1C: Historical and legal background of the problem, more excerpts from EFM research
The obstetrical profession’s relationship with EFM as the universal standard of care in the US is like looking under the lamp post for keys that you lost on the far side of the street. The reason you are looking on this side is because the the light is better, not because you can expect to find your keys there.

The seductive but false idea that continuous use of EFM on every laboring woman will prevent cerebral palsy and other forms of brain damage in newborns keeps the obstetrical profession from looking in the right place — the 50 or more peer-reviewed studies published in professional medical journals that have unequivocally confirmed that the routine use of EFM for healthy women with normal pregnancies provides no benefit to either mother or baby, while unnecessarily risking the mother’s life due to the significantly increased rate of C-sections and the higher maternal death rate following a Cesarean delivery.
The Best of Intentions, a disappointing reality
Historically and in contemporary times, some apparently normal fetuses of healthy mothers after a perfectly healthy pregnancy are born with permanent mental and/or physical disabilities for inexplicable reasons.
For families that suffered a birth-related tragedy such as cerebral palsy, there is a high likelihood that they will sue hospital and all the doctors and nurses involved in any way with the labor or birth. This compounds a personal tragedy into a legal nightmare for the obstetrician and other professionals that provide care to them.
It’s totally reasonable that obstetricians would want to permanently prevent these tragedies by using continuous EFM for all laboring women. Continuous EFM, combined with expedited cesarean delivery whenever the monitor tracing indicated even a small problem, was seen by the obstetrical community as the long-awaited and logical answer to their prayers.
When the electronic technology of fetal monitors first became available, obstetricians all across America believed they found the “final solution” to an ancient and heartbreaking problem of babies born after a ‘normal’ birth who had some kind unexplained brain damage.
So there was (and is) nothing wrong with hospitals and obstetricians hoping that continuous electronic monitoring of all laboring women would eliminate both the personal tragedy and the malpractice risk to the obstetrician.
The idea that c-EFM & Cesareans would eliminate CP while protecting obstetricians from malpractice suits was enormously seductive. But unfortunately, it turned out to be wrong when EFM used on the 70-85% of healthy women with low- and moderate-risk pregnancies.
The problem for society is not a fight against the hopes and dreams of the obstetrical profession, but to look to the scientific evidence — what is says, or in this case, what it does NOT say. Since the very first study of electronic fetal monitoring in 1975, the research on its continuous use on low and moderate-risk mothers has repeatedly found that EFM by itself and EFM when combined with an increased rate of Cesarean delivery based on a “non-reassuring” EFM tracing did not make any statistically significant difference in perinatal outcomes — no reduced rate of perinatal deaths, cerebral palsy or encephalopathies.
The only cohort for which the benefits outweighed the risks was in the very highest risk pregnancies.
The right use of EFM: High-risk pregnancies
The one and ONLY area that c-EFM outperforms auscultation(regularly-scheduled listening with a fetoscope or hand-held doppler) is using EFM to monitor the labors of pregnant women with extremely high-risk pregnancies. However, this is only 15% of total labors. Women with low-risk pregnancies are the huge majority of all labor patients; 70% to 85%.
If the obstetrical profession had limited its routine use of c-EFM to the demographic that actually needed and benefited from it — extremely high-risk labors — I wouldn’t be writing about this discordant obstetrical practice and you, the reader, wouldn’t be reading about an expensive medical misadventure directly associated with increased levels of iatrogenic mortality and morbidity.
The real but never acknowledges tragedy of focusing on universal EFM as the ‘answer’ to preventing CP and other newborn neurological disabilities is that our society cannot turn its considerable talents — brain-power and the use of other strategies, such as statistical analysis and information from other forms of technology — to figure out the REAL origin of cerebral palsy and associated types of brain damage in newborns.
The 2003 ACOG Task Force on on Neonatal Encephalopathy & Cerebral Palsy (additional excerpts below) stated that the introduction of EFM made absolutely no change in the incidence of cerebral palsy, that the majority of newborn brain injury does not occur during labor and most instances of cerebral palsy and similar problems are attributed to events that occur prior to the onset of labor.
The obstetrical profession’s relationship with EFM as the universal standard in the US is like looking under the lamp post for the keys you lost on the far side of the street because the light is better on this side. It keeps us from looking in the right places.
Another ‘mis-direct’ — claims by EFM promoters that it is “Buckle-up for Safety” device
Manufactures of this expensive technology spend a great deal of time and money marketing the almost magical abilities of EFM. It’s described as such an essential safety device that it equate to buckling one’s safety belt each time we get in cars.
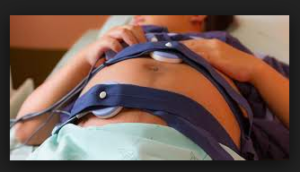
It shouldn’t surprise us that hospitals and the obstetrical profession treat c-EFM as the equivalent of the laboring woman wearing her seatbelt during labor. The hospital staff, the family and the obstetrician all act as if the two electronic cords circling the mother’s abdomen and plugged in to a computer console at her bedside has a magical ability to keep her baby safe through out the dangerous journey of labor and birth. The only thing that makes everyone in the room feel even safer — the “belt and suspenders” of obstetrics — is to put an oxygen mask on the mother so she is breathing pure oxygen.
These intervention are put in the same category of essential safety device as putting the newborn in an infant car seat for the trip home from the hospital.
Nonetheless, the facts are indisputable and give rise to an exactly opposite conclusion: The current system treats all healthy women with normal pregnancies as if they were high-risk. More to the point, it does this without improving outcomes for babies and while increasing medically-unnecessary surgical deliveries, and its many complications, including increased maternal mortality and morbidity.
For example, a paper titled “Heart Rate Monitoring Update” [The Female Patient, April 2011] makes this crystal clear. It begins by saying:
“Intrapartum fetal heart rate monitoring is the most common obstetric procedure performed in the United States” {1}
The author immediately admits that:
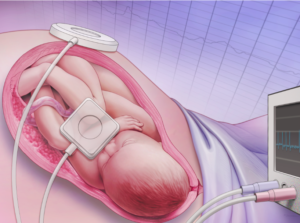
“Despite the widespread use of EFM, there has been no decrease in cerebral palsy. … a meta-analysis of randomized control trials has shown that EFM has no effect in perinatal mortality or pediatric neurologic morbidity.2
However, EFM is associated with an increase in the rate of operative vaginal and cesarean deliveries.1”
Although intermittent fetal auscultation {IA} may be a theoretical option in low-risk patients, nursing staffing limitations make this impractical … ”
A 2006 meta-analysis aggregated the data from randomized controlled trials done during the 1980s and 1990s and found no change in perinatal mortality or cerebral palsy rate when electronic fetal monitoring was used during labor.
It also identified a decided increase in Cesarean section rates and operative deliveries. It’s only positive finding was a small reduction in neonatal seizures, but this did NOT seem to make an overall difference in infant well being.
- Another recent study noted that the ability of continuous EFM to detect potential cases of cerebral palsy during labor is only 0.2%
This is not because the electronic circuitry of the equipment is flawed, but because the premise is incorrect – cerebral palsy can neither be reliably detected nor prevented based on the routine use of c-EFM during labor of healthy women with normal pregnancies.
The reason is simple enough:
- Only about 8% of neurological complications in newborns have any possible association with events of labor or birth
- Of that small percentage, intermittent auscultation (a simpler and non-continuous form of fetal monitoring known as IA) would have either picked up or missed the very same data but without introducing the added expense and all the other potential complications of c-EFM
- When c-EFM is routinely used on low and moderate risk populations with normal pregnancies, it introduces unnatural and unnecessary risks that include a substantial increase in episiotomy, forceps delivery, vacuum extraction, Cesarean surgery, and maternal mortality.
A report in the September 15, 2003 edition of Ob.Gyn.News stated:
- “The increasing cesarean delivery rate that occurred in conjunction with fetal monitoring has not been shown to be associated with any reduction in the CP rate…
- … Only 0.19% of all those in the study [diagnosed with CP] had a non-reassuring fetal heart rate pattern…..
- If used for identifying CP risk, a non-reassuring heart rate pattern would have had a 99.8% false positive rate N.Engl. J. Med 334[10:613-19, 1996
- Evidence leads us to believe that maternal infections during pregnancy might play an important role in [CP] development . . . and that in most cases the condition cannot be linked with the birth process.”
An even more authoritative study, one that is the equivalent of a blue-ribbon panel, is the report issued in 2003 by the American College of Obstetrician and Gynecologists (ACOG) known as the Task Force on Neonatal Encephalopathy & Cerebral Palsy
It stated:
- Since the advent of fetal heart rate monitoring, there has been no change in the incidence of cerebral palsy. . . .
- The majority of newborn brain injury does not occur during labor and delivery
- …. most instances of neonatal encephalopathy and cerebral palsy are attributed to events that occur prior to the onset of labor . . .
This ACOG report was endorsed by six major federal agencies and professional organizations, including the CDC, the March of Dimes and the obstetrical profession in Australia, New Zealand and Canada and is widely regarded as the:
“most extensive peer-reviewed document on the subject published to date”.
A report in Ob.Gyn.News on August 15, 2002, Dr. Hankins, professor and vice chair of Ob-Gyn at the University of Texas, Galveston. stated:
“Performing cesarean section for abnormal fetal heart rate pattern in an effort to prevent cerebral palsy is likely to cause as least as many bad outcomes as it prevents.
… A physician would have to perform 500 C-sections for multiple late decelerations or reduced beat-to-beat variability to prevent a single case of cerebral palsy.
But since Cesarean section carries a roughly 0.5% risk of future uterine rupture, those 500 C-sections would result on average in 2.5 uterine ruptures. This, in turn, would cause one case of neonatal death or cerebral palsy….
So I’ve prevented one case of cerebral palsy and I’ve caused one, concluded Dr. Hankins
Moreover, those 500 women who underwent C-section because of an abnormal fetal heart rate pattern face substantial morbidity related to their surgery, including a 5 to 10 fold increase in relative risk of infection, a 5-fold increase in [blood clots] as well as a 10- to 20-fold increase in future risk of placenta previa and accreta, he added.”
A current EFM textbook for L&D nurses and midwives notes that:
“the greatest misconception about EFM is the belief that it is a diagnostic tool. EFM is useful only as a screening tool”.
[Ref: EFM-Concepts and Applications, Menihan & Kopel, 2nd ed, p. xii, 2008]
- The value of EFM lies in using the information as a question, and not as an answer. Over 90% of fetuses with ‘non-reassuring’ FHR patterns are healthy.
To properly evaluate an abnormal EFM strip, additional medical procedures are needed to determine the significance of this non-reassuring data. These methods include fetal scalp sampling (taking blood from small blood vessels on the unborn baby’s scalp) and fetal scalp stimulation.
However, these additional methods also suffer from serious disagreements between professionals who frequently disagree over the guidelines for use and the validity of the information they provide.
Continue ~ 1D ~ Dark Side of the Moon