| The Myth of the Ideal Cesarean Section Rate: |
 |
Commentary & Historic Perspective
American Journal of Obstetrics & Gynecology 2006
Clinical Opinion by Dr. Ronald M. Cyr, MD
Fellow in the History of American Obstetrics and Gynecology
This following is the last two pages — p. 935 & 936 — of this published article by Dr. Cry, MD.
Public Policy and the Cesarean Section Rate:
For the past 100 years, the US has lagged behind other industrialized countries in every measure of healthcare quality, including maternal and neonatal mortality. It is a sad indictment of our national priorities that millions of working Americans have no health insurance and inadequate prenatal care.
In Europe, better perinatal outcomes are achieved with lower cesarean rates and less spending on health care. In those countries, midwives manage most low-risk pregnancies, with obstetricians acting as consultants. How did procedure-oriented specialists [i.e., obstetricians] come to perform midwifery and well-woman care in the US?
A hundred years ago, most births occurred in the home. The apparent simplicity of obstetrics contributed to its poor teaching (“see one, do one”), low status and remuneration. DeLee – after Williams, the foremost academic leader of the day – believed that obstetrics would never achieve respect as a profession until “the pathologic dignity of pregnancy” was recognized.(19) This meant accepting the illogical and unscientific premise that most pregnancies are potentially abnormal and using that assumption to decree that all pregnancies be obstetrically managed by experts and rely on multiple interventions thought to be essential to good good outcomes.
This view of parturition deliberately excluded the midwives, who were systematically eliminated by organized medicine on the grounds [unproven claim] that she was untrained, and a threat to the developing “science” of obstetrics. Residency training programs multiplied as births moved to hospitals during the 1920s and 30s. The creation of the American Board of Obstetrics and Gynecology in 1930 formalized the notion that obstetrics was a specialty practiced by surgeons.
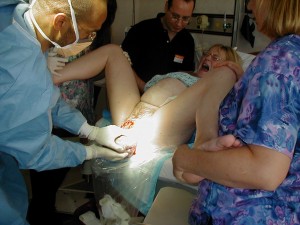
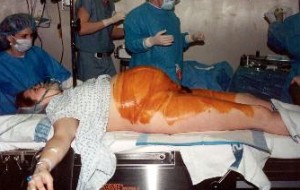
OB-managed “normal birth” with the mother laying flat on her back, doing her best to overcome gravity by pushing her baby uphill while her doctor stands between her legs and pulls her baby out of her vaginia
By the 1950s, birth in America had become a standardized hospital ritual, presided over the procedure-oriented male doctors in solo, fee-for-service practice.
High-volume obstetrics was and remains the bread-and-butter of community specialists – its drudgery offset by the prospect of a busy gynecology practice in middle age.
For specialists, this was the golden era of obstetrics in America. Having successfully promoted themselves as the sole purveyor of expert maternity care in this country, obstetricians took credit for the improvement in maternal and fetal welfare observed between 1940 and the 1970s.
During the last few decades, it has become apparent that more sub-specialization, more technology – and more cesarean sections—have not yielded commensurate benefits to the population. They have, instead, raised patient expectations of perfect outcomes to unrealistic levels, further fueling litigation.
This impasse presents an opportunity to reexamine the way obstetrics is practiced in the US.
In contemplating change, a major goal—after improving access to health care—would be to offer American women more maternity care options than exist presently in most areas.
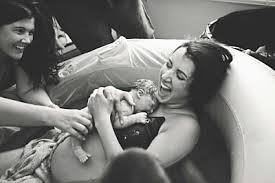
Although trained midwives provide safe obstetrics care, with lower cesarean section rates, they attend only 7% of births in the US – working mostly in an environment where they don’t compete economically with doctors.
@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@
URL for the original post on Collegeofmidwives.org –> https://former.collegeofmidwives.org/Cesarean_2006/AJOG_Myth_IdealCSrate_Exercept_06.htm
So long as most women with health insurance are not complaining about their care, there is little political incentive to change the American way of birth and its high cesarean rate. However, other forces are creating a shortage or mal-distribution of maternity care providers, and this will spur a demand for “alternative solutions”, as fewer family practitioners are delivering babies, while increasing sup-specialization is reducing the number of generalists and marginalizing their role in larger centers.
In truth, the average obstetrician-gynecologist compares poorly to the family practitioner in the breadth of her training for primary care, and there is little office obstetrics and gynecology that cannot be performed competently by midlevel practitioners. In teaching hospitals, the reduced work schedule of residents is creating service needs that can only be addressed by in-hospital personnel.
Because, by training and inclination, obstetricians spend little time and support during labor –why not phase out the generalist (i.e. non-perinatologist OBs) altogether? A self-regulated midwifery profession, working in collaborative practice with consulting perinatologists, would appear to provide a better model for *obstetric care [*actually, the obstetrical model of routine intervention for healthy women with normal pregnancies needs to be 
replaced by the midwifery model of non-interventive care] in the global and historical sense of the term — non-surgical maternity care to healthy women].
In our “quick fix culture”(24), one should not expect the cesarean rate to drop without re-educating the public and the medical profession that most births proceed uneventfully without interference, and that many adverse outcomes can neither be anticipated nor prevented by cesarean section.
Cultural changes take time; it also requires inspired leadership and grassroots support. In the meantime, let everyone practice the best obstetrics [and midwifery!] they know and let the cesarean section rate seek its own level.
