Double-click the graphic to enlarge & read.
Click here to download a PDF of it
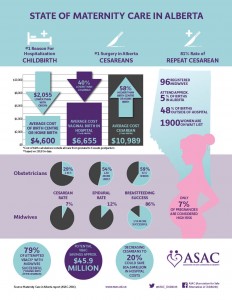
In the Canadian province of Alberta:
- The single most frequent reason for hospitalization is childbirth.
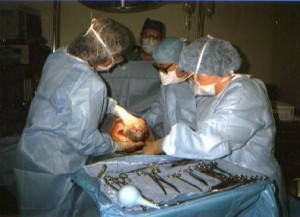
- Cesarean is the most frequent type of surgery.
- Alberta’s repeat C-section rate is 81% (equals a VBAC rate of 19%).
In Alberta, the average cost of maternity care as provided by professional midwives is $2,000 less than obstetrical care for a normal spontaneous birth {$4,600 vs. $6,655}.
Alberta’s average costs and intervention rates for both obstetricians and midwives were:
- Cesarean rate was 29% for obstetrical care, but only 7% for physiological management provided by midwives
- Cost of Cesarean section was approximately $11,000 ($10,998)
- Epidural rate was 54% for obstetrics, but only 12% for midwifery providers
Successful VBAC rate for midwifery care was 79% — a potential VBAC saving of $45.9 million since 2009, which is when professional midwifery services first became publicly funded in the province
According to the report, reducing the C-section rate to 20% (down from 29%), would potentially save $14.5 million annually in hospital costs.
The report also notes that only 7% of Alberta’s childbearing population has “high risk” pregnancies. In other words, 93% of the pregnant women in this Canadian province are healthy and having normal pregnancies.
Based on such data, Albert’s healthy childbearing population could have as easily, and much more economically, given birth in out-of-hospital birth centers staffed by midwives and family practice physicians.
Comparison of obstetrical cost in the US:
The same maternity-centric use of hospitals and surgical services is also true in the United States. 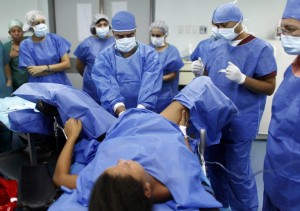
Childbirth is our most frequent reason for hospitalization, cesarean surgery our most frequently performed surgery, and our repeat CS rate is even higher — 91% (i.e. our national VBAC rate is only 9%).
Standard obstetrical care for a normal vaginal birth US costs $12,000 for families living in the mid-west and south, and $20,000-$30,000 on both coasts (highest in large urban areas such as NYC, Chicago, Denver, L.A. and the San Francisco Bay area). The average C-section rate in US is 33%; a few hospitals (ex. Kaiser HMOs) have a rate as low as 15%, while at the other end, there are hospitals with a 70% rate.
The percentage of high-risk pregnancies in the US is estimated to be between 10 and 30%, depending on the criteria used (for example, whether maternal obesity does or does not automatically put the pregnant woman in “high-risk” category). But even if you took the most conservative US number, 70% of childbearing women in America would be found healthy and having normal (term) pregnancies.
If we were we to identify physiologic childbirth (instead of current medicalized birth practices) as the appropriate standard of care for healthy women, and policies that provided pregnancy and childbirth care by professional midwives and family practice physicians, we would see these same benefits as in Alberta Canada — much lower cost, fewer interventions, and iatrogenic complications, greatly reduced CS rates, higher levels of successful breastfeeding and increased patient satisfaction.
Applying this data to maternity care for healthy women in the US
If the US really wanted to lower health care costs and make high-quality maternity care available to all healthy women with normal pregnancies (70 to 90%), we would adopt a physiologically-based care standard of care as provided by professional midwives and family practice physicians in hospitals and free-standing birth centers (OOH).
This would need to be accompanied by new, non-surgical billing code for normal childbirth (for the last 100 years, normal birth has been billed as a surgical procedure). This is the only way that midwives and physicians can be fairly compensated for their time, instead of our current system that only reimburses them for performing medical interventions and surgical procedures. This backward system of incentives and economic compensation fits the definition of “insane”, and should be immediately scrapped.
To successfully provide physiologically-based childbirth practices requires the full-time presence of the primary birth attendant (MD or midwife) throughout active labor, the birth and care of the new mother and new baby for the first hour or so after the birth. As established by the Canadian report, this form of one-on-one professional care reduces the rate of medical and surgical interventions four-fold — that is, statistically significant level — thus also reducing the cost of maternity care for healthy women without any reduction in safety and other aspects of quality care.
Clearly, the full-time presence of professional birth attendants trained and experienced in physiologic childbirth management prevents the need, and associated risks and additional expense, of otherwise unnecessary medical interventions and surgical procedures. However, our current system does not compensate professional birth attendants for their professional time; this stumbling block can be easily removed by creating a new and non-surgical billing code that combines the care received during all phases of the intrapartum — labor, birth and new mother-new baby period.
Bottom line, we have to speak up and keep moving the action forward until we have replaced this historical craziness with the “best practice” of physiologic care for healthy women with normal pregnancies that neither need or want routine medical and surgical intervention. That also means fairly compensating our professional maternity care providers for their time-consuming efforts to keep our new mothers and babies safe and our taxpayers happy.
 Pass it on!
Pass it on!
URL for the info graphic:
https://d3n8a8pro7vhmx.cloudfront.net/asac/pages/75/attachments/original/1481648616/Maternity_Care_Report-Infographic.pdf?1481648616