 1-B ~ Second half of Overview
1-B ~ Second half of Overview
The Bad Old Days — it’s nobody’s fault but our job — all of us — to fix it
Since 1840, there have been three well-defined, decades-long episodes in which many individuals and groups within the obstetrical profession systematically used, taught and propagated the continuation of poor obstetrical practices that were directly responsible for a substantial increase in maternal mortality and other forms of serious harm to both mothers and babies.
Each of these episodes lasted a minimum of 40 years. During each these 40+ year eras, the obstetrical profession uniformly rejected all attempts to correct obvious problems while the obstetrical profession continued to insist that they were right and everyone else was wrong. In each instance, proponents of these untested obstetrics practices claimed that highly medicalize and interventive practices made pregnancy and childbirth much safer for healthy women with normal pregnancies, therefore it would endanger to do otherwise.
The most important and personally relevant part of the story for Americans is how and why women have been and continue to be harmed by an obstetrically-centric model of maternity care. This unscientific model has been systematically imposing a series of risky, often painful interventions on healthy women since early in the 20th century. A hundred years ago, this long list includes the routine use of Twilight Sleep drugs during labor, general anesthesia, episiotomy, forceps, manual removal of the placenta.
In the 21st century, it includes inductions of labor, the use of Pitocin to speed up labor, having adopted the routine use of continuous electronic fetal monitoring. EFM was developed in the early 1970s to monitor the labors of women with high-risk pregnancies or complications highly risky to unborn babies. But within a few years, it EFM become the obstetrical standard for all laboring women, which includes healthy women with low-risk pregnancies.
For reasons that defy logic, but are 100% consistent with the three historical periods in which “Wrong use of Obstetrics” was used as the standard of care, the continuously and electronically monitoring every pregnant woman, every minute of her labor, has become the universal standard in the US for healthy women with low-risk pregnancies.
The reason was given for the universal use c-EFM is to prevent cerebral palsy and other newborn neurological problems. However, all the studies and randomized controlled prospective trials on the efficacy of electronic monitors since 1975 found that when healthy women with normal pregnancies (70-plus percent of the childbearing population, EFM did NOT prevent CP, or reduce the incidence of perinatal morbidity but it did result in a statistically-significant increase in Cesareans.
One example out of hundreds of published studies was written by an obstetrician for other obstetricians and begins with these startling statements:
- “Intrapartum fetal heart rate monitoring is the most common obstetric procedure performed in the United States.
- Despite the widespread use of EFM, there has been no decrease in cerebral palsy.
- … a meta-analysis of randomized control trials has shown that EFM has no effect in perinatal mortality or pediatric neurologic morbidity.2
- However, EFM is associated with an increase in the rate of operative vaginal and cesarean deliveries.1”
- Although intermittent fetal auscultation {IA} may be a theoretical option in low-risk patients, nursing staffing limitations make this impractical … ”
{Fetal Heart Rate Monitoring Update; The Female Patient, April 2011}
The Most Profound Change in Childbirth Practice in History
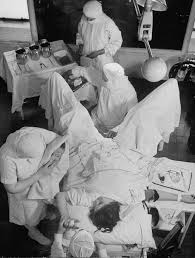 Routinely applying interventionist obstetrics to healthy childbearing women was the most profound change in childbirth practices in the history of the human species.
Routinely applying interventionist obstetrics to healthy childbearing women was the most profound change in childbirth practices in the history of the human species.
When the obstetrical profession implemented their plan to eliminate the traditional form of maternity care in the early 1900s, this was done without having first scientifically tested their theory. No studies were ever conducted that compared outcomes of traditional childbirth practices (physiological management as provided by midwives and many GPs) to the highly medicalized and interventive methods promoted and standardized by the obstetrical profession as the new ‘scientific’ way to have a baby.
Had the scientific method been applied, it would have been instantly obvious that routinely medicalizing labor and birth in a healthy population of childbearing women was not safer or more cost-effective.
The 1910 decision to medicalize normal labor and conduct normal birth as a surgical procedure that has never been reevaluated.
We are now 30 years into the current example of the perennial problem of obstetrics’ shadow-side. The seminal event for the most recent, US-centric episode was a paper published in a highly-respected professional journal (NEJM) in 1984 by two obstetricians. It promoted the idea that “prophylactic” Cesarean surgery should become the new norm for childbirth in the United States. They cited the ‘obvious danger’ of vaginal birth as the reason.
The authors admitted that such a policy would inevitably result in a small number of ‘excess’ maternal deaths as a result of complications from the surgery. However, they rationalized this grim fact by saying that a half-dozen additional maternal death was a small price to pay for saving a much larger number of babies. They also seriously suggested that women who wanted to give birth spontaneously (gulp!) be required to sign a lengthy document listing all the dangers and harm of vaginal birth and releasing their doctor from any subsequent liability.

Whatever the origin or motives that have given rise to this dysfunctional form of maternity care in the US, the routine medical and surgical excesses are bad for both mothers and babies. The simple fact is that over-treatment (or unnecessary and unwanted medical interventions ) in healthy women with normal low-risk pregnancies are not better or safer than under-treatment of patients with medical complications. Both are serious problems and both need to be fixed.
 The safest and best policy is to provide care based on the health status and actual biological and psychological needs of the laboring women. Since 70 to 85% of pregnant women are healthy, the statistically most frequent form of care would be physiologically-based management. This includes the routine use of non-interventive support, and the much safer from of fetal monitoring, which is intermittent auscultation and NOT routinely using continuous EFM.
The safest and best policy is to provide care based on the health status and actual biological and psychological needs of the laboring women. Since 70 to 85% of pregnant women are healthy, the statistically most frequent form of care would be physiologically-based management. This includes the routine use of non-interventive support, and the much safer from of fetal monitoring, which is intermittent auscultation and NOT routinely using continuous EFM.
What I am NOT saying:
What this series of articles does NOT represent is any lack of appreciation or rejection of the right use of modern obstetrics. The role of this surgical specialty is to extend compassionate care to women with childbearing-related reproductive issues — infertility, complications of pregnancy or childbirth or healthy women who simply prefer to be under the care of an obstetrician and have freely, with fully-informed consent, chosen medicalized care relative to their own childbirth.
Why should I care I’m not pregnant (or have a close relative) planning to have a baby soon?
The short answer to the above question is because YOU (and everybody else) is paying for care that is medically unnecessary and actually results in iatrogenic complication that cost a lot of money and often result in preventable deaths and disabilities!
Here is a brief synopsis of what the problem is and how it came about:
The routine medicalizing of normal childbirth began in the early 1900s when a few influential doctors decided that obstetrics should no longer be seen as merely a part of a family doctor’s medical practice. Instead, the “new” obstetrics should be developed into a stand-alone surgical specialty and therefore distinguished from the ordinary maternity care provided by general practice doctors and referred as a ‘man-midwife’.
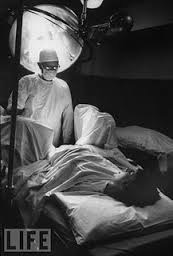 These new rules turned healthy pregnant women into the patients of a surgical specialty and normal childbirth into a surgical procedure performed (only) by physicians on women under general anesthesia.
These new rules turned healthy pregnant women into the patients of a surgical specialty and normal childbirth into a surgical procedure performed (only) by physicians on women under general anesthesia.
The same trend-setting members of the obstetrical profession, in conjunction with organized medicine as a political entity, began to aggressively promote this interventive model of obstetrics all across the US. An accompanying public relations campaign glowingly (and with great frequency) described childbirth under the care of an obstetrically-trained surgeon as the ‘modern’ way to have a baby.
At the same time, they denigrated the traditional model of care for normal labor and birth — physiologically-based management — as old-fashioned, inadequate, unsafe and unpleasant — something that should no longer be tolerated by hip, modern women in the first decades of the brand new 20th century.
In the early 1900s, the country was all abuzz with exciting scientific breakthroughs and riding successive waves of the industrial revolution. This produced, in quick succession, electricity, telephones, air flight, automobiles, vacuum cleaners and the first dishwasher (invented by Lady Astor to keep her maids from breaking the dishes). It seemed that anything ‘modern’ was always better than what went before and that these bright new inventors could do no wrong.
The unexamined perspective of the ‘new’ obstetrics was perpetuated throughout the entire 20th century and deep into the second decade of the 21st century. The current policy of the obstetrical profession is still “full-speed ahead”. But obstetrics is always wrong when it ignores, denigrates or tries to eliminate the normal biology of childbirth by imposing obstetrical procedures indiscriminately on healthy women with normal pregnancies.
The Medical Leadership Council (an association of 2,000 US hospitals) commented on the rising rate C-section rate in 1996, when it was barely 20%. The Council characterized the mounting rate of Cesarean surgery to be:
“medicine’s equivalent of the federal budget deficit; …. long recognized as [an] abstract national problem, yet beyond any individual’s power, purview or interest to correct.”
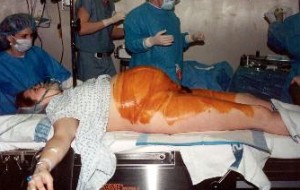 The Cesarean rate in the US is now approximately 33%, and the observation of the Medical Leadership Council couldn’t be more accurate or more chilling: a problem that is “beyond any individual’s power, purview or interest to correct.”
The Cesarean rate in the US is now approximately 33%, and the observation of the Medical Leadership Council couldn’t be more accurate or more chilling: a problem that is “beyond any individual’s power, purview or interest to correct.”
In the hundred years between 1910 and 2010, normal maternity care and normal birth became the domain of a surgical specialty. By 1910, the ‘new’ obstetrics had replaced spontaneous normal childbirth as a biological activity that the mother did under her own power (i.e., giving birth), with vaginal birth as a series of surgical procedures performed by her doctor that included general anesthesia, episiotomy, forceps, manual removal of the placenta and suturing of the perineal wound.
As the surgical procedure of “delivery”, childbirth was something the doctor did, thus making the physician (not the mother) the central actor in the drama of childbirth.
By 2010, many influential and policy-setting obstetricians had successfully invented the newest iteration of the “new obstetrics” by slowly, over a span of 30 years, replacing the idea of vaginal birth itself (biologically normal childbirth) with the notion that all the danger of childbirth could be simply and easily eliminated by making it into a real, sure-enough surgical procedure – Cesarean section.
Cesarean surgery was and continues to be promoted as ‘safer’ or the baby. This means the best way for a woman to give birth is for her NOT to give birth. It also maintains the 1910 idea that the doctor is the central actor in the drama of childbirth and the most important person in the room.
What is “maternity care”, where did it go and why is it different from obstetrics?
The word “maternity” comes from the root “maternal” and logically would describe meeting the needs of mothers, which almost always includes making sure their babies are OK. No mother is happy if her baby is not healthy.
The formal purpose of maternity care is to preserve and protect the health of already healthy women with normal pregnancies. Mastery in normal childbirth services means bringing about a good outcome without introducing any unnecessary harm or unproductive expense. For an essentially healthy population, the most efficacious form of maternity care (safety plus cost-effectiveness) is the model that provides “maximal results with minimal interventions”.
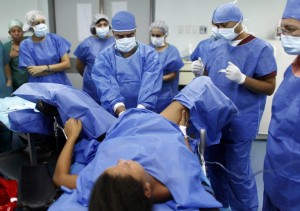 Our present system of obstetrics for normal childbirth does not do this very well. As a surgical specialty, the obstetrical model makes very little distinction between healthy childbearing women and those with complications, as the same surgical standard of care and the same medical interventions and surgical procedures are routinely applied to both.
Our present system of obstetrics for normal childbirth does not do this very well. As a surgical specialty, the obstetrical model makes very little distinction between healthy childbearing women and those with complications, as the same surgical standard of care and the same medical interventions and surgical procedures are routinely applied to both.
 Compared to evidence-based physiological management, medicalized childbirth services that include the preemptive use of obstetrical interventions in a healthy childbearing population introduces the risk of iatrogenic and nosocomial harm was without corresponding benefit. Throughout its history has increased maternal mortality and morbidity.
Compared to evidence-based physiological management, medicalized childbirth services that include the preemptive use of obstetrical interventions in a healthy childbearing population introduces the risk of iatrogenic and nosocomial harm was without corresponding benefit. Throughout its history has increased maternal mortality and morbidity.
“Pit to Distress” as Hospital Policy
A shocking example of this blind spot is what I consider an aberrant and unethical practice referred to as “Pit to distress”, which entails an irresponsible use of the drug Pitocin, an artificial hormone made by Parke-Davis that induces labor or triggers uterine contraction that are much longer and stronger, and closer together, therefore speeding up labor.
 As reported in a Wall Street Journal article [ref: 1] “Pit to distress” is a practice commonly used in hospitals that entails increasingly stronger doses of Pitocin in the laboring woman’s IV until the baby is either blasted out or goes into fetal distress and the doctor performs an emergency Cesarean..
As reported in a Wall Street Journal article [ref: 1] “Pit to distress” is a practice commonly used in hospitals that entails increasingly stronger doses of Pitocin in the laboring woman’s IV until the baby is either blasted out or goes into fetal distress and the doctor performs an emergency Cesarean..
Unfortunately, Pitocin is a potentially dangerous drug that can leads to uterine rupture, fetal distress and even the death of mother or baby. A 2002 article in the professional journal American Family Physician identified 77% uterine rupture rate when Pitocin was given to include or speed up labor in women who previously had a C-section delivery.
What on earth would justify this as a policy or as an individual practice?
How did this happen to smart people like us?
There are two issues here. As a society, we have been actively enculturated for the last hundred years by organized medicine to uncritically accept an unscientific model of obstetrical intervention as the standard of care. Marketing, at least in 20th century American, inevitably entail some form of advertising and/or public relations campaign in order to convince people to do something they otherwise would not have done.
As members of the surgical specialty of obstetrics and gynecology, obstetricians are the primarily attending the births of healthy women with normal pregnancies.
The second part of the problem is an inability or unwillingness by the obstetrical profession in toto to learn from their collective mistakes.
In far too many instances, obstetrical organizations and their members have consistently failed to take corrective action after being provided with corrective information.
 They prefer instead to shoot the messenger.
They prefer instead to shoot the messenger.
Learning about this unfortunate history is quite disturbing. However is a vital part of the political process, as it puts the current politics of organized medicine into its correct perspective. This can help us make the necessary changes to our national maternity care policies that are to the benefit of all — childbearing women and their families, taxpayers, governments, obstetricians, midwives, and the mainstream healthcare system AND it is good for any business that pays its employee healthcare costs.
Everything you always want to know about the economics of the ‘new obstetrics’ but were afraid to ask . . .
Right now we spend 25% of our total healthcare budget on an obstetrically-based maternity care system that primarily provides care to healthy women experiencing a normal biological event. For hospitalized patients, normal childbirth is the single most frequent discharge diagnosis. The second most frequent diagnosis is “healthy newborn baby”.
Out of the approximately 4 million births each year, more than 70% occur to healthy childbearing women with normal pregnancies. This describes the medicalized care of over 8 million mothers and babies annually — twice the number of students that graduate from college every year in the US.
 The United States spends MORE on maternity care than any other country in the world and up to three times more than the five countries with the best outcomes. In spite of all this money, the US ranks a lousy 50th in maternal mortality and about 40th in perinatal outcomes.
The United States spends MORE on maternity care than any other country in the world and up to three times more than the five countries with the best outcomes. In spite of all this money, the US ranks a lousy 50th in maternal mortality and about 40th in perinatal outcomes.
Healthcare dollars spent conducting the labor of healthy women as a potential medical emergency and normal childbirth as requiring a surgical procedure is not available to build a true healthcare system that prevents, protects and preserves the good health of our citizens.
Nor is money available to better treat mild and minor illness and disease so they won’t become major and even terminal ones. It can’t go to health education and other supportive services for patients with chronic diseases so their condition stabilizes, their personal quality of life is improved and lifetime costs associated with their illness are dramatically reduced. All these worthwhile goals can already be achieved, but our sickness-care system is stuck in a crisis-response mode, which means we can’t even imagine a what a rational system would be like and we don’t have the money to search out better, more humane and cost-effective models of care.
Our huge national debt and its deficits are in large part due to the extraordinarily cost of our sickness-care system, which currently includes money spent on highly medicalized obstetrical care for healthy women. As a result, we find ourself rationing many of the true miracles of modern medicine – organ transplants, more effective but expensive cancer treatments, and genomic research. New DNA-based treatments have the potential to totally eliminate certain diseases altogether, cure previously fatal ones and make our pharmaceuticals every so much safer and effective by being individually matched for each patient to our personal genetic profile.
A health-based care system will never bankrupt us. Continuing our 19th-century system of population-based, sickness-oriented medical care into the 21st century will drown the country under useless debt, while people continue to die from lack of access to necessary services. Our s0-called “maternity care” (actually an “obstetrical-care”) system is a BIG part of that problem.
The solution to the looming Medicare disaster is not even on the table because we think we can’t afford to spend the money to make the leap us from our current 19th century, unaffordable sickness-care model to an effective, affordable and humane 21st century model that doesn’t ever have to ration health-related services to any of its citizens.
 We could start today by transforming our national maternity care policies. To reconfigure the system at its most basic and practical level we need a system that provides:
We could start today by transforming our national maternity care policies. To reconfigure the system at its most basic and practical level we need a system that provides:
- Maximal results with minimal interventions
- Skillful use of physiological management
- Adroit use of medical interventions as necessary
- Fewest number of medical/surgical procedures
- Least expense
- Best outcome to for mothers and babies
The form of care recommended by W.H.O. for a healthy population integrates the principles of physiological management with the best advances in obstetrical medicine to create a single, evidence-based standard for all healthy women.
This standard should apply to all categories of birth attendants and in all settings and include the use of standard obstetrical interventions to treat complications or if requested by the mother.
In an evidence-based model, the individual management of pregnancy and childbirth should be determined by the health status of the childbearing woman and her unborn baby, in conjunction with the mother’s stated preferences, rather than the occupational status of the care provider (obstetrician, other MD or midwife).
Never having to choose between a midwife and an obstetrician in order to have a normal childbirth
When these changes are implemented, healthy childbearing women will never again have to choose between an obstetrician and a midwife or between hospital and home in order to receive normal care for normal childbirth. No matter who provides maternity care, they can be confident of receiving appropriate, physiologically-based care for a normal labor and spontaneous birth and having the best obstetrical services if or when they desire or require them. This twenty-first century model of maternity care for healthy women is one that all Americans can be proud of.
A personal note from me:
In revealing the shadow-side of obstetrical history and assigning responsibility in modern times for harmful polices and practices that need to be changed, I am not pointing fingers at obstetricians as individuals. In the first place, they aren’t personally responsible for this miserable history or the contemporary mess it caused. As individuals, obstetricians don’t have any special ability to instantly change the system. In fact, they are very often its victims as well as many others, including midwives like myself and childbearing women who want non-medicalized care for normal childbirth.
Second, I liked my obstetrician, a lovely old-fashioned doctor by the name of Louis Polhman. When I was a 19-year-old bride, he diagnosed me to have Stein-Leventhal ovaries (now called PCOS). It was Dr. Pohlman’s excellent diagnostic and surgical skills that allowed me to become pregnant and eventually give birth to three very appreciated children (and to have two grandchildren).
As a former L&D nurse and now as a professional midwife, I count many obstetricians as long-time treasured friends. I respect and regularly depend on their technical skills whenever the women I provide care to need help with a medical or obstetrical problem. We all benefit from their life-and-limb saving skills and not a one of us wants to go back to the very bad old days before the modern era of scientific medicine.
I know only too well the hazards and potential harm when childbearing occurs without any of the benefits of modern biological science. Whenever and wherever childbearing women have no access to ordinary healthcare and emergent medical services (or husbands, mothers-in-law, uninformed birth attendants, religious beliefs or poverty prevents its timely use), pregnancy and childbirth in even the healthiest of women run the risk of turning into a needless tragedy.
I am not arguing against obstetrical medicine, but rather for the right use of its astonishing abilities. Women like me are asking for recognition of physiologic care as a scientifically-based model that should be a normal part of the mainstream healthcare system. When obstetrical medicine is required or desired, we are asking for a light hand — not too much and not too little, but the just right amount under the right circumstances. This should be determined by the health status of the mother and informed the choice of the childbearing family, rather than the professional politics, economic considerations, and preferences of the care provider. Nothing that purports itself to be a science should rest on the personal preference of its practitioners.
I can only hope that all the wonderful obstetricians that I am personally acquainted with will understand and forgive me if I’ve stepped on some toes. All I can say in my own defense is that I sincerely believe that improving our maternity care system is a good thing — that is, good for ACOG and really good (even great!) for all 40,000 hard-working obstetricians in the US.
I believe Americans are a practical, optimistic and problem-solving nation. With the tools of information and dedication and a willingness to do the hard work, we can and should fix these problems — not in another 20 years, but right now. I invite you to read on and become part of the solution.
Continue to part 2 ~ In the Beginning . . . .
[1] Wall Street Journal ~ New practices reduce childbirth risks Wednesday, July 12, 2006
By Laura Landro
“Pitocin is used like candy in the OB world, and that’s one of the reasons for medical and legal risk,” says Carla Provost, assistant vice president at Baystate, who notes that in many hospitals it is common practice to “pit to distress” [i.e. give progressively larger doses of Pitocin until the mother either delivers or the baby goes into fetal distress].
Intermountain Healthcare says its program has led to a sharp drop in birth complications and decreased the lengths of stay in labor and delivery, cutting costs by $500,000 annually.
However, the new efforts are meeting some resistance from obstetricians, who aren’t used to having their wings clipped. “It has been hard to get doctors to go along because they don’t necessarily believe the risks,” says Ware Branch, who heads Intermountain’s 39-weeks- gestation program.”
Labor Issues – The top six contributors to obstetrics litigation
- Inappropriate use of labor-inducing drugs
- Failure to recognize fetal distress
- Inappropriate use of vacuum/forceps
- Failure to perform timely Caesarean birth
- Failure to properly resuscitate depressed baby
NEXT POST: The story I hate to tell: the dark history of obstetrics (part 2)

