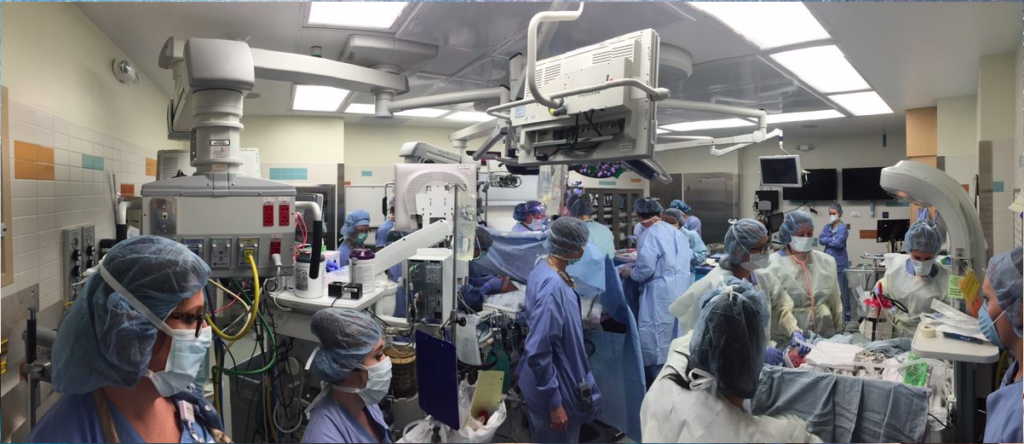
Semi-comatosed patient laboring under the influence of Twilight Sleep drugs, restrained with a straight-jacket so she can’t hit or bite the nurses and straps across her chest tired to the bed rails so she won’t fall out of bed and chip a tooth or break an arm
- Public dissatisfaction in 1950s with half a century of highly-medicalized and invasive “Knock’em-out, Drag’em-out” obstetrics ~
- Push-back by public opinion that rejects information about normalizing normal childbirth ~
Public dissatisfaction with childbirth practices first came to light in mid-1950s, when a popular women’s magazine published a ‘whistle-blower’ article by a Labor and Delivery nurse.
As a personal eye-witness, she was reporting on the systematic and institutionalized harm being done to mothers and unborn babies, and even physical abuses by the L&D staff. This was directly associated with the use of Twilight Sleep drugs during labor and routine use of general anesthesia for normal birth, which was defined as a surgical procedure conducted by a physician-surgeon on an unconscious woman.
The article was followed by a flood of letters to the magazine by other L&D nurses, a few doctors and many women who vividly remembered being abused in the hospital during their labor and birth.
This publicity created a ‘grassroots’ movement made up of consumer groups (childbearing women and family members), childbirth preparation/education instructors, nurses, and professional midwife groups who mobilized to stop these abuses and generally improve maternity care in the US.
Changing this obstetrics-centric system turned out to be a lot harder than anyone imagined. When it comes to childbirth services, the obstetrical profession is the 800-pound gorilla on the block, and they don’t let anyone or anything get pass unless its to their advantage.
In addition, there are two things the obstetrical profession never does, not historically or in contemporary times.
American Obstetrics – never admitting it was wrong, never saying “Sorry”, never agreeing stop using harmful or objectionable practices
The fatal character flaw of the American obstetrical profession has two parts, the first being their inability to ever admit that any of their official policies, practices or protocols were proven over time to be wrong. This inability to admit to the plain but somethings painful truth has always been a characteristics of obstetrics, one that applied with vengeance in the distant past and is still the case.
An infamous historical example from two centuries ago is that of Dr. Semmelweis. In the 1840s, he was obstetrical resident in an Austrian medical school that provided clinical training to its students in Vienna’s large general hospital. As a grad student, he conducted his own scientific research on the deadly infection known as ‘childbirth fever’, which routinely killed 5% to 20% (during some brief periods as high as 50-75%) of the women who delivered in his hospitals.
Dr Semmelweis was able to provide strong evidence to his professors that this lethal infection was being caused by the purulent (pus, white blood cells) material under the fingernails of the professors and medical students who performed autopsies on women who had just died of childbirth fever. We must note that it would be many more decades before latex exam gloves were invented, so doctors and med students were using their bare (ungloved) hands. This was also a century before antibiotics became available.
After finished for the day, the professor or senior resident and his students wiped their fingers on a rag, rinsed the remaining blood off in a bucket of water, dried their hands on their lab coats, and then unknowingly carried this virulent germs under their fingernails into the labor ward. Unfortunately, these professors rejected Dr. Semmelweis’s idea out-of-hand. To them, the idea that pus and infected organic material on the hands and under the nails of doctors and interns was causing women to die simply ludicrous.
As hospital policy, these professors flatly refused to require (or even allow) their medical students to wash their hands in an antiseptic solution after dissecting cadavers, and before and after doing pelvic exams on each labor patient. As a result, this deadly infection was systematically spread to every woman in the labor ward, with a large percentage of newly-delivered mothers dying from the preventable disease of puerperal sepsis (septicemia or ‘blood poisoning’).
The Right Use of Obstetrics is Life-saving, while its inappropriate use is a preventable problem
We all agree that obstetrical medicine, with its cornucopia of medical interventions and surgical procedures, has the potential to be life-saving in life-threatening emergencies. For that, we have great respect for obstetrical medicine and are profoundly grateful for what that means to mothers and babies that need this kind of care. However, the stated goal of the American obstetrical profession in the early 1900s was not to simply be called in as consultants and surgeons when needed; the surgical speciality of obstetrics and gynecology wanted nothing less than to to “own” — have total control over — all childbirth services.
Hospital-based obstetrical services, as developed by leading obstetricians of the day (in particular, Dr. J. Whitridge Williams, Dr. Joseph DeLee) included an astonishingly long list of ‘routine’ but painful and potentially dangerous interventions that were used on healthy women who did not need or benefit from these risky procedures. The history of obstetrics is a history of iatrogenic harm that was both systematic and institutionalized and resulted in unnecessary, painful, often humiliating, risky or dangerous policies, practices or protocols becoming the Standard of Care in the United States.
The second thing is the obstetrical profession et al never ever says is: “sorry”, nor do they promise to stop practices identified as harmful or unnecessary and going forward NOT to institute new policies, practices and protocols without first including feedback from the primary “stakeholders” in maternity care — childbearing families, birth educators, midwives, and economists with expertise in healthcare-related costs.
This beating heart of this issue is the obstetrical community’s relationship with physiological management of childbirth, which is to say their LACK of a relationship with or knowledge of physiologically-based care. As represented by ACOG, the obstetrical profession as a group continues to reject out-of-hand, while promoting more and more interventions in the labors and births of healthy women with normal term pregnancies. In the 1980s, obstetrical leaders pushed the idea that vaginal birth was so dangerous to babies that it should be replaced with universal use of ‘prophylactic’ Cesarean section as the new standard of care.
For a variety of reasons (cost and the increasing rate maternal mortality associated with immediate and long-term complications of Cesarean surgery), Cesarean, at least so far, has not become the ‘standard’ for normal childbirth.
Special Delivery/Operating Room for women with a placenta accreta, a frequent complication of a previous C-section
However, the obstetrical profession’s newest plan to disrupt and disregard physiologically-based childbirth is to insist that all pregnant women be electively induced the week BEFORE their baby is due — sometimes in the 39th week. Studies currently being circulated in peer-review (reviewed by obstetricians for obstetricians) assure us that systematic and mass-scale induction of all pregnant women as the 21st century way to give birth is safer than waiting for the spontaneous onset of normal labor, does not increase the C-section rate, and saves the lives of at least one baby per 1,000.
The new norm for ‘normal’ childbirth ~ hospital induction

Two Steps Forward, one-and-half steps backward!
Success in this endeavor has been a mixed bag – a lot small and a few big successes. However, nothing any of these groups has done has been able to substantially changed the“American model of childbirth”as a hospital-based obstetrical procedure. This expensive system is unquestioningly reimbursed by health insurance companies and the federal Medicaid program. Currently, 50% of all births in the US are paid for by Medicaid.
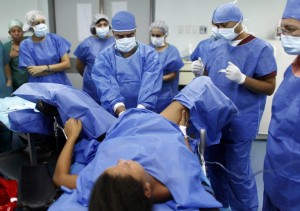 While husbands are now allowed to be present during the labor and birth, and childbearing women now labor and give birth under epidural anesthesia instead of general anesthesia, the cultural assumption of the early 1900s remains intact in the 21st century in the US– the illogical idea that obstetrically-trained surgeons should control the entire maternity care system, be the primary providers for healthy childbearing women and that more and more medical and surgical interventions used earlier and more often is the very best way to ‘improve’ maternity care.
While husbands are now allowed to be present during the labor and birth, and childbearing women now labor and give birth under epidural anesthesia instead of general anesthesia, the cultural assumption of the early 1900s remains intact in the 21st century in the US– the illogical idea that obstetrically-trained surgeons should control the entire maternity care system, be the primary providers for healthy childbearing women and that more and more medical and surgical interventions used earlier and more often is the very best way to ‘improve’ maternity care.
The obstetrical “winner-take-all” perspective also believes and publicly promotes the idea that midwifery care in general is a wrong-headed, substandard and a step-backwards. Likewise, any attempt to move childbirth services for healthy women out of an acute-care hospital setting (independent birth centers, home, etc) is so irresponsibly dangerous that it should be illegal.
Attempts in the 1950s to eliminate “knock’em-out, drag’em-out” obstetrical practices

Labor room nurse in 1910 with labor patient who has been giving scopolamine so she won’t remember bing in labor. The hood and the makeshift straight-jacket (sheet tied around her shoulders and around her back) was a standard way to reduce unwanted stimulation for room lights and the staff moving around in the patient’s room
Activists groups initially focused primarily on eliminating the use of Twilight Sleep drugs — repeatedly giving shots of narcotics and the hallucinogenic-amnesic drug scopolamine during labor. This was soon expanded to eliminating the routine use of general anesthesia, episiotomy, forceps and manual removal of placenta in healthy, low-risk women who did not need, want or benefit from a heavily-medicalized labor and birth.
By any standard, the efforts by birth activists were very successful in bringing attention to the general issue of childbirth practices and ultimately spurred a lot of interest in “awake and aware” childbirth. This was the extreme polar opposite of being semi-comatose during labor and unconscious during a surgically-conducted ‘delivery’, in a restricted “Hospital Personnal Only” L&D unit, where no family members were permitted under any circumstances.
For the mother-to-be, an important part of being awake was sharing the experience with her husband or close family member (her mom or sister), policy changes the would allow one’s husband and close friends or family members to be present during the labor and birth was a central goal.
This interest in the mother’s experience and participation in normal labor and birth gave rise the idea of ‘childbirth preparation’. Very popular books about this were written by Dr. Bradly (originator of “Husband-coached Childbirth”), the French obstetrician, Dr. Lamaze and others such as “The Birth Book” in 1972 by Raven Lang. All of these authors focused on the mother being unmedicated and the many advantages that provide for both mothers and babies.
When laboring mothers were allowed to be ‘awake and aware’, their babies did not suffer the deleterious effects of narcotic and general anesthesia. This provided an opportunity for the newborn baby to be given to its mother to hold briefly before being it was taken off to the newborn nursery to be monitored for the first 12 hours after delivery.
Multiple articles in women’s magazines and even the general-circulation magazine “Life” spread the revolutionary new idea that healthy mothers with normal pregnancies should be able allowed to be conscious during birth. This was followed by the idea of childbirth ‘education’ that would prepare unmedicated mothers to cope with labor pains and how to cooperate with the doctor while she was pushing her baby out. Some formal training materials and courses were developed by Lamaze, Husband-coached Childbirth and the International Childbirth Education Associations (ICEA).
In addition to this new interest in the how labor and birth were conducted, books like “The Womanly Art of Breastfeeding” that would be followed by groups that promoted breastfeeding (Le Lache League).
Publicity ~ two-edged sword that woke organized medicine’s 800-pound gorilla
Widespread and negative publicity about the harm and dislike of ‘standard’ obstetrical practices by many women of childbearing age got the full attention of the obstetrical profession. Unfortunately, this was NOT something that ultimately benefited healthy childbearing women or made real and long-lasting institutional changes, such as increasing care by midwives and family practice physicians (both in and out-of-hospital) or legitimized the options for physiological management of normal childbirths in OOH settings, such as independent birth centers and home birth services.
The reason was simple, and considering that we were dealing with an 800-pound gorilla that did NOT/ does not like to share, this should not be too much of a surprise. Many of the changes introduced by birth activists groups were simply co-opted by the obstetrical profession — cosmetic or insubstantial changes such as colored bedspreads or letting husbands or one’s mom into the labor room — took the wind out of the sails of activists as many childbearing women were fooled into thinking that things were “all different” now.
One of the most critical issues a decision by obstetricians, hospital administrators and anesthesiologists to create a new sub-speciality in anesthesia – obstetrical anesthesia. Beginning in the early 1980s, epidural anesthesia became increasingly available in for-profit hospitals who decided to hired anesthesiologists to staff their L&D 24-7, so they could adverse the availability of ‘on-demand’ epidurals as a way to get a jump on their competition.
This allowed laboring women to be “awake and aware” while still being confined to bed, and still giving birth while anesthetized, which in many cases an operative deliveries to overcome the mother’s innately anti-gravitational position (lying on her back) and her inability to push effectively because she was numb from the waist down and couldn’t tell what was happening in her body. As a result their babies needed to be extracted by their doctor with forceps or vacuum extraction.
Epidurals quickly and seamlessly replaced the administration of narcotics during labor and use of general anesthesia during delivery. This it to say that ubiquitous use of epidurals did more to eliminate the use of Twilight Sleep drugs than consumer groups, birth activists and childbirth education instructions. The routine use of epidurals also made it so much easier (at least from the physician’s perspective) to perform CSs, as the mother was already numb. All they had to do was roll the ICU-type labor bed into the OR.
Birth activists in contemporary times have been promoting physiologic childbirth practices as the standard of care for healthy women, working to stop the ever-escalating use of elective inductions and Cesarean surgery rates and hope to dramatically reverse the trend, and are trying to make sure that pregnant women understand their legal and ethical rights to self-determination – that is, say “no” to unwanted medicalization.
Doctors making birth safe vs. letting the normal biology keep it safe
It was obvious early on that educating the public about normal childbirth was a critical first step. It provided the most immediate opportunity to turn the public discourse around by 180-degrees. For the entire 20th century, doctors were seen as responsible for “making” childbirth safe by using an ever-lengthening list of medical and surgical interventions.
However, it turns out that Mother Nature is no fool. Whenever we try to fool Mother Nature, it disrupts the normal biology and introduces artificially-created “complications”. The smarter relationship with normal biology in healthy childbearing women is to “let” the inherent safety of its spontaneous physiology be our guide and standard.
For the last 100 years, the obstetrical profession has had many reasons for not wanting to normalize childbirth, but one of the biggest and most important is economics. Normal childbirth is legally categorized as a surgical procedure identified as “normal spontaneous vaginal delivery” (NSVD). At a practical level, this means obstetricians, who are specially trained surgeons, are only responsible for performing the surgical procedure of NSVD.
Unless there are serious complications, obstetricians bear no responsibility to provide the time-consuming supportive care needed by the pregnant woman during the many hours of her latent, 1st and 2nd stage labor, and the immediate care of the newly delivered mother and her neonate. Instead, hospital nurses are responsible for both the ‘pre-op’ phase (labor) and post-op phase (new mother/new baby).
In this rather Kafkaesque arrangement, nurses can’t legally “catch” babies except in an emergency, i.e. if the baby is born precipitously. When that happens everyone is upset and even angry with the labor patient’s nurse. As a former as L&D nurse, I know that labor room nurses get in a lot of trouble if they don’t call the doctor at just the ‘right’ time – not to soon and certain not too late!
Of the two possibilities, ‘too late’ is the unforgivable “opps”, as neither the hospital nor patient’s obstetrician can bill for the well paying surgical procedure of normal birth if the nurse ‘catches’ the baby. The patient’s obstetrician cannot bill for a surgical procedure that he or she did not officially “perform” (or at least be in the room). The hospital, as the nurse’s employer, can’t bill use the NSVD billing code to get reimbursed because the nurse is not licensed by the state to perform surgical procedures. This also applies if the mother accidently delivers unattended in the bed or bathroom.
The surgical reimbursement system described above helps us understand the basic economics of the obstetrical profession. To maximize their personal profit stream, OB-GYN surgeons, like all other types of surgeons, must have the freedom to move unencumbered from one operating room (or LDRP) to another, while never “wasting” their valuable surgeon’s time doing something for which they are not reimbursed at the rates paid for performing surgery. This is achieved by delegating all the care needed by their patients during labor and postpartum to hospital nurses, who are being paid a very modest (by comparison) salary or hour wage.
Remarks by two obstetricians who practiced nearly a hundred years apart reveals both the historical and contemporary nature of obstetrical economics. The first, published in 1922, is a quote from Dr. Ziegler, a well-known obstetrician of his day. He was describing the historical strategy of the obstetrical profession to eliminate the participation of midwives in childbirth and then divide the comprehensive care normally provided by midwives during all stages of labor, birth and postpartum by reapportioning these services unequally between the two professions of medicine and nursing.
Laboring ‘sitting’, which was both low paying and time-consuming, was assigned to hospital nurses, who worked 12 hour shifts in the 1920s. The high-paying photo-finish part was assumed by doctors, who were called in to catch the baby as described in the more formal terms of “performing” the surgical procedure of NSVD (15-to-45 minutes). As seen from the surgeon’s perspective, the bottom line was to maximize per unit/patient profit by minimizing per unit/patient time. This was to be achieved by having nurses do almost everything but catch the baby. In that regard, a very important part of the nurse’s job was to notify the doctors at the right time – not too early, which (as noted earlier) would waste his time, or too late, which would deprive him of his professional fee.
The doctor must be enabled to get his money from small fees received from a much larger number of patients cared for under time-saving and strength-conserving conditions; he must do his work at the minimum expense to himself, and he must not be asked to do any work for which he is not paid the stipulated fee. This means … the doctors must be relieved of all work that can be done by others —… nurses, social workers, and midwives.”
The nurses should be trained to do all the antepartum and postpartum work, from both the doctors’ and nurses’ standpoint, with the doctors always available as consultants when things go wrong; and the midwives should be trained to do the work of … “practical nurses,” acting as assistants to the regular nurses and … assistant-attendants upon women in labor — conducting the labor during the waiting period or until the doctor arrives, and assisting him during the delivery. [1922-A; Ziegler, MD, p. 412]
In this plan, the work of the doctors would be limited to the delivery of patients, to consult with the nurses, and the making of complete physical and obstetrical examinations … Under this arrangements the doctors would have to work together in a cooperative association with an equitable distribution of the work and earnings.” [1922-A; Dr. Ziegler, MD, p. 413]
The second quote comes from a Dr. J A Macer, contemporary obstetrician. It was published in 1992 in the American Journal of Obstetrics and Gynecology in an article about the future direction of the obstetrical profession, a direction that is consistent with the economic plan described by Dr. Ziegler 70 years earlier:
“It is no longer feasible for individual physicians who have invested 12 years in training at a cost of hundreds of thousands of dollars to dedicate extended periods to observing one normal woman in labor.” [Macer JA et al; Am J Obstet Gynecol 1992:166:1690-7].
Lowering the CS rate – What’s Missing?
Our current, Cesarean-centric maternity care system introduces unnecessary danger by using an emergency rescue operation as a business-as-usual daily routine. As a result, obstetricians have inadvertently become a prisoner of their own project. Without meaning to, the current system favors babies at the great expense of their mothers and other family members. It is bad for society for many obvious reasons.
For the lay pubic, it has institutionalized an irrational fear of childbirth and perpetuates ignorance of the actual normal biology. The wrong use of obstetrical practices is even bad the obstetrical profession itself, as they too are trapped by this same fear and ignorance, which prevents them from developing mastery in the very area that we would most expect and benefit – the principles and practices that lead to a safe and spontaneous normal birth.
What to do?
Let me start with an example from the “fast foods” vs. ‘”slow cooking” debate.
Over the last decade, we realized that a steady diet of ‘fast foods’ was detrimental to our health, and a growing appreciation of the benefits and critical role of cooked-at-home nutritious meals in the company of friends and family. According to public health officials, a third of Americans are either pre-diabetic or have already been diagnosed as a Type II diabetic. Apparently French fries are not a health food.
Nonetheless everyone gets in a rush from time to time. When that happens, we pull into the drive-thru of a fast-food restaurant and come out the other end with burger, fries and a coke, which we eat alone in our cars as we go on our way. As an occasional meal, this is not a problem, but as daily fare it is potentially deadly. We can be certain that the CEOs of giant fast-food franchises do not serve burgers and fries at their up-scale stockholder meetings.
But the issue of ‘fast food’ is not just nutritional. A lot of really smart people have realized that the ‘style’ of fast food preparation and consumption is detrimental to our social values in many ways. The sheer number of Americans with diabetes threatens to both overwhelm and bankrupt our healthcare system, as the inevitable complications of diabetes turns productive full-time employees into long-term unemployed hospital patients. But the even bigger issue is a ‘quality of life’ (i.e. lack of quality) problem for every American and children as yet unborn.
These and similar problems are forcing us to reconsider one of the most fundamental ideas of the industrialized revolution — that fast is so much better than slow, and that fast, faster, fastest is good, better, best. Unfortunately the one-speed setting of ‘fast’ turns out to be a problem in many other delicate areas of life — trying to set a speed record is not a trait we would appreciate in a lover. Relative to fast foods, the fact that we don’t cook for our self and our families any more is a social as well as an intergenerational ‘healthy life-style’ problem. Thankfully this has a wonderful solution called the “slow cooking” movement.
That bring me back full circle to our topic and our national obsession with speeding things up as much as possible. Obviously a scheduled CS is the fastest way to have a baby! But in our haste to get everything over with quickly, we are putting normal (physiologic) childbirth on the ‘endangered species’ list for normal biological functions.
Within the last year, several large businesses have noticed that their health insurance costs are much higher when employees have Cesarean surgery instead of a vaginal birth. The list of serious complications noted earlier is not just a nightmare for the childbearing family. Hemorrhage, blood transfusions, emergency hysterectomies, surgical wound infections, hospital-acquired sepsis, ICU admissions, re-hospitalization, treatment of secondary infertility, repeat CS are all extraordinarily expense for the patient’s employer. A few of these big companies have acted boldly by removing hospitals with high Cesarean rates from their ‘approved reimbursement’ list. This certainly has gotten the attention of more than a few hospital administrators.
It also has spurred a number of very smart people in the field of maternity care to hunt for safe and cost-effective ways to reduce our CS rate. One of these is the California Maternal Quality Care Collaborative (CMQMC), whose offices are on the Stanford Campus in the University’s medical school building. They published a 66-page document this year titled “Toolkit to Support Vaginal Birth and Reduce Primary Cesareans” and are engaged in outreach to obstetrical providers via frequent on-line webinars. The toolkit describes the problems associated with a high C-section rate and provide many useful suggestions for safely increasing the rate of vaginal birth within the hospital setting.
It was a huge undertaking and the staff of the CMQCC has done an extraordinary job. But this endeavor was privately funded by the obstetrical-hospital complex. Since midwives already have a high vaginal birth rate, the toolkit is specifically directed to the obstetrical profession. Some measure of what a steep hill this is to climb is a study published in the BJOG on different attitudes towards birth by obstetricians, family practice physicians and professional midwives.
After extensive surveys, the authors reported that obstetricians more strongly believed that women had the right to request a Cesarean section without any maternal-fetal indications and that epidurals early in labor were not associated with development of fetal malpositions. Most astonishing, a majority of obstetricians believed that increasing caesarean rates were a sign of improvement in obstetrics. Do maternity care provider groups have different attitudes towards birth? Reime B, Klein MC, Kelly A, Duxbury N, Saxell L, Liston R, Prompers FJ, Entjes RS, Wong V. BJOG. 2004 Dec;111(12):1388-93.
Given such a daunting list of restrains, the CMQCC document necessarily stopped short of stating the otherwise inescapable fact – the only thing that will safely reduce the CS rate and increase the rate of normal spontaneous vaginal birth is to fundamentally transform the American system of maternity care for healthy women. That means replacing the current obstetric-centric process as it applies to healthy women with a mother-baby-father friendly model that is a physiologically-based and primarily staffed by professional midwives.
Obviously this is not what the obstetrical profession wants to hear but the best — in fact, the only way — to reduce our over-the-moon Cesarean rate in the US is to apply the idea of slowing down to the care provided during labor and birth. For our purposes today, I’ll call this the “slow childbirth” movement, which would ultimately preserve the health and improve the experience of already healthy laboring women and their unborn-newborn babies, while saving the national healthcare budget a ton of money.
Transforming maternity care system for the 21st century
As “slow childbirth” model would begin by integrating the science-based principles of physiological management need to be with best advances in obstetrical medicine to create a single, evidence-based standard for all healthy women with normal pregnancies. In this model, obstetric interventions are reserved for those with complications or if requested by the mother. Such slowing-down also requires a trusting attitude toward normal biology and the use of time-tested strategies for supporting the physiology of normal labor. This includes patience-with-nature, maternal mobility and upright postures, use of non-drug pain relief (one-on-one care, touch relaxation, walking about, hot showers, warm deep-water tubs) and the right use of gravity during the pushing stage.
In the absence of complications it eliminating artificial time constraints and acknowledging the healthy woman’s right to choose the place of birth, the persons present in the room when she gives birth, and the positions that work best for her unless a bona fide medical emergency is occurring.
This can be seen as a drastic remedy, but historically, the ‘slow’ movement for normal childbirth practices was always the safer choice. What it says is particularly relevant when describing the “modern” practice (circa 1931) in which “many physicians to employ procedures which are calculated to hasten delivery”. Such a description could have come from today’s newspaper.
. . . that trained midwives surpass the record of physicians in normal deliveries has been ascribed to several factors. Chief among these is the fact that the circumstances of modern practice induce many physicians to employ procedures which are calculated to hasten delivery, but which sometimes result in harm to mother and child.
On her part, the midwife is not permitted to and does not employ such procedures. She waits patiently and lets nature take its course.”
White House Conference on Child Health and Protection. Committee on Prenatal and Maternal Care, 1931; testimony on the efficacy of midwifery care
Lets hear a round of applause for “She waits patiently and lets nature take its course.”
How did we get a system that is so out-of-kilter with the biological needs of healthy women, so expensive, w/ such a high CS rate?
That’s a $64,000 question, but when you list the facts, it seems so obvious. After 13 grueling years as a student in college, medical school and ob-gyn surgical residency, and owing a quarter million in student loans, why would we expect newly-minted obstetrical surgeons to take on the job of providing one-on-one bedside support to healthy women having a normal labor?
First off, it would be economic suicide. But even if obstetricians were compensated at the same hourly rate as gynecological surgeries and Cesarean deliveries, there still is a fundamental disconnect. As noted already, the physiological management of childbirth is not taught in medical schools or obstetrical residencies. Obstetricians are not trained or otherwise prepared to be responsible for laboring women, newly delivered mothers, newborns or helping new mothers breastfeed for the first time.
As a rule, obstetricians don’t want to “labor sit”. Being an obstetrician/gynecologist requires them to have the temperament of a surgeon. Successful ‘surgeon’ traits include decisiveness, quick action and taking charge. The traits that got them through 4 years obstetrical residency are the polar opposite of the supportive, time-consuming care required during a normal labor. What laboring women needs and want is someone she already know relatively well who is low–key and friendly and has the temperament to sit around patiently and cheerfully for endless hours, whispering encouragement and other sweet things in her ear about how she doing fine and she got what it takes, can ‘do it’. Sometimes acceding to Mother Nature time-table for a safe spontaneous birth takes 30 hours and whoever is ‘midwifing’ (the verb) the mother must be continuously present (except for occasional 1 1/2 hour naps) for the entire time. This would really drive a surgeon-obstetrician nuts.
The reticence and mismatch of obstetricians to personally support slow biological process of normal childbirth would not be an problem if the obstetrical profession just hired professional midwives to staff their hospital’s L&D unit. In that case, laboring women would be cared for midwives who are already trained and experienced in physiological management and accustomed to waiting patiently on Mother Nature. This and only this will drastically reduce the hospital’s CS rate. It would also take a huge burden off the shoulders of obstetricians. But a majority of obstetricians see this as a call to war and won’t even discuss such a commonsense solution to the high CS/low NSVD rate in their communities.
But regardless of the obstetrical profession’s opinion about the “slow childbirth” movement, there is an immutable bottom-line that will not go away. We must figure out why we are one of only 8 countries with a rising maternal mortality rate. I’ve stressed the virtues of “slow”, but the watchword is “pronto” when it comes to fixing this kind of problem.
Personally I believe that the best way to eliminate preventable maternal deaths, as well as eliminating unproductive expenses, is to lower our CS rate. In order to do that, retire the current system that was designed to medicalized healthy women with normal pregnancies. We must safely increase the rate of normal spontaneous birth by reducing the C-section rate without increasing the use of Pitocin, vacuum extraction or forceps.
No healthy women should ever be forced to choose between a physician-obstetrician and a midwife, or between hospital and home, in order to have a physiologically-managed normal labor and birth. Science-based physiologic childbirth practices must be available to all healthy childbearing women in all birth settings – home, hospital, or free-standing birth center – by all categories of birth attendants (physician-obstetricians and all professional midwives — LMs CPMs and CNMs).
Where do we start?
We have to raise the public’s awareness and understanding of these issues. This usually calls for a targeted and well-designed public education campaign. Sadly previous efforts to do this have been frequently rebuffed. Over the past half-century, a deep-set bias against normal childbirth causes most Americans to reject new information on this topic. For the most part, people think they already know all they need to know, which is to say that normal childbirth is “extremely dangerous”. This can be traced back to the early 1900s, when two distinct historical situations cemented the public opinion about childbirth as both dangerous and too complicated for a layperson to understand, therefore best left to doctors.
Our modern ability to educate and mobilize Americans in sufficient numbers to be politically effective has been negatively effected by two major historical forces. One is the position taken by the new American of obstetrics and gynecology between 1910 and yesterday, and the other is the American people over this same 100-plus span of time.
Historical situation #1 – How healthy women were turned into the patients of a surgical specialty and normal childbirth became a surgical procedure “performed” by obstetrically-trained surgeons ~ why such ‘ancient history’ still matters today
The two American professions of obstetrics (as part of a GPs practice) and gynecology (a surgical specialty) combined to form a brand new surgical discipline in the late 1890s. One of the new profession’s first official acts was to develop a plan for eliminating the legal practice of midwifery, while also promoting the routine hospitalization of healthy women under the care of obstetrically-trained doctors. Women were assured that the “modern” way to have a baby was in the hospital under the care of an MD.
By 1910, a small but steady stream of the very poor (often homeless) women and the very wealthy but healthy were going to hospitals to have their babies. The germ theory of infectious disease was common knowledge by this time, so the “bio-hazards” associated with caring for the ill and injured were generally understood by doctors and the lay public alike. The obstetrical profession was proud of to play their part of in ‘modern medical science’ and enthusiastically adopted antiseptic principles such as hand washing and the use of sterile gloves. Hospitals regularly cleaned floors and other surfaces with germicides and sterilized instruments and other equipment between patients. Kids were not allowed to visit, lest they contaminate the hospital with their colds and contagious childhood diseases.
But in spite of what we considered to be effective anti-bacterial strategies, the rate of fatalities among newly delivered women from childbirth fever still unacceptably high. This virulent form of septicemia (i.e. blood-poisoning) continued to be the 3rd most frequent cause of maternal deaths, and was especially a problem in hospitalized maternity patients. Unfortunately, it would be another three decades before medical science discovery antibiotics and longer still before they were available in the US (May 1945).
This was an awkward in-between era for obstetrics, a time that was post- germ theory but pre-antibiotics. Before the discovery of antibiotics, there was absolutely NO effective treatment for systemic sepsis. Everything depended on prevention, which wasn’t nearly as dependable as everyone hoped, since new mothers were still dying from supposedly ‘preventable’ infections.
Influential leaders in the field, including Dr. De Lee and Dr. J. Whitridge Williams (author of “Williams’ Obstetrics” textbook) concluded that the only thing they hadn’t tried yet was to “Listerize” normal childbirth birth. This extraordinarily complicated protocol meant adopting strategies invented by Dr. Joseph Lister (of “Listerine” fame and remembered as the “Father of Modern Surgery”) for conducting surgery under a “strict sterile technique”. This was the only way to prevent, or at least reduce, the likelihood that a surgical patient would die afterwards from a post-operative infection. At that time, from 30% to 100% of post-op patients succumbed to “hospital fever”, depending on what part of the body was involved.
The model adopted by De Lee and Williams required the usual 5-minute scrubbing of hands and wearing of a sterile gown, cap, mask and gloves. The OR-type delivery room was off-limits to all non-essential personnel, and of course husbands or other family members. It also required the mother to be in the delivery room for the entire 2nd or pushing stage of labor. After being moved to the narrow delivery table, her wrists were put in leather restraints, her legs slipped into sterile thigh-high cotton stockings and strapped into the stirrups. Then her perineum was scrubbed with an antiseptic soap and sprayed with iodine. Finally she was covered from head to toe in sterile sheets, and then put to sleep under general anesthesia.
Based on the Lister’s principles of asepsis, these sterility protocols were considered essential. General anesthesia was also necessary to be sure the mother didn’t contaminate the sterile field. Dr. Delee was all too familiar with how women in labor who were not anesthetized kept moving around; they talked and coughed and touched things, sometimes (god forbid!) even grabbing the surgeon’s sterile gloved hands.
As soon as the mother-to-be was unconscious, the doctor cut a “generous” episiotomy, used forceps to lift the baby out, manually removed the placenta and sutured the perineal incision. Being quick was important. Doctors knew they had to limit the unborn baby’s exposure to the potentially deadly effects of chloroform before its birth, and afterwards they had to guard the mother against respiratory depression or liver failure caused by prolonged breathing anesthetics gases. This series of surgical procedures in quick succession reduced the delivery time for first-time mothers from 2 or even 3 hours to less than 30 minutes. In their minds, this made childbirth so much safer.
Obstetrical physicians were concerned about maintaining the highest level of sterility to prevent for two problems. The first was reducing in the likelihood of contagion and deaths from puerperal sepsis. The second was not medical but a legal-social issue. If, despite the doctor’s best efforts, the mother should develop a fatal infection afterwards, the doctor might needed to defend himself against claims by the family that he was to blame. Considering the frequency of maternal deaths from infection, both of the doctor’s fears were quite realistic.
However, Dr. De Lee thought it was unfair for the public, which also knew about germs and contagion, to automatically blame the doctor when their wife or daughter died from childbed fever. He was quick to point out that the husband was the more likely culprit, intimating that the husband had sex with prostitutes or deviate sexual practices that introduced deadly bacteria in his wife’s vagina. Doctors needed to be able to defend themselves from these recriminations and the possibility that the family might try to ruin his reputation by publicly claiming his sterile technique was faulty and he introduced harmful bacteria during the birth.
Just as doing a CS today is the modern obstetrician’s way of demonstrating that he or she has done “everything humanely possible” to prevent an ‘adverse event’, so using a flawless sterile technique meant the early 1900s obstetrician could assure the bereaved family that he was not to be blamed for any ‘unfortunate’ outcome caused by microscopic bacteria.
This is the history of how normal childbirth became a surgical procedure. Normal birth has retained this legal designation for the last 100 years, as doctors are still reimbursed under the surgical billing code “NSVD” (normal spontaneous vaginal delivery).
Situation #2
In spite of the bio-hazards of hospitalizing healthy women and their babies during the American obstetrical profession had embarked on a well-financed PR campaign that so far has lasted more than a 100 years. It has consistently stigmatized and misrepresented of the idea of a medically-undisturbed normal birth as irresponsibly dangerous, while portraying the pre-emptive use of multiple medical and surgical interventions as an inherently harmless and beneficent.
Fear-based assumption by the lay public and the medical profession sincerely believed that a highly medicalized and interventive system of obstetrical care was needed to make childbirth ‘safe’. This is the origin of the contemporary policies and protocols that treat every laboring woman as a potential medical emergency. Healthy women with normal pregnancies are routinely tethered to their beds with IVs tubing, electronic monitor leads, automatic blood-pressure cuffs and other medical devices in an obstetrical Intensive Care Unit (ICU), where they are subjected to an average of 7 significant medical and surgical procedures.
So far, this communal fear of childbirth has locked allt his in place and effectively block 50-plus years of attempts to change the system of care provided to healthy childbearing women, from an obstetrically-interventive model to the physiologically-based, non-medical management of normal labor and birth in healthy women, with access to comprehensive obstetrical services as needed or requested by the childbearing woman.
Our culture’s fear-based relationship with normal childbirth has justified a highly medicalized form of care in which interventions developed to treat so there is no need to make any changes or pay any further attention to the topic.
As a result, these is no public dialogue about the many unintended consequences or ‘side-effects’ of our expensive, highly-medicalized obstetrical model.
Additional aspects of this history:
- Accurate knowledge about professional midwifery.
Very recent media presentation of interest on this general topic:
http://money.cnn.com/this-is-birth-with-lisa-ling/
Original file name “CALM_KReckdahl_addendum#2_Sept 2016”