The truth about ineffective, harmful or economically exploitive obstetrical practices as report by obstetricians
 Excerpts from published sources
Excerpts from published sources
Maternal-Fetal conflict vs Maternal-doctor conflicts
Oberman 2000: So-called maternal-doctor conflicts” in which obstetricians, based on their own opinion, routinely perceives a conflict about what best serves the interest of the fetus, believing that doctors have the right to override the woman’s autonomy.
In the words of a law review analysis:
” … these are not maternal-fetal conflicts at all, but rather maternal-doctor conflicts. The construction of these conflicts as “maternal-fetal” . . . begins when doctors project their own estimations of the optimal course of action onto their pregnant patients.
When a pregnant woman resists medical advice, the doctor often invests the fetus with interests and rights that directly coincide with his own personal treatment preferences. The pregnant woman’s interests are then rendered in direct opposition to those attributed by the doctor to her fetus. Hence, the “maternal-fetal conflict.”
Finally, the doctor steps in as a seemingly neutral arbitrator who is well situated to settle this “conflict.” But, as it is the doctor who identifies the course of action deemed to be “in the fetus’s best interests,” the doctor is, by definition, not neutral. . . . the doctor becomes just another party to these conflicts—one who always tips the balance 2:1 against the pregnant woman.”
The belief that pregnancy and childbirth are inherently difficult and dangerous
 For the last 100-plus years, the obstetrical profession has assumed by that pregnancy and childbirth are inherently difficult and dangerous processes. In the early 1900s OBs defined pregnancy as: “A nine month disease that requires a surgical cure”.
For the last 100-plus years, the obstetrical profession has assumed by that pregnancy and childbirth are inherently difficult and dangerous processes. In the early 1900s OBs defined pregnancy as: “A nine month disease that requires a surgical cure”.
As a result, the majority of obstetricians and hospital obstetrical units distrust the normal biology of childbirth and reject physiologically-based as substandard at best, if not outright negligent. Instead the profession believes that all laboring women requires intensive monitoring, and aggressive intervention at all times.
This includes the ‘pre-emptive strike” of routine induction, in which perfectly healthy women with normal low-risk pregnancies are scheduled to be induced the week before their due date (i.e. at 39 wks)
“Labour is one of the shortest yet most hazardous journeys humans take during their lifetime” (Carlin 2006).
“Human reproduction is a wasteful process. There is little we as obstetric care providers can do about adverse events that occur in early pregnancy, such as failed implantation, recurrent miscarriage, cervical insufficiency, or preterm birth. But we can minimize injury and loss at the end of pregnancy.
Thirty-nine weeks and out! Saved by birth!” (D’Souza 2017).
- “I always tell people that an easy C-section is better than a hard vaginal delivery” (Mackenzie 2016).
Economic Incentives:
“NPR’s Shankar Vedantam description of the economic motives for obstetrical interventions:
‘Obstetricians perform more cesarean sections when there are financial incentives to do so,’ citing a study conducted by the National Bureau of Economic Research (NBER), which analyzed the links between ‘economic incentives and medical decision-making during childbirth’” (Wesley 2016).
Off-label use of Cytotec, a 27 cent ‘magic pill’ (cash cow!) that makes scheduled elective inductions profitable for hospitals
“The best part about it is that you can block-schedule your nurses so that you have enough on hand. . .
[I]f we start our inductions at 7 a.m., we know that we’re going to have X number of patients in labor being admitted by 4 p.m. That’s helped our hospital tremendously,
. . . [Cytotec is] a great agent. It works very, very efficiently. . . . And it’s ungodly inexpensive: 27 cents per tablet” (Jancin 2004).
Epidurals: Making hospital L&D units into a lucrative, assembly-line process
“While there may be problems with high epidural usage, in the presence of our nursing shortages and economic or business considerations, having a woman in bed, attached to an intravenous line and continuous electronic fetal monitor and in receipt of an epidural may be the only realistic way to go” (Leeman 2003).
Defensive Medicine:
“Increasingly, these adverse events during trial of labor have led to malpractice suits. These developments . . . illustrate the need to reevaluate VBAC recommendations” (ACOG 1999).
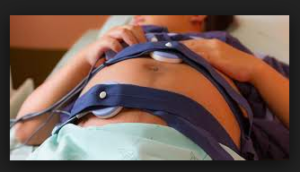 “The minute you see a deceleration on the heart monitor, you say maybe it’s fetal distress, better to do a cesarean. . . . A lot of that is driven by fear of liability” (Block 2007).
“The minute you see a deceleration on the heart monitor, you say maybe it’s fetal distress, better to do a cesarean. . . . A lot of that is driven by fear of liability” (Block 2007).
“. . . if there are any adverse outcomes, well that’s—you know—it’s all the obstetrician’s fault, so I tend to do inductions very easily” (Nippita 2017).
Hierarchical social structure of many hospitals:
“There was a wide discrepancy between current evidence/standards/guidelines and what nurses indicated would occur in actual clinical practice. . . . Open-ended responses revealed hierarchy, fear of and intimidation by physician colleagues, and lack of administrative support when conflict occurs as primary barriers to effective communication and perinatal teamwork” (Simpson 2009).
Convenience:
 “It’s almost like . . . [some nurses] think, ‘Just get an epidural because I’m not here to babysit you’” (Carlton 2009).
“It’s almost like . . . [some nurses] think, ‘Just get an epidural because I’m not here to babysit you’” (Carlton 2009).
“‘Scheduling an induction can make everyone’s life easier,’ [Dr. Leveno] said. . . . ‘I am not capable of constantly doing my best work in the middle of the night’” (Villarosa 2002).
“There is a convenience piece of [why obstetricians perform cesareans],” [Dr.] Rosenstein said.
“It is difficult to ask physicians to stay up all night and be patient with a laboring woman when they have to go to work the next day and see a full day’s worth of clinic patients or if they have to be in the operating room doing another type of surgery” (Halstead 2015).

