Tiny URL ~ https://tinyurl.com/y48tcu6g
But first, a brief recap of part 3:
 As described in great detail in Chapter 3, in the centuries before modern obstetrics became available, childbirth in America was a grim and depressing story.
As described in great detail in Chapter 3, in the centuries before modern obstetrics became available, childbirth in America was a grim and depressing story.
For women in general, but particularly for the very young, the working class poor, minorities and immigrant women, the physical health of a large proportion of the childbearing population was awful and their pregnancies high-risk in an era before modern medical science, when there were no treatments for these life-threatening problems.
This sad situation was made worse by social and economic inequities and other factors that often made childbearing more dangerous, and even more deadly.
Progress @ Last!
 Then that situation began to change for the better. The maternal-infant mortality rate began to fall dramatically, as women became healthier and the quality of medical care improved with each passing decade of the 20th century.
Then that situation began to change for the better. The maternal-infant mortality rate began to fall dramatically, as women became healthier and the quality of medical care improved with each passing decade of the 20th century.
Since the mid-point of the 20th century (1950) the standard of living for the majority of Americans has dramatically improved and American women are healthier, wealthier and better educated than ever before in our history.
Compared to the experience of their great grandmothers 50 years ago, the contrast is stunning.
Multiple important discoveries that created the modern world of obstetrical medicine track closely with the improved social and economic situation of the US. When the ability of modern obstetrics to prevent or treat birth-related complications is combined with our dramatically improved standard of living, which includes a vastly healthier, wealthier population of childbearing women, one would naturally anticipate spectacular results for childbearing women living in the 21st century.
Given such facts, obstetricians should have been able to dramatically reduce the number of obstetrical interventions required during labor and birth. One would logically expect a big drop in operative deliveries (episiotomy, vacuum extraction, forceps, and Cesarean section), one that would provide an order-of-magnitude lower rate than the ‘bad old days’ of pre-scientific care.
Along with those improvement, we’d be justified in expecting much lower rates of maternal morbidity and mortality in the 21st century America to match or exceed those of all other wealthy, first-world countries.
However, that just didn’t happen by any measure, either for mothers of babies. The US is way down the list for maternity care outcomes, behind several small, painfully poor 3rd world countries and the rate of medical and surgical interventions is at an all-time high and continuing to rise, while the ratio of good outcomes continues to fall.
Despite the absence of almost every parameter of modern obstetrical medicine, the operative delivery rate in metropolitan hospitals on the East Coast in 1910 was a (not whooping!) 20%.
Our current operative rate of 50-plus percent is inexplicable when compared to the historical context. In the early 1900s, there was NO prenatal care. This earlier generation of obstetrical providers were providing care to a population of childbearing women who did NOT have blood drawn to screen for anemia and syphilis. No one took a personal or obstetrical history or did an initial physical exam. Neither mothers nor their attending physicians had the benefit of ongoing prenatal risk-assessment during pregnancy, no weekly check-ups to access the pregnant woman’s blood pressures, check fetal heart tones, palpation of fetal position or assessment of fetal growth by the sequential measuring of fundal height.
No surprise that pregnancy and childbirth in the early 1900s was dangerous and often deadly, and yet, the rate of operative interventions was less than half what it is today.
The good news is that childbearing women in 21st century American are healthier and wealthier than ever before, have a dozen or more prenatal appointments with blood work, other labs, repeated ultrasounds, genetic testing, regular tracking of BPs, FHTs, fetal growth, etc, haven’t had a case of contracted pelvis for decades, and babies that are electronically monitored every second of the labor . . . .
. . . . . inquiring minds want to know why the operative rate for modern obstetrics is a whooping 50% and maternal mortality is on the rise in our super wealthy country?
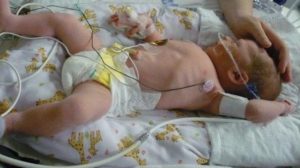 Shocking Reality: The US is one of the very most dangerous developed countries to give birth, both for mothers and babies, with very high rates of intervention, high prematurity rates, and 2- to 3-times greater economic expense than any other country on earth
Shocking Reality: The US is one of the very most dangerous developed countries to give birth, both for mothers and babies, with very high rates of intervention, high prematurity rates, and 2- to 3-times greater economic expense than any other country on earth
How could this be?
Begin part 4A
The ethical dilemmas, technological dichotomies and a skyrocketing Cesarean rate of American obstetrics in the 2st century
How did this come about, why, and what can we do to fix these problems?
The issues facing modern obstetrics and the healthy, 21st century population of women they serve is a conundrum of ethical dilemmas and dichotomies.
Operative Rates: Then and Now
Let’s start with issue of the illogical dichotomy of an operative rates in the early 1900s (the bad old days before modern obstetrics) of only 10 to 20%, compared to the nearly 50% rate (episiotomy, vacuum extraction, forceps and Cesarean) in the first decades of the 21st century.
Given the historical facts, this is illogical.
In the early 1900s, the high levels of maternal ill health and the low-level of development of the medical science made childbirth was 10-to 20 times more dangerous. One example is the extraordinary high maternal mortality rate (MMR) prior to discovery of antibiotics in 1940s. In the year 1925, there were 25,000 maternal deaths, a ratio of 1:80 or one death for of 80 women who gave birth that year.
In our own contemporary times, American women are 10 to 20 times safer, due to being so much healthier and wealthier, and in general having unfettered access to all the services that modern obstetrical science provide.
While the MMR in the US is higher than any other developed country, nonetheless, there are only about 800 maternal deaths annually (compared to 25,000 in 1925), with a ratio that plummeted from 1:80 to 1: 5,000.
With all these encouraging facts, why is the operative delivery rate in America today a whopping 50% or 2 1/2 times higher than then the 20% or less was in 1910?
Maternal Mortality: Historic and Modern
Why does the U.S. have the worst rate for maternal deaths in the world of wealthy developed countries?
And why is maternal mortality rising in the U.S. as it declines elsewhere?
Key findings in a 6-month investigation on maternal mortality in the U.S by NPR and ProPublica were:
- More American women are dying of pregnancy-related complications than any other developed country.Only in the U.S. has the rate of women who die been rising
- Approximately 65,000 come close to dying — severe morbidity in pregnant women and newly-delivered mothers; by many measures, this is the worst maternal health record in the developed world
- Greater prevalence of Cesarean sections leads to more life-threatening complications.
- American women are more than three times as likely as Canadian women to die in the maternal period six times as likely to die as Scandinavians (officially defined by the Centers for Disease Control as starting with pregnancy to one year after delivery or termination)
- Maternal deaths In the U.S. increased from 2000 to 2014; a recent analysis by the CDC Foundation, found nearly 60% of such deaths to be preventable
- Federal and state funding show only 6% of block grants for “maternal and child health” actually go to the health of mothers.
- In the U.S, some doctors entering the specialty of maternal-fetal medicine were able to complete that training without ever spending time in a labor-delivery unit.
ProPublica and NPR used social media to identify more than 450 expectant and new mothers that died in the last 9 years — a list includes teachers, insurance brokers, homeless women, journalists, a spokeswoman for Yellowstone National Park, a co-founder of the YouTube channel WhatsUpMoms.
The cause of these maternal deaths included massive intra-operative or postpartum hemorrhage, pulmonary blood clots, infection and pregnancy-induced hypertension (preeclampsia), as well as rarer causes such as cardiomyopathy and other heart problems. Many of these deaths occurred days or weeks after their babies were born.
A Rational Answer to these conundrums, ethical dilemmas and irrational dichotomies?
It’s totally irrational to allocate 90% of one’s resource to address the rare and unusual, leaving only 10% of the system’s resources to address 90% of the normal and predictable needs of its labor patients.
Currently we have an obstetrical system in the US that focuses a huge percentage of its attention and hospital resources on the management of an obstetrical system that revolves around continuous fetal monitoring and being geared up to deliver one-third of all laboring women by C-section, with “non-reassuring EFM strip” being the 2nd most frequent reason given.
Might this mal-distribution of resources have something to due with this distressing situation? Is our high CS rate the natural consequence of only having 10% of the time, attention and resources of our maternity care system available to meet the minute-by-minute needs of each of the 4 millions laboring women that give birth every year in the US?
What if we flipped those number? —What if we only a lotted 10% of our resources to the technologically-centric aspect of obstetrical care and redirected the remaining 90% to care for laboring women?
There is no doubt that we’d greatly reduce the likelihood that healthy pregnant women with normal pregnancies would l have unplanned, unexpected Cesarean deliveries and be exposed to the many short and long-term complications of this major operation.
Doing that would greatly reduced and the maternal morbidity and mortality and the US would finely compared favorably to other wealthy countries.


