- Hamilton, B. E., Martin, J. A., & Ventura, S. J. (2009). Births: Preliminary data for 2007. Natl Vital Stat Rep, 57(12), 1-23.
- Hansen, A. K., Wisborg, K., Uldbjerg, N., & Henriksen, T. B. (2007). Elective caesarean section and respiratory morbidity in theterm and near-term neonate. Acta Obstet Gynecol Scand, 86(4), 389-394.
- Hansen, A. K., Wisborg, K., Uldbjerg, N., & Henriksen, T. B. (2008). Risk of respiratory morbidity in term infants delivered byelective caesarean section: Cohort study. BMJ, 336(7635), 85-87.
- Hicks, T. L., Goodall, S. F., Quattrone, E. M., & Lydon-Rochelle, M. T. (2004). Postpartum sexual functioning and method ofdelivery: Summary of the evidence. J Midwifery Womens Health, 49(5), 430-436.
- Hodnett, E., Gates, S., Hofmeyr, G., & Sakala, C. (2007). Continuous support for women during childbirth. Cochrane Database SystRev(3), CD003766.
- International Cesarean Awareness Network. (Feb 20, 2009). New survey shows shrinking options for women with prior cesarean.from http://www.ican-online.org/ican-in-the-news/trouble-repeat-cesareans
- Ip, S., Chung, M., Raman, G., Chew, P., Magula, N., DeVine, D., et al. (2007). Breastfeeding and maternal and infant healthoutcomes in developed countries. Evid Rep Technol Assess (Full Rep)(153), 1-186.
- Jukelevics, N. (2008). Understanding the dangers of cesarean birth. Westport, CT: Praeger Publishers.
- Kacmar, J., Bhimani, L., Boyd, M., Shah-Hosseini, R., & Peipert, J. (2003). Route of delivery as a risk factor for emergentperipartum hysterectomy: A case-control study. Obstet Gynecol, 102(1), 141-145.
- Kalish, R. B., McCullough, L., Gupta, M., Thaler, H. T., & Chervenak, F. A. (2004). Intrapartum elective cesarean delivery: Apreviously unrecognized clinical entity. Obstet Gynecol, 103(6), 1137-1141.
- Kennare, R., Tucker, G., Heard, A., & Chan, A. (2007). Risks of adverse outcomes in the next birth after a first cesarean delivery.Obstet Gynecol, 109(2 Pt 1), 270-276.
- Klein, M. C., Kaczorowski, J., Firoz, T., Hubinette, M., Jorgensen, S., & Gauthier, R. (2005). A comparison of urinary and sexualoutcomes in women experiencing vaginal and caesarean births. J Obstet Gynaecol Can, 27(4), 332-339.
- Knight, M., Kurinczuk, J. J., Spark, P., & Brocklehurst, P. (2008). Cesarean delivery and peripartum hysterectomy. Obstet Gynecol,111(1), 97-105.
- Koroukian, S. M. (2004). Relative risk of postpartum complications in the ohio medicaid population: Vaginal versus cesareandelivery. Med Care Res Rev, 61(2), 203-224.
- Labbok M, & Taylor E. (2008). Achieving exclusive breastfeeding in the united states. Washington D.C.: United States BreastfeedingCommittee.
- Larsson, C., Kallen, K., & Andolf, E. (2009). Cesarean section and risk of pelvic organ prolapse: A nested case-control study. Am JObstet Gynecol, 200(3), 243 e241-244.
- Lin, S. Y., Hu, C. J., & Lin, H. C. (2008). Increased risk of stroke in patients who undergo cesarean section delivery: A nationwidepopulation-based study. Am J Obstet Gynecol, 198(4), 391 e391-397.
- Liu, S., Heaman, M., Joseph, K. S., Liston, R. M., Huang, L., Sauve, R., et al. (2005). Risk of maternal postpartum readmissionassociated with mode of delivery. Obstet Gynecol, 105(4), 836-842.
- Liu, S., Liston, R. M., Joseph, K. S., Heaman, M., Sauve, R., & Kramer, M. S. (2007). Maternal mortality and severe morbidityassociated with low-risk planned cesarean delivery versus planned vaginal delivery at term. CMAJ, 176(4), 455-460.
- Loebel, G., Zelop, C. M., Egan, J. F., & Wax, J. (2004). Maternal and neonatal morbidity after elective repeat cesarean deliveryversus a trial of labor after previous cesarean delivery in a community teaching hospital. J Matern Fetal Neonatal Med, 15(4), 243-246.
- Lydon-Rochelle, M., Holt, V. L., Martin, D. P., & Easterling, T. R. (2000). Association between method of delivery and maternalrehospitalization. JAMA, 283(18), 2411-2416.
- MacDorman, M. F., Declercq, E., Menacker, F., & Malloy, M. H. (2008). Neonatal mortality for primary cesarean and vaginal birthsto low-risk women: Application of an “intention-to-treat” model. Birth, 35(1), 3-8.
- MacDorman, M. F., Menacker, F., & Declercq, E. (2008). Cesarean birth in the united states: Epidemiology, trends, and outcomes.Clin Perinatol, 35(2), 293-307, v.
- Makoha, F. W., Felimban, H. M., Fathuddien, M. A., Roomi, F., & Ghabra, T. (2004). Multiple cesarean section morbidity. Int JGynaecol Obstet, 87(3), 227-232.
- Martin, J. A., Hamilton, B. E., Sutton, P. D., Ventura, S. J., Menacker, F., Kirmeyer, S., et al. (2007). Births: Final data for 2005.Natl Vital Stat Rep, 56(6), 1-103.
© 2010 Coalition for Improving Maternity Services. Permission granted to freely reproduce with attribution.
Coalition for Improving Maternity Services (CIMS) Fact Sheet February 2010
The Risks of Cesarean Section Page 6
- McMahon, M. J., Luther, E. R., Bowes, W. A., Jr., & Olshan, A. F. (1996). Comparison of a trial of labor with an elective second cesarean section. N Engl J Med, 335(10), 689-695.
- Mollison, J., Porter, M., Campbell, D., & Bhattacharya, S. (2005). Primary mode of delivery and subsequent pregnancy. BJOG, 112(8), 1061-1065.
- Moore, E., Anderson, G., & Bergman, N. (2007). Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database Syst Rev(3), CD003519.
- National Institute for Clinical Excellence. (April 2004). Caesarean section, clinical guideline. Retrieved 12/18/09, from http://www.nice.org.uk/nicemedia/pdf/CG013fullguideline.pdf
- Nelson, R. L., Westercamp, M., & Furner, S. E. (2006). A systematic review of the efficacy of cesarean section in the preservation of anal continence. Dis Colon Rectum, 49(10), 1587-1595.
- Nisenblat, V., Barak, S., Griness, O. B., Degani, S., Ohel, G., & Gonen, R. (2006). Maternal complications associated with multiple cesarean deliveries. Obstet Gynecol, 108(1), 21-26.
- Pistiner, M., Gold, D. R., Abdulkerim, H., Hoffman, E., & Celedon, J. C. (2008). Birth by cesarean section, allergic rhinitis, and allergic sensitization among children with a parental history of atopy. J Allergy Clin Immunol, 122(2), 274-279.
- Press, J. Z., Klein, M. C., Kaczorowski, J., Liston, R. M., & von Dadelszen, P. (2007). Does cesarean section reduce postpartum urinary incontinence? A systematic review. Birth, 34(3), 228-237.
- Raju, T. N., Higgins, R. D., Stark, A. R., & Leveno, K. J. (2006). Optimizing care and outcome for late-preterm (near-term) infants: A summary of the workshop sponsored by the national institute of child health and human development. Pediatrics, 118(3), 1207- 1214.
- Repeat c-sections climb by more than 40 percent in 10 years. . (April 15, 2009). AHRQ News and Numbers Retrieved 11/13/09, from http://ww.ahrq.gov/new/nn/nn041509.htm
- Richter, R., Bergmann, R. L., & Dudenhausen, J. W. (2006). Previous caesarean or vaginal delivery: Which mode is a greater risk of perinatal death at the second delivery? Eur J Obstet Gynecol Reprod Biol, 132(1), 51-57.
- Rortveit, G., Brown, J. S., Thom, D. H., Van Den Eeden, S. K., Creasman, J. M., & Subak, L. L. (2007). Symptomatic pelvic organ prolapse: Prevalence and risk factors in a population-based, racially diverse cohort. Obstet Gynecol, 109(6), 1396-1403.
- Rotas, M. A., Haberman, S., & Levgur, M. (2006). Cesarean scar ectopic pregnancies: Etiology, diagnosis, and management. Obstet Gynecol, 107(6), 1373-1381.
- Sagady Leslie, M., & Romano, A. (2007). Appendix: Birth can safely take place at home and in birthing centers. J Perinat Educ, 16(1), 81S-88S.
- Sagady Leslie, M., & Storton, S. (2007). Step 1: Offers all birthing mothers unrestricted access to birth companions, labor support, professional midwifery care. J Perinat Educ 16(1), 10S-19S.
- Saisto, T., Ylikorkala, O., & Halmesmaki, E. (1999). Factors associated with fear of delivery in second pregnancies. Obstet Gynecol, 94(5 Pt 1), 679-682.
- Schwarz, E. B., Ray, R. M., Stuebe, A. M., Allison, M. A., Ness, R. B., Freiberg, M. S., et al. (2009). Duration of lactation and risk factors for maternal cardiovascular disease. Obstet Gynecol, 113(5), 974-982.
- Silver, R. M., Landon, M. B., Rouse, D. J., Leveno, K. J., Spong, C. Y., Thom, E. A., et al. (2006). Maternal morbidity associated with multiple repeat cesarean deliveries. Obstet Gynecol, 107(6), 1226-1232.
- Smith, G. C., Pell, J. P., & Dobbie, R. (2003). Caesarean section and risk of unexplained stillbirth in subsequent pregnancy. Lancet, 362(9398), 1779-1784.
- Smith, G. C., Wood, A. M., Pell, J. P., & Dobbie, R. (2006). First cesarean birth and subsequent fertility. Fertil Steril, 85(1), 90-95.
- Spong, C. Y., Landon, M. B., Gilbert, S., Rouse, D. J., Leveno, K. J., Varner, M. W., et al. (2007). Risk of uterine rupture andadverse perinatal outcome at term after cesarean delivery. Obstet Gynecol, 110(4), 801-807.
- Taylor, L. K., Simpson, J. M., Roberts, C. L., Olive, E. C., & Henderson-Smart, D. J. (2005). Risk of complications in a secondpregnancy following caesarean section in the first pregnancy: A population-based study. Med J Aust, 183(10), 515-519.
- Tegerstedt, G., Miedel, A., Maehle-Schmidt, M., Nyren, O., & Hammarstrom, M. (2006). Obstetric risk factors for symptomaticprolapse: A population-based approach. Am J Obstet Gynecol, 194(1), 75-81.
- Thavagnanam, S., Fleming, J., Bromley, A., Shields, M. D., & Cardwell, C. R. (2008). A meta-analysis of the association betweencaesarean section and childhood asthma. Clin Exp Allergy, 38(4), 629-633.
- Tollanes, M. C., Melve, K. K., Irgens, L. M., & Skjaerven, R. (2007). Reduced fertility after cesarean delivery: A maternal choice.Obstet Gynecol, 110(6), 1256-1263.
- Tower, C. L., Strachan, B. K., & Baker, P. N. (2000). Long-term implications of caesarean section. J Obstet Gynaecol, 20(4), 365-367.
- Uma, R., Libby, G., & Murphy, D. J. (2005). Obstetric management of a woman’s first delivery and the implications for pelvic floorsurgery in later life. BJOG, 112(8), 1043-1046.
- van Brummen, H. J., Bruinse, H. W., van de Pol, G., Heintz, A. P., & van der Vaart, C. H. (2007). The effect of vaginal and cesareandelivery on lower urinary tract symptoms: What makes the difference? Int Urogynecol J Pelvic Floor Dysfunct, 18(2), 133-139.
- Whiteman, M. K., Kuklina, E., Hillis, S. D., Jamieson, D. J., Meikle, S. F., Posner, S. F., et al. (2006). Incidence and determinants ofperipartum hysterectomy. Obstet Gynecol, 108(6), 1486-1492.
- World Health Organization. (2009). Monitoring emergency obstetric care: A handbook. France: World Health Organization.
- Yang, Q., Wen, S. W., Oppenheimer, L., Chen, X. K., Black, D., Gao, J., et al. (2007). Association of caesarean delivery for firstbirth with placenta praevia and placental abruption in second pregnancy. BJOG, 114(5), 609-613.
© 2010 Coalition for Improving Maternity Services. Permission granted to freely reproduce with attribution.
About the Risks of Cesarean Section