Editor’s Note:
 To makes these essays easier to read, I divided the longer ones into parts A, B, C & sometimes D. There are a total 13 posts. At the very end of the Mayday series, I provided links to a series of 8 scientific references and science-based editorials used in writing factual account.
To makes these essays easier to read, I divided the longer ones into parts A, B, C & sometimes D. There are a total 13 posts. At the very end of the Mayday series, I provided links to a series of 8 scientific references and science-based editorials used in writing factual account.
Easy way to share this link: https://tinyurl.com/y5ojmvue
19 minute read
 Chapter 1-A
Chapter 1-A
Calling all Americans:
We need to fix a simple problem that wastes many millions of our precious healthcare dollars every year by routinely using an ineffective technology that is very expensive (billed as much as $400 an hour) and results in preventable maternal deaths from complications associated with the increase in unnecessary Cesarean surgeries that accompanies the use of this obstetrical technology.
These needless tragedies for childbearing women and their families are a direct result of routinely using this ineffective and risky technology on healthy women with normal low-risk pregnancies whose unborn babies do not need or benefit from it.
Electronic fetal monitoring (EFM) was originally developed in the late 1960s for high-risk pregnancies. When used on laboring women with very complicated circumstances, EFM is helpful and in some cases can be life-saving. However, when EFM is routinely used during the labors of healthy women with normal pregnancies, it not only does not provide any benefit to either mother or baby, but does introduce potential and actual harm that especially affects the mother-to-be.
For the last 50 years, the manufacturers of EFM have promoted their product as an exciting new technology that can prevent cerebral palsy (CP) and newborn neurological disorders by providing an early warning system. Use of continuous EFM was purported to notify the OB staff immediately when a the unborn baby was becoming distressed. This in turn allowed the patient’s obstetrician to immediately do an Cesarean section. Virtually everyone agreed that “early” C-sections reliably prevented development of CP and other type of labor-related neonatal brain damage.
These same EFM manufacturers also mentioned to obstetricians and hospital administrators that the universal use of continuous EFM on all laboring women would reduce, if not outright eliminate, malpractice suits brought by the parents whose baby turned out not to be “perfect”. This was seen as a major ‘win-win’ miracle for both the obstetrical profession and childbearing public.
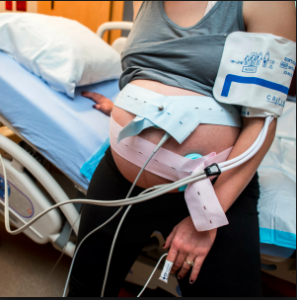
What a very “modern” but decidedly unnatural labor looks like!
But when EFM is applied to healthy women with low-risk pregnancies, it does not do what its proponents claimed, since the routine use of EFM does not reduce rates of CP, permanent neurological disabilities or perinatal morbidity and mortality.
What EFM does do, and does very well, is to immobilize the laboring woman the minute she walks into her labor room, as finds herself immediately tethered to her hospital bed by the EFM’s belts and cables.
This means she is unable to walk or move around, which are the classic non-drug coping strategies used for thousands of years by millions of healthy laboring women to help them tolerate the normally painful labor contractions — a vital heritage denied to us as “modern” women hooked up to electronic monitoring machines.
Equally important, having the labor woman be upright and mobile, walking and moving around freely and changing positions frequently, is Mother Nature’s way to keep labor progressing naturally without having to resort to potentially dangerous drugs like Pitocin to artificially speed up the labor. Unfortunately, the universal use of EFM denies access to these historical, time-tested coping strategies. Instead the mother-to-be lies in her hospital bed or stands leaning against it, while hooked to one or more machines.
For many laboring women, getting hooked up to continuous EFM is the beginning of a cascade of increasingly invasive obstetrical interventions that often end in an unplanned Cesarean section at a rate (31%) that is orders-of-magnitude higher than the legitimate use of Cesarean (5-10%) as a rescue operation appropriately used when the mother or unborn baby are in trouble.
Slip Twix Cup and Lip: When Words and Facts don’t Match
For half a century, EFM has been promoted as the only science-based method for preventing labor-related cases of cerebral palsy and similar newborn neurological pathologies. Unfortunately, the scientific evidence does NOT support this claim, as proven in study after study after study, beginning with the very first randomized control trial of EFM (Haverkamp, 1975). These studies compared the perinatal outcomes for two different methods or ‘arms’ of the study that monitored the well-being of unborn babies during the many long hours of labor.
 These randomized trials and studies included a “control” group in addition to the new and experimental methods of EFM. Then they compared the use of the traditional fetal monitoring method called “auscultation” to the new electronic monitoring device.
These randomized trials and studies included a “control” group in addition to the new and experimental methods of EFM. Then they compared the use of the traditional fetal monitoring method called “auscultation” to the new electronic monitoring device.
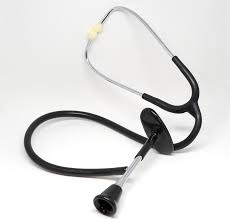
Auscultation, which means to listen and is pronounced “aws-cul-ta-tion”, uses a special stethoscope called a fetoscope (now days a hand-held electronic Doppler). The protocol for auscultation require that L&D nurses or midwives regularly listen to the rate and rhythm of the fetal heartbeat. The schedule for listening increases in frequently as the labor progresses towards birth. This data is recorded on the mother’s chart.
 Contemporary practice of Auscultation, circa 2020
Contemporary practice of Auscultation, circa 2020
Now days a hand-held ultrasound Doppler is used to listen (i.e. auscultate) fetal heart tones. To get the full benefit from auscultation requires one-on-one care by L&D nurses, midwives or obstetrically-trained physicians. Throughout the active stage of labor and birth, at least one of the trained staff should be in the room with the laboring mother at least 90% of the time.
Not only do these nurses and midwives count and record the baseline rate of the fetal heartbeat (normally at term btw 110 and 150 bpm), but also listen for accelerations, indications of “normal variability” (or note its absence as that can indicate a problem). They are also listening to be sure the baby’s heart rate is not having decelerations (a prolonged drop below baseline), which also can indicate an abnormality unless mother is in the pushing stage and the recovery to normal is fairly quick and consistent.
The EFM Arm of the study
The second or ‘experimental’ group used an electronic device attached by two belts that encircled the mother’s abdomen. One of the two transducers picked up the FHR and the other one was set to record the presence (or absence) and length of any uterine contractions. This information was electronically recorded and continuously printed out the fetal heart rate on graph paper throughout the entire labor.
This automated process did not/does not require the presence of hospital staff except to reposition the data-recording belts on the mother’s abdomen whenever the signal was lost. During the 1st three decades of EFM use, the laboring woman was required to lie still in the same position in order to get a good EFM tracing. Despite these efforts, the signal was lost so frequently that repositioning the monitor belts became the L&D nurse’s main and most frequent interaction with the laboring woman.
Unfortunately, when this elaborate, expensive, confining, and uncomfortable electronic process was used on healthy childbearing women with normal or ‘low-risk’ pregnancies, EFM could not and did not deliver on its many promises for guaranteeing the ‘perfect’ baby each and every time. What c-EFM did do is drive the primary Cesarean rate through the roof without any statistically significant improvement in perinatal outcomes for babies, and sadly, also increasing the maternal mortality rate.
Decades of studies find a significant increase in Cesareans & maternal deaths, but no decrease in CP or perinatal morbidity or mortality
For each of the last five decades, the scientific literature has come to the same conclusion again and again about the efficacy and safety of continuous EFM: When used on healthy childbearing women with normal low risk pregnancies, continuous EFM has no benefit to either mother or baby. A clear example of this scientific consensus was published in 2011 in a professional OB-GYN journal. It’s obstetrician-author began by explaining that:
“Despite the widespread use of EFM, there has been no decrease in cerebral palsy.
… meta-analysis of randomized control trials has shown that EFM has no effect in perinatal mortality or pediatric neurologic morbidity.2
However, EFM is associated with an increase in the rate of operative vaginal and cesarean deliveries.1”
Although intermittent fetal auscultation may be a theoretical option in low-risk patients, nursing staffing limitations makes this impractical … ”
Fetal Heart Rate Monitoring Update; The Female Patient, April 2011
Editorial comment: The last line acknowledges the effectiveness of auscultation for low-risk women, but claims that the staff limitations (i.e. additional staff to provide the necessary one-on-one nursing/midwifery care) makes auscultation “impractical”. This is code for “costs more” and tell us that is much cheaper for the hospital to hire a few nurses to sit at desks in the hallway and monitor banks of EFM computer screens piped in from the labor rooms rather than hiring L&D nurses to provide direct nursing care to the each of the women in labor.
As noted earlier, this is a false equivalency, as central monitoring is associated with an even higher C-section rate than bedside EFM.
The routine use of EFM over the last 5 decades has not reduced the CP rate by a even teeny tiny 1/10th of 1 percent — zip, zero, zilch, nada!
All EFM does for women with low-risk pregnancies is to sky-rocket the C-section rate.
NOTE: The second most frequent diagnosis for doing a C-section on a first-time mother is “non-reassuring fetal heart rate” as defined by the EFM strip.
In low-risk pregnancies, EFM is an iatrogenic intervention (i.e. a detrimental form of medical care). Its routine use is associated with a significant increase in Cesarean surgeries that in turn increases maternal morbidity (serious complications) and mortality (death) due to complications during and after Cesarean surgery and all future pregnancies. This also includes an increase in unexpected fetal demise/stillbirth in post-cesarean pregnancies due to placental abnormalities subsequent to previous Cesarean surgery.
For those who are still unconvinced, I offer the finding of the 2003 ACOG Task Force on Neonatal Encephalopathy and Cerebral Palsy published in a document titled “Neonatal Encephalopathy and Cerebral Palsy: Defining the Pathogenesis and Pathophysiology”
This ACOG report concluded that:
“… the majority of newborn brain injury does not occur during labor and delivery. Instead, most instances of neonatal encephalopathy and cerebral palsy are attributed to events that occur prior to the onset of labor.”
Link to the first of several studies and other publications cited or used as references in this series of posts on the use of electronic fetal monitoring on healthy women with low-risk pregnancies. The consequences for childbearing families are substantial, and in some cases, tragic.
After you click the link to this first reference, you can read this post and then sequentially follow the link at the bottom of each posts in order to load each of 7 published studies, articles or abstracts.
In addition the human cost is the unproductive economic expense to society. The universal use of EFM drives up the cost of hospital-based childbirth services as well as the rate of Cesarean surgeries. These expenses generated by these often ineffective or unnecessary procedures or costly complications are either billed to private insurance companies (running up everyone else’s premiums) or to the Medicaid program. The federal government reimburses hospitals for 49% of all births in the US, thus creating an additional tax burden for the rest of us.
The unnecessary and potentially harmful use of EFM satisfies the criteria for a genuine public health crisis!

