Brave New World of Evidence-based Maternity Care ~ Chapter 6
Chapter 6
~ Scientific Principles & Tort Law ~
Evidence-based Health Care, Normal Childbirth Services,
the modern Practice of Medicine & associated legal implications
faith gibson, LM
Published originally in 2005
 Part I ~ Rule #1:
Part I ~ Rule #1:
Strict Adherence to the Scientific Method
The universal use of the scientific method is what ensures the safety and effectiveness of health-related services, maternity care, medical treatments, prescription drugs and surgery.
Before and After of Modern Science
Prior to development of the biological sciences late in the 19th century, people didn’t know about the world of microscopic organisms or “germs” (bacteria) that caused potentially fatal infections. Even medical professionals never imagined that something so small it couldn’t be seen by the human eye was a living organism that spread dangerously infectious diseases from person to person by personal contact, on unwashed utensils, instruments, and bedding, as well as the clothing and hands of doctors, nurses and their assistants.
Childbirth during the Bad Old Days
An untreatable fatal infection commonly called “childbed fever” or “puerperal sepsis” (blood poisoning) by the medical profession was the most frequent reason that healthy new mothers died after giving birth. In the charity hospitals of western Europe, were poor and homeless women went to give birth, the maternal mortality rate from this septicemia was hoovered around 10% and during epidemic outbreaks in the summer, went as high as 50%.
1881: Before and after the discovery of microscopic bacteria and other germs
 All this began to change in 1881 when the French chemist Louis Pasteur published his “Germ Theory of (infectious) Disease. Other scientists quickly used this new information to develop the principles of “asepsis” and the “sterile techniques” used by surgeons. This required doctors and nurses to scrupulous wash their hands before touching each patient.
All this began to change in 1881 when the French chemist Louis Pasteur published his “Germ Theory of (infectious) Disease. Other scientists quickly used this new information to develop the principles of “asepsis” and the “sterile techniques” used by surgeons. This required doctors and nurses to scrupulous wash their hands before touching each patient.
All medical equipment and surgical instruments had to be scrubbed well with soapy water and brush and then dipped in a germ-killing solution. Soon pressurized-steam sterilizers and large industrial autoclaves were developed to sterilize surgical instruments and institutional supplies.
The Birth of Modern Medical Science
Vigorous application of the principles of aseptic cleanliness and sterile technique reduced the number of patients that got infected, which was extremely important. However, for those unlucky souls that developed septicemia, whatever its origin, there was absolutely no effective treatment. It wasn’t until sulfa drugs and antibiotics became available in the 1930 and 1940s, that what we think of and experience as “modern medicine” came into existence — the ability not only to diagnose but to treat the wide range of human ills became a reality for the first time in the history of the human species.
 Obviously not everyone that is “saved” by modern medical techniques was suffering from a bacterial infection, but without access to effective antimicrobials and antibiotics, emergency room care, many invasive diagnostic procedures and all surgeries would become death-defying feats.
Obviously not everyone that is “saved” by modern medical techniques was suffering from a bacterial infection, but without access to effective antimicrobials and antibiotics, emergency room care, many invasive diagnostic procedures and all surgeries would become death-defying feats.
So many people would die of infections that we would be back to the medical world of the 19th century. As a species, it’s up to us to make wise use of these drugs to keep their therapeutic value from being erased by drug-resistant strains.
Understanding the Scientific Method
The bedrock of scientific theory is simple and straightforward — the efforts of those individuals or groups that want to introduce change into an existing system or substitute a new process or product — new health care principles, drugs, medical treatment, surgical interventions, etc — must be based on the ‘scientific method’.
This is a dynamic process that constantly tests the validity of its theories and conscientiously re-adjusts its conclusions based on new information. This is how the scientific method establishes (i.e. proves) that the new methods are:
- (a) are not harmful or dangerous
- (b) are useful and effective
The legal requirements associated with use of the scientific method
 The legal systems of developed countries require that healthcare and medical services not be harmful or dangerous and also provide whatever positive benefits are promised. This is the most basic level of safety as established by our country’s tort laws. Tort laws identify a legally-enforceable responsibility between individual persons or groups that provide products or services to other individuals or entities.
The legal systems of developed countries require that healthcare and medical services not be harmful or dangerous and also provide whatever positive benefits are promised. This is the most basic level of safety as established by our country’s tort laws. Tort laws identify a legally-enforceable responsibility between individual persons or groups that provide products or services to other individuals or entities.
Historic Principles of Responsibility
Our modern-day principles of legal responsible go as far back as the Code of Hammurabi written by King Hammurabi of Babylon in 1750 BCE. If a Babylonian contracted to build a house for someone, and the roof fell in and someone was badly injured or killed, the builder would be held responsible.
These same principles were reiterated in the book of Exodus and espoused in a more limited form by the ancient Greeks as the Hippocratic Oath “In the first place do no harm” written in 400 BCE. In 1154 CE, the idea of legal responsibility was incorporated into English “common law” by Henry II and then adopted by the 13 British-American colonies very early in our country’s history. By the time we declared independence from Britain in 1776, English common law was a permanent part of our legal system as well.
The principle of legal responsibility is one of the very few things that people from all places and all times have been in agreement. However, there is a step above a simple promise “not to harm” and be clinically “effective” and that is the idea of “value added“. This is the core of all claims made for products or services described as “better” than the same service or product provided by “others”.
While value added is not legally required, it’s very important at a practical level, both personally and to society.
“Value Added” are gains NOT offset by equal or greater losses
After the scientific process had established that the product or process is not harmful or dangerous and is as ‘effective’ as promised, the scientific process can continue to be used to determine whether these new methods are merely equal to to previous product or process, or they represents a substantial improvement or advantage that can legally be defined as “value added” — a benefit that is NOT offset by an equal or greater detriment. In other words, that the new model is NOT significantly more costly without providing any significant gain, or it introduces unpleasant, painful, dangerous side effect or it has potentially lethal side effects.
 The Burden of Proof ALWAYS falls on the individual or group that wants to introduce a new method, process or product
The Burden of Proof ALWAYS falls on the individual or group that wants to introduce a new method, process or product
When using or referring to the scientific method, the burden of proof always falls on those who develop a new idea, product or process. It’s promoters must to establish the merits of its new method or process before being able to legally claim its superiority.
For example, if you want to convince people that “Round-up” weed killer is much better than the centuries-old traditional custom of pulling weeds by hand, you must at the very least prove that chemicals used in your product, when properly used as identified on the product’s label, will not kill the gardener, his family, pets, wildlife, nor will it’s use poison the water source or future vegetable crops.
Once its promoters are able to establish its ‘safety’, it is left up to each individual to choose whether pulling weed is sufficiently onerous to make their chemical ablation preferable. As fully “informed” persons, we define ‘cost-benefit ratio’ for ourselves, which means deciding what ‘benefits’ are worth the costs — i.e. its additional risks and/or expense.
 Bar of “Proof” extremely high when dealing with essential healthy biological states
Bar of “Proof” extremely high when dealing with essential healthy biological states
In regard to the biology of “normal life” – our health and normal bodily functions such as eating, drinking, sex, conception, pregnancy, childbirth, breastfeeding, child rearing practices, normal changes associated with adolescence and aging, etc — society normally holds the bar of “proof” quite high.
We generally require those who wish to introduce change, particularly those that add considerable economic cost, or are potentially dangerous or have restricted access that requires paying for professional services, etc, prove that new way is functionally necessary, safe and cost-effective.
An example of this idea is the drug approval process used by the Federal Drugs Administration (FDA), in which both safety and efficacy (effectiveness and favorable cost-benefit ratio) is factored in to whether or not a drug is approved for use.
Scrutiny when it come to normal biology
This kind of scientific scrutiny specifically applies to the sphere to human biological functions. This includes codes that regulate the sanitary conditions in public bathrooms, restaurant kitchens, swimming pools, hospitals, clinics, blood banks, nursing homes and mortuaries.

New mother breastfeeding her newborn baby
At a personal level, society generally believes that cooking in own kitchen is “better” (more normal and economical) than eating in restaurants or ordering “take-out”.
As for our personal biology, we generally think that fertile couples having sex is a better choice than in vitro fertilization and that breastfeeding, when possible, is more beneficial for mothers and babies and less costly than purchasing prepared formula.
Governments generally recognize that it is unwise, and sometimes harmful, to use an unnaturally large share of finite resources or make something very expensive that is otherwise is freely available, natural, easy and/or economic.
Breastfeeding vs. Formula as a ‘proof of theory’ case study
One easy example of this principle applies to breastfeeding vs. formula feeding and by extension, to the business model for baby formula manufacturers. These milk products are nutritionally adequate to sustain the life and promote the normal growth of human infants. When the baby’s mother can’t or doesn’t want to breastfeed, or she is ill or otherwise unavailable, artificial formulas and bottle feeding are a life-saving substitute for breast milk. We are all grateful that this product is available when needed.
Nonetheless, adequate calories, vitamins and other nutritional elements are not the whole story when it come to feeding newborns and older infants. At a purely biological level, breastfeeding transfers maternal antibiotics to the baby that protect her infant from diseases that the mother has developed an immunity. No mass-produced product can do that. Also it’s extremely unlikely that a baby will be “allergic” to something in its mother’s breast milk (0.5%).
 But even more important and impactful on the overall wellbeing of infants is the bonding relationships that normally develops between mother and baby during its 6 to 10 daily feedings. The very nature of breastfeeding normally provides this emotional foundation without doing anything “special”.
But even more important and impactful on the overall wellbeing of infants is the bonding relationships that normally develops between mother and baby during its 6 to 10 daily feedings. The very nature of breastfeeding normally provides this emotional foundation without doing anything “special”.
While emotional bonding is not impossible with bottle feeding (I was bottle fed), it does require a recognition that the baby still needs to be held firmly and close to the mother (or father, grandparents’ etc) body, and needs to be looked at and talk to while it is drinking down the formula. This is falls into the category of making the best of a less than ideal situation, which is to say that it isn’t the best or first choice.
There was a time when baby formula manufacturers worldwide tried mightily to influence parents to buy formula instead of breastfeeding. They gave away bottles of baby formula to new parents when being discharged from the hospital and they passed out free cans of formula in poor neighborhoods in third-world countries. Once a new mother starts using the free formula instead of breastfeed, her milk supply dries up and these impoverished families are forced to buy formula.
This is such a significant expense that many poor families tried to ‘stretch’ the formula by adding water. But this only resulted an underweight baby that kept getting sick, a situation made worse by the bacteria in the unsterilized water it’s parent added to the bottle of formula. Many of these severely undernourished bottle-fed babies died from malnutrition, making this a case study in how a seemingly simple thing — purchasing manufactured formula rather than breastfeeding — can result in extremely unfortunate outcomes somewhere down the line.
Scientifically-speaking, formula manufactures have a legal duty to inform parents that breastfeeding is the best all-round process for feeding infants when possible. However, for new mothers that cannot or do not want to breastfeed, or nursing mothers that need to supplement their milk supply, their company’s artificial baby formula will safely meet their infant’s nutritional needs.
This “warning label” should be printed on every case of manufacture baby formula.
Avoiding the cascade of complications triggered
by a supposed “simple” medical intervention
Imagine for a moment that medical supply companies selling urinary catheters claimed the routine use of their product was somehow easier or better than just going to the bathroom to empty our bladders the “old-fashioned” (i.e. normal) way. Under those circumstances, we would all come from the “show me” state of Missouri!
 However, there is not a shred of scientific proof to uphold such an outrageous claim — the cost of sterile catheter sets and the complex machinations of using such a product every time you had to pee would be a non-starter for most people.
However, there is not a shred of scientific proof to uphold such an outrageous claim — the cost of sterile catheter sets and the complex machinations of using such a product every time you had to pee would be a non-starter for most people.
Published studies on the safety of catheterization report that this procedure results in a bladder infection 1% of the time, which often requires antibiotic treatment.
Some cases of cystitis are resistant to these drugs, while others progress to a kidney infection (pyelonephritis), which is far more serious. Kidney infections can also become resistant to antibiotics and the side effects of the drugs, even when effective, can trigger other problems that lead to kidney failure or liver damage.
Without dialysis or a kidney transplant, these unwitting and unfortunate victims will die from a totally preventable, man-made problem, something originally described by its adherents as the new and better way, something benign, “safe, simple”, just a “minor” medical procedure.
Part II: What the (heck) does this have to do with contemporary obstetrical practices?
Part II: What the (heck) does this have to do with contemporary obstetrical practices?
 This same scientifically-mandated “burden of proof” and tort laws apply to the entire premise of obstetrical care for healthy women with essentially healthy pregnancies. But unfortunately, obstetrics in America is not scientifically-based when the mother-to-be is healthy and has a normal term pregnancy (70-85% of the childbearing population in the United States).
This same scientifically-mandated “burden of proof” and tort laws apply to the entire premise of obstetrical care for healthy women with essentially healthy pregnancies. But unfortunately, obstetrics in America is not scientifically-based when the mother-to-be is healthy and has a normal term pregnancy (70-85% of the childbearing population in the United States).
The routine use of obstetrical interventions is a “wrong” use of obstetrical medicine. No scientific studies have identified the routine use of obstetrical interventions to be better (safer for mothers and babies) than simple non-interventive support for the normally progressive biology of labor and birth.
This is a shame, as obstetrics was historically developed to give doctors the ability to intervention when something went wrong and there was a complication that threatened the life or well-being of mother and/or unborn baby.
Obstetrical interventions should only be used by those who need them — women with very high-risk pregnancies, those who developed complications or suffered an obstetrical emergency. In that case, obstetrical medicine does a splendid job, for which we all (myself included as a former L&D nurse) would be enormously grateful.
The Wrong Use of Obstetrics ~ Protocols typically associated with the obstetrical model are NOT currently “evidence-based”
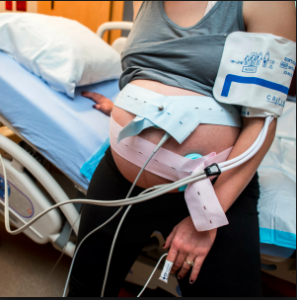
Hospital admission of an obstetrical patient typically begins by immobilizing the mother-to-be in bed and immediately hooking her up to the electronic fetal monitor (EFM 89%). As a result, the vast majority of healthy labor patients spend more than 90% of their labors lying in bed. According to the University of Minnesota “Taking Charge” website:
After the mother is wired up the EFM, most labor protocols include routinely starting an IV (66%) and, in many places, restricting oral fluids (60%) and food (79%). Depending on the situation, Pitocin is 0ften started to either induce (20-to-40%) or “aumentent” (speed up) the labor (31%, or total of ). An article in the Wall Street Journal (Landro, July 12, 2006) had this to say about the drugs used to induce labor and the way it is used and thought of by the obstetrical profession:
“The most common brand name is Pitocin, which is a synthetic version. It’s often used to speed or jump-start labor, but if the contractions become too strong and frequent, the uterus becomes “hyperstimulated,” which may cause tearing and slow the supply of blood and oxygen to the fetus. Though there are no precise statistics on its use, IHI says reviews of medical-malpractice claims show oxytocin is involved in more than 50 percent of situations leading to birth trauma.
“Pitocin is used like candy in the OB world, and that’s one of the reasons for medical and legal risk,” says Carla Provost, assistant vice president at Baystate, who notes that in many hospitals it is common practice to “pit to distress” [i.e. to give progressively larger doses of Pitocin until the mother either delivers or the baby goes into fetal distress].
Among women who labor in a hospital obstetrical unit, 67% will have Epidural anesthesia. The standard “delivery” position still has the mother lying on her back, most often with her legs and feet in obstetrical stirrups. The Cesarean surgery rate in the US is currently 31%,
According to the Listening to Mothers Survey, more than 90% of hospitalized women receive 7 (or more) obstetrical interventions, which includes pharmaceutical products such as narcotic drugs, labor accelerating hormones (Cytotec and prostaglandins), and obstetrical instruments such as forceps and vacuum extractors.
How do we know that this is still true? Will here are the numbers from the “horse’s mouth” so to speak — peer-reviewed professional journals that publish scientific studies by obstetricians and other researchers:
According to a statement by the American College of Obstetricians (ACOG) Jun 11, 2015
Thirty percent of women in the United States have their spontaneous labors stimulated with exogenous oxytocin (Pitocin; Declercq et al., 2013) and 20 percent to 40 percent of labors are now induced.
According to the Mayo Clinic, the disadvantages of inducing labor a significant number of serious risks including:
- Failed induction 25 percent in first-time mother
- Low fetal heart rate. …
- Infection. …
- Uterine rupture. …
- Increased bleeding {hemorrhage} after delivery.
Inducing labor: When to wait, when to induce – Mayo Clinic
https://www.mayoclinic.org › in-depth › art-20047557
As published in the Journal Of Perinatal Education, a research paper titled “Healthy birth practice #4: avoid interventions unless they are medically necessary” …
link to a free PDF @ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6503899/
“Maternity care in the United States continues to be intervention-intensive, despite substantive evidence that the routine use of intervention without medical indication increases risk for mothers and babies.”
-
-
- 89% of women experienced electronic fetal monitoring (EFM)
- 79% experienced restrictions on eating
- 67% of women who gave birth vaginally had an epidural in labor
- 66% have continuously IV infusion
- 62% received intravenous fluids at some time during labor
- 60% experienced restrictions on drinking in labor
- 31% were given Pitocin to speed up their labors
- 31% had a cesarean
- 20% had their membranes artificially ruptured
- 17 % of women had an episiotomy
-
@@@@@@@@@@@
Historically this “burden of proof” as applied to medicine was known as “positivism” and is one of the foundational principles of the Scientific Age (cite Cry and the Covenant). Individuals holding or wishing to promote a particular theory were required to prove the validity of their theories on objective grounds. In the “big picture” of maternity care for a healthy population, it would be necessary to evaluate the overall necessity and safety of obstetrician management versus physiological management. In the small picture is the need to look at each and every procedure and products to determine its direct safety and the potential for their use to lead to a cascade of complications. This burden of scientific proof cannot be met for the routine medicalization of normal birth any more than for the routine medicalization of bladder function, as each of these interventions introduces unnecessary and unnatural risk when applied to healthy women with normal pregnancies.
A very small example of the problem associated with what appears to be ‘minor’ interventions is the association between epidural anesthesia and bladder infections. Most women with an epidural are not able to spontaneously empty their bladder because they have lost feeling in their lower body. They are also receiving large quantities of IV fluids to counteract the blood pressure lowering effects of the epidural drugs. So the majority of anesthetized women require urinary bladder catheterization. Sometimes are given what is called an indwelling or “Foley” catheter that is left in place during the many hours of labor and even while the mother is pushing (a practice that can damage the mother’s urethra). At a minimum, 1% of these mothers will develop a bladder infection during the postpartum; a few will wind up with a kidney infection and the potential for all the other complications that are associated with pyelonephritis.
However Foley catheterization is not the only danger the mother will be exposed to, as each increment of intervention has the potential to trigger a cascade of complications. In addition to the rubber urinary catheter, she will also have an small plastic epidural catheter taped to the her back, an automatic blood pressure cuff that goes off automatically every 15 minutes. In many hospitals, she will also have a pulse oximetry devise on one of her fingers. There are usually two intravenous lines (the second for Pitocin which is a frequent accompaniment of epidural anesthesia), two external EFM belts (or an internal fetal monitor leads and sometimes, even a uterine pressure catheter) and of course, the Foley catheter and its bag clamped to the lower side of the bed. Entanglement in this massive quantity of equipment (8 wire leads and plastic tubes) that effectively chain the mother to the bed and frequently result in her lying prone and immobilized for most of the hours she is in labor. According to the obstetrical profession, however, none of this interferes with the natural function of the pregnant uterus or ‘spontaneous’ nature of childbearing – at least not in their minds. The opinion of mothers might well be different, especially if those who finds themselves in the unlucky 30% of healthy women who wind up with operative deliveries – forceps, VE or Cesarean surgery.
Pharmaceutical and mechanical interventions do provide a way for physicians to control the interaction between themselves and the mother as well as the timing and the manner and circumstance of normal birth. Our 20th century technological society has been having a romance with control with over our biology – a natural desire to reduce the unexpected and inconvenient. We firmly believe that our superior intellect and the superb technological capacity of the US makes it possible to control everyone and everything, that we positively deserve to be in control, particularly over our own normal biology. Over the course of the last 100 years, that propensity to control bodily functions has included the use of various drugs on a routine or casual basis to manipulate bodily functions.
In the early 1900s the idea of controlling normal bowel function through the use of laxative was very popular. Eventually a public education campaign was undertaken to disabuse the public of the notion that laxatives were an “improvement” and teach that an appropriate diet and drinking water was safer and better than drug dependency. There was a period of time when the casual use of prescribed sleeping pills was very “in”. Eventually the down-side of their use became apparent, which was disturbed sleep patterns in which the deep dreaming phase of sleep (responsible for feeling refreshed the next morning) was missing. These problems spawned a public re-education campaign exposing the dangers of barbiturate use.
For a while women were instructed that a proper lady must douche after a menstrual period and more often if she wished to be fastidious or welcomed into polite company – also a notion that was without merit and caused many unintended side effects. Many Americans have sought out aphrodisiacs of various kinds and now we have the dubious benefits of Viagra available to the male populations. And of course, the control of appetite and eating is our biggest favorite with various prescription and OTC diet pills abounding. With the possible exception of Viagra, virtually all these medicinal interventions designed to manipulation of normal bodily function has been debunked, at least among the more well informed public.
Historically speaking, obstetricians also have been having a romance with control. In particular, they have long desired to have total control over the physical act of childbirth through the use of labor stimulating drugs and narcotics so that the mother could better tolerate other surgical interventions such as instrumental delivery and manual removal of the placenta. The obstetrical profession has always seen itself as revolutionary and responsible for defining all aspects of pregnancy and birth care, including the politics of childbearing and our national maternity care policy. A historical example of this is a quote from the February 23, 1911 edition of the Boston Medical and Surgical Journal, page 261]
We believe it to be the duty and privilege of the medical profession of American to safeguard the health of the people; we believe it to be the duty and privilege of the obstetricians of our country to safeguard the mother and child in the dangers of childbirth. The obstetricians are the final authority to set the standard and lead the way to safety. They alone can properly educate the medical profession, the legislators and the public”
What we must first do is arouse public sentiment and first of all we must have the enthusiastic support and united action of the medical fraternity…. We feel that the most important change should be in the laws governing the registration of births. The word “midwife” as it occurs, should be at once erased from the statute books. … [Boston Medical and Surgical Journal, Feb. 23, 1911, page 261]
@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@@
New Chapter ???
The Scientific Method applied to equipment developed to listen to the unborn baby’s heart rate during labor: traditional fetoscope, hand-held Doppler vs. continuous electronic monitoring (EFM)
A contemporary example that directly affects women in labor is the type of equipment used to listen to the unborn baby’s heart rate and rhythm during labor. This is a normal part of the care provided by midwives, nurses to laboring women. They listen to the fetal heart every hour or so and then more often it get closer to the birth of the baby. This is to make sure the baby is tolerating the physical stress of active labor.
 |
 |
 |
| Fetoscope | Hand-held Doppler | Continuous EFM |
HISTORY: The equipment used to listen to the fetal heart rate traces back to 1816 when a physician in Paris, Dr. Rene Laennec, invented the stethoscope so he would not have to place his ear against the bare a woman patient’s chest in order to listen to her heart.
 In 1819 Dr. Jacque Kergaradec, a former student Dr. Laennec who was now an obstetrician, placed his stethoscope on the abdomen of a pregnant woman and heard the distinctive sounds of fetal heart tones. He described hearing “the movements of a watch placed very close to me.” It occurred to Dr. Kergaradec that variations in the fetal heartbeat would allow doctors and midwives to monitor the health of the unborn baby during pregnancy and when the mother-to-be was in labor.
In 1819 Dr. Jacque Kergaradec, a former student Dr. Laennec who was now an obstetrician, placed his stethoscope on the abdomen of a pregnant woman and heard the distinctive sounds of fetal heart tones. He described hearing “the movements of a watch placed very close to me.” It occurred to Dr. Kergaradec that variations in the fetal heartbeat would allow doctors and midwives to monitor the health of the unborn baby during pregnancy and when the mother-to-be was in labor.
The Constitutional Nature of Obstetrics: One could say that the obstetrical profession felt a certain divine appointment as if their “right” to control dominate and monopolize all things related to childbearing and maternity care was constitutionally established.
According to obstetrical folklore:
“We hold these Truths to be self-evident:
That normal birth is abnormal and dangerous
That doctors and hospitals make normally abnormal birth safer
That the intrinsically pathological nature of birth routinely requires the skills
of a surgical specialist and the use of drugs and anesthesia
That healthy women cannot cope with normal labor
That normal birth is too painful to occur without anesthesia
That midwives, who are not MDs are inadequately trained to safely handle normal childbirth
That midwifery care introduces unrealistic expectation and unnecessary danger
That midwifery care is inherently unsafe because it prevents women from being cared for by an obstetrician”
Obstetrics for Healthy Woman – Value Added or Value Subtracted?
Historically, the obstetrical profession established itself as ”value added” over what had traditionally preceded it, which was midwifery as an organized profession or vocation. Before anyone can thoughtfully examine the merits of their claim to superior abilities, one must first define the foundational “value” of midwifery as the standard for maternity care to which obstetrics becomes the “added” quality.
Midwifery has traditionally been a combination of services relative to both childbearing and childrearing. The mother’s physical safety was addressed through prenatal care, one-on-one labor and birth management. The ‘soft’ side of birth services include providing the emotional and social services so central to the development tasks of childbearing women. Meeting these “soft” needs, which addressed the quality of motherhood itself, are built into the midwifery model of care. The midwife’s role included ‘mothering the mother’ so that the mother was empowered to better ‘baby the baby’. This included the provision of “comfort measures” during labor, help with the new baby, preparing or serving food and drink, helping with personal hygiene and bodily function (such as perineal care, getting the mother up to go to the bathroom and changing soiled linens) and educating the mother about milk production, breastfeeding, newborn care (diapering, dressing and bathing the baby), normal child development and when to seek out healthcare services or emergency medical care relative to her or her baby’s well being.
Midwifing as a verb was an extension of mothering and practiced mostly by older women who were experienced mothers themselves. They were pleased to be able to contribute the benefits of their personal experience back into the system by becoming a professional caregiver later on, after having raised a family. At this point, the average midwife has developed a depth and breadth of mother-friendly abilities that are of great cultural value. Her ability to bring to these services to other women and families during the childbearing years is at the heart of the art of midwifery.
Obstetrical version of “value-added” was, from the start, only half a loaf. Doctors immediately jettisoned all professional responsibility for “soft” services – the intimate personal care of the mother during the long hours of labor and care of her and the baby after the birth. These “soft” or feminine services were considered to be beneath the dignity of a male doctor, as well as a waste of a medical education. When faced with patients in need of this type of care, obstetricians enlisted other “helpers” to provide the nursing/caregiving aspects of midwifery during labor and the postpartum period. Nurses and other para-professionals were employed to assist the mother with all aspects of recovering from childbirth, establishing breastfeeding and care of herself and the new baby.
This paved the way for doctors to focus solely on “adding value” to the medical management of pregnancy and the last few minutes of labor, delivery of the baby and placenta. It is immediately clear that this is a very diminished version of ‘maternity’ care. In a simple contrast between the two systems, obstetrics would come off badly, as the services they provide would have to be augmented by many other assistants and members of other professions. Reduced to “face time” their contributions would seem trivial. This certainly would not be economically competitive, were it seen as a comparison of “like with like” – obstetrician versus midwife as equal provider of normal childbirth services.
However, the official strategy of organized medicine was to unilaterally change the definition of childbirth, thus eliminating the idea that childbirth was a normal aspect of healthy biology and thereby eliminating any basis of comparison between the two professions. During this same period of history, childbirth was seen by the public and by midwives as a normal biological process. This continues to be one of the officially unique aspects of midwifery as compared to obstetrics. The Maternity Center of New York, an organization that has been providing nurse midwifery services for more than 80 years, still uses the fundamental definition of childbirth as a “normal biological process” and not one benefiting from routine medical interventions. Midwives and most mothers saw the arduous aspect of labor and birth as having value in their own right and as contributing to the overall well being of the mother and baby. These biological processes were expected to occur “unaided by steel or brawn” (cite Alan Gutenbacher book, 1937) unless a problem or complication arise that signaled the need for external help, in which case the obstetrician’s specialized surgical skills were solicited and appreciated.
Organized medicine formally turned this historical relationship upside down and backwards – characterizing childbirth as intrinsically pathological and dangerous and requiring the skill of a surgeon. This medical model as generated in the early decades of the 20th century redefined pregnancy as a “nine-month sickness requiring a surgical solution”. In 1911 a well-known obstetrician stated: “For the sake of the lay members who may not be familiar with modern obstetric procedures, it may be informing to say that care furnished during childbirth *is now considered, in intelligent communities, a surgical procedure.” [1911-D, p. 214]. *emphasis added
In 1915, another famous obstetrician (Dr Joseph DeLee), incorporated a remark by a 19th century ethnographer of childbirth in primitive cultures (Engelman) in his own comments: “ ‘The parturient (i.e., laboring woman) suffers under the old prejudice that labor is a physiologic act,’ and the profession entertains the same prejudice, while as a matter of fact, obstetrics has great pathologic dignity —it is a major science, of the same rank as surgery”. [1915-C; De Lee MD p. 116]
In contemporary obstetrical parlance, this idea is restated as “birth is only normal in retrospect”. One of the major advantages of this notion is that it keeps the obstetrical profession from having to provide any personal care to the mother or assume any responsibility for the social dimension of childbearing – it redraws the lines of professional responsibility to the realm of high-tech medicine, confined primarily to a focus on the fetus and the delivery rather than either the mother or newborn baby once the delivery is completed. It also confuses the idea of obstetrics as “value-added” to the traditional childbirth services of midwifery, as it is no longer a comparison of “like with like”. By rejecting the whole idea of ‘normal’ (“birth is only normal in retrospect”) it obfuscates and confounds any outside examination of relative quality of care.
Like nuclear scientists and Federal Reserve chairman Alan Greenspan, these areas are portrayed as too complex and technical for ordinary folks to understand. Obstetricians insist that the lay public just doesn’t realize all the things that can go wrong. They are quite convinced that the public doesn’t appreciate how hard doctors must work to keep mothers and babies from being damaged or dying from what obstetricians describe as the “frequent and sudden disasters” that routinely befall “even the most normal of labors or births”. For the last 90 years the obstetrical profession has promoted the idea that all the problems of unpredictable Mother Nature (i.e., the flawed biology of the childbearing women) could and would be successfully eclipsed by “modern” obstetrical care. The implied (and sometimes stated) concept was that employment of a surgically skilled obstetrical specialist – that is an obstetrician and ONLY an obstetrician — was a virtual guarantee of a “good outcome”. This resulted in a biased presentation of the need for and value of obstetrical services for healthy women. Unfortunately, the claim to god-like powers also gave rise to a host of unrealistic (and unrealized) promises which only added to the likelihood of malpractice litigation, a nightmare come to roast in the last 25 years.
The fallacious idea of obstetrical surgeons snatching healthy women and their unborn or newborn babies back from the jaws of death permitted the obstetrical profession to side-step the issue of whether or not its standard (i.e., unscientific) management of normal birth is, in actual fact, as safe or “efficacious” as that of non-obstetrician maternity caregivers – general practitioner MDs, family-practice doctors and professionally licensed midwives. Most important, the fiction of obstetrical practice for healthy women as “value-added” continues to allow the obstetrical profession to charge extra for their pregnancy and birth services, just as the brain surgeon or cardiac specialist charges are higher than GPs or nurse practitioners. The myth of “value-added” services is all based on the idea that pregnancy and birth related services as provided by obstetricians to healthy women improved outcomes, was safer, was more technically complex, and more satisfactory to its recipients – than care as provided by non obstetricians, especially that of professional midwives.
This permits “creative” bookkeeping – that is, the quality of deceptive accounting methods, recently made infamous by the firm of Author Anderson — in which information that is clearly detrimental is moved to the other side of the ledger and reported as a positive factor. Obstetrical sources (such as research published in peer-reviewed journals) consistently replace the simple reporting and honest accounting on such topics as spontaneous vaginal birth rate for healthy women under obstetrical management, Cesarean rates for OBs, GPs and midwives, the safety, long term side effects and cost-effectiveness of the dozen or so routine interventions (bed rest, IVs, ARM, electronic fetal monitoring, Cytotec use, elective induction, routine acceleration of labors, epidural anesthesia, episiotomy, vacuum extraction, etc) by not counting the things that actually “count” most – the falling rates of spontaneous vaginal birth and increasing need to use other medical and surgical treatments. This failure to mention what counts most is matched by counting the secondary or irrelevant issues in double digits (such as legal protection for the physician or reduced costs to the HMO).
A minor example of this “cooking the books” is an obstetrical study by on the relative benefit of “permitting” hospitalized women to walk during labor versus women who received the typical or “standard” hospital bed rest. It would seem that this research was an attempt to prove that midwifery management, which uses the upright and mobile mother as a mainstay of maintaining a spontaneously progressing labor, was all wrong. In the study the supposedly “walking” group of mothers in fact walked less than 50 feet over the course of their entire labor, as contrasted with the bed rest mothers that walked less than 25 feet. When women walk as a part of physiological management they are often on their feet and moving about during labor for many hours and typically walk more a ½ mile or so, sometimes as much as a mile or even two. Despite the fact that this obstetrical study did not actually contrast “like with like”, it was published with great fanfare as the “final” authority on the topic. According to its author, the issue had been decided once and for all by “debunking” the myth that walking during labor was helpful or made any difference at all as their study found no statistically significant difference in the rate of progress in labor or spontaneous births between the two groups.
A great deal of contemporary obstetrical medicine is organized around and devoted to concealing the incongruity between the idealized goals of “value-added” services in the form of greater safety and realistic reality of what obstetrical management actually does, which is the routine recommendation of a host of techniques and procedures that obviously introduce unnatural risks – often the very ones supposedly reduced by that very medical procedure. An example that comes instantly to mind is the routine use of continuous electronic fetal monitoring (EFM) to as a strategy to prevent fetal distress but which ignores (ig-nore — to not-know what is known) the deleterious effect of anti-gravitational positions its use entails and the total disruption of any opportunity for non-drug dependent pain management when continuous EFM is used. It is well established that when the mother is confined to bed in a prone position (lying down) this can be expected to interferes with blood circulation to the uterus. This creates or acerbates fetal distress and the need for emergency cesarean section, which a gift that “keeps on giving”, as the unborn baby in the next or “post-cesarean” pregnancy now becomes vulnerable to fetal distress resulting from uterine rupture – all in the name of reducing fetal distress via the wonders of continuous electronic fetal monitoring.
However, not even the obstetrical profession has been able to hermetically seal the border of our country or our minds from the world-wide realities of other, older health care systems that do not share this notion of birth as inherently pathological. Countries with the very best maternal-infant outcomes have been successfully providing safe maternity care, some for as long as 200 years, that was based on the midwifery model of physiological management. Whether from historical or contemporary sources, a scientific inquiry of safety in childbirth always documents the efficiency of normalizing labor and birth and minimizing the use of medical or surgical interventions. Studies that contrast specialist physician care versus professional midwives always favors the midwife. Studies that examine the relative safety of the co-management of doctors and midwives versus midwife-only care again favor the midwife as the solo primary caregiver.
Recognizing this immutable truism permits us to returns to the legitimate question, “can the obstetrical profession document that its typical ministrations to healthy women with normal pregnancies and spontaneous labor and births actually has ‘added-value’ over and above either professional midwifery care or an unattended birth?” One must look at direct and indirect expenses (the cost of medical education plus maintaining institutions able to provided intensive care nursing) and examine the quality of the care provided – does it meet both the biological needs (such as right use of gravity) and the emotional and social needs of the new mother and her necessity to take on the expansive role of motherhood and to learn both parent craft as well as being supported in her efforts to maintain stable and satisfying relationships with her spouse and other family members.
For healthy women with normal pregnancies who do not want or need labor inducing or accelerating drugs, narcotics pain medications, anesthesia or operative delivery, the “standard” obstetrical care is value-subtracted from the Midwifery Model of Care.
Next in series: Chapter 7 ~ Hospitals: Help or Hazard?
@@@@@@@@@@@@@@@@@@@@@@@@@@@@
Reference:
Code of Hammurabi 1705 to 1755 BC consisted of 282 laws. They are one of the earliest and more complete written legal codes from ancient times and have served as a model for establishing justice in other cultures. They also are believed to have influenced laws established by Hebrew scribes, including those in the Book of Exodus.
